Fear of the unknown is almost always worse than the procedure itself. In my experience, placing implants, most patients tell me afterward that the anticipation was the hardest part – not the surgery. That’s not a sales line. It’s something I hear consistently, and it’s why I want to walk you through exactly what happens at each stage before you’re sitting in the chair, wondering what comes next.
The dental implant procedure isn’t a single appointment. It’s a sequence of stages spread across several months, each with a distinct purpose. Understanding what each stage involves – what we’re doing, why, and what you’ll feel – takes a significant amount of anxiety off the table before you even arrive.
Stage One: Consultation and Imaging
The process begins well before any surgery. At your consultation, we take 3D cone beam imaging of your jaw – a scan that gives us a detailed picture of your bone density, volume, nerve positions, and sinus anatomy. This is where treatment planning actually happens.
Standard dental X-rays show us two dimensions. The 3D scan shows us three. That distinction matters because implant placement requires accuracy around anatomical structures that flat images can misrepresent. We review the scan with you during the appointment so you can see exactly what we’re working with.
By the end of your consultation, you’ll have a clear picture of your candidacy, whether any preparatory procedures are needed, what your timeline looks like, and what the full treatment plan will cost. Nothing gets scheduled until you understand what you’re agreeing to.
Stage Two: Preparatory Procedures (If Needed)
Not every patient needs preparatory work, but when it’s indicated, skipping it compromises the outcome. The most common preparatory procedures are tooth extraction and bone grafting.
Extraction – if the tooth being replaced is still present, it needs to be removed before or during implant placement. In some cases, we can place the implant the same day as the extraction – called immediate implant placement. Whether that’s appropriate depends on the condition of the bone and surrounding tissue at the time of surgery.
Bone grafting – when inadequate bone volume is present to anchor an implant securely, grafting rebuilds the foundation. Grafting material is placed at the site and allowed to integrate with your existing bone over three to six months before the implant is placed. Patients are often surprised that graft sites are less uncomfortable than expected – swelling and soreness for a few days is typical, not extended pain.
If you need preparatory procedures, your timeline extends accordingly. This isn’t a complication – it’s the treatment plan working as intended.
Stage Three: Implant Placement Surgery
This is the stage most patients are apprehensive about, and the one that consistently turns out to be more manageable than expected.
Implant placement is performed under local anesthesia. You will be numb in the area being treated – pressure and movement are normal to feel, but not pain. If you experience anything sharp during the procedure, tell us immediately. That’s what we’re here for.
Here’s what actually happens during the surgery:
- The site is numbed – local anesthetic is administered to the treatment area; this is typically the most uncomfortable moment of the entire procedure
- A small incision is made in the gum tissue – this exposes the bone where the implant will be placed
- A channel is prepared in the bone – using a series of drills at controlled speed and pressure, we create the space for the implant post
- The implant is placed – the titanium post is seated into the prepared channel and positioned precisely according to the treatment plan
- The site is closed – gum tissue is sutured over or around the implant, depending on the surgical approach used
Most single implant placements take between twenty minutes and an hour. You’ll go home the same day. A responsible adult should drive you if sedation was used; local anesthesia alone does not impair driving, but many patients prefer not to drive after any oral surgery.
Post-operative instructions will cover what to eat, how to keep the site clean, and what to watch for. Following them carefully makes a measurable difference in how your recovery goes.
Stage Four: Osseointegration – The Healing Phase
This is the phase that surprises patients most – not because it’s difficult, but because most of the work happens without you feeling it.
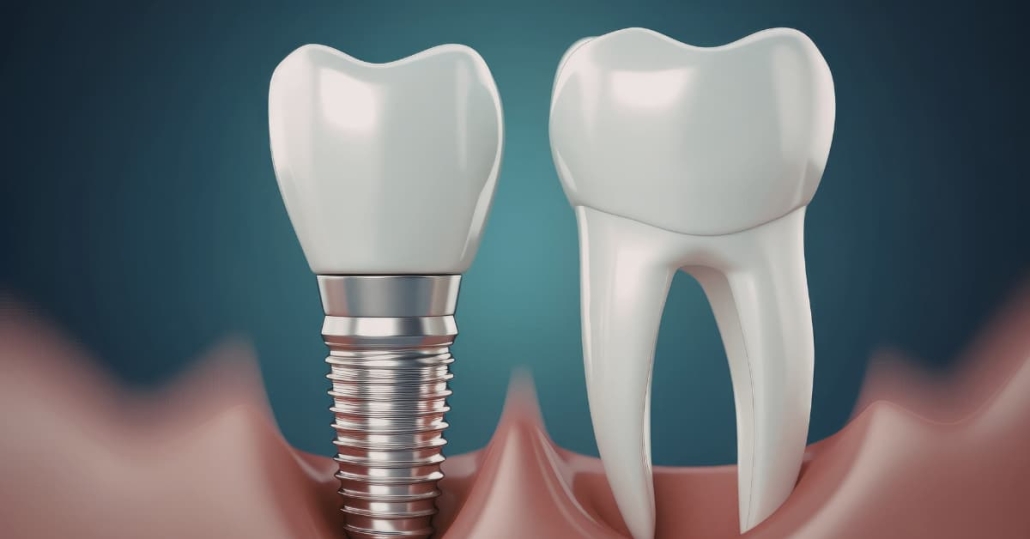
Osseointegration is the process by which your jawbone grows around and bonds with the titanium implant post. Titanium has a unique biological compatibility with bone tissue – the body does not reject it the way it might a foreign material, but instead incorporates it into the bone structure over time.
This process takes approximately three to six months for most patients, sometimes longer depending on bone quality and individual healing. During this period:
- You’ll have a temporary restoration so the gap is covered
- You’ll eat normally with some restrictions on the implant site initially
- We’ll schedule monitoring appointments to check healing progress
- You will not feel the osseointegration happening – it is not painful
This phase requires patience. The timeline is biological, not arbitrary. Placing the final crown before adequate integration would risk the stability of the entire restoration. The wait is doing important work.
Stage Five: Abutment Placement
Once osseointegration is confirmed through imaging, a small connector piece called an abutment is attached to the implant post. This is a minor procedure – often performed under local anesthesia in a short appointment.
The abutment protrudes above the gumline and serves as the attachment point for the final crown. In some cases, the abutment is placed at the same time as the implant; in others, it’s a separate stage. Your treatment plan will specify which approach applies to your case.
After abutment placement, impressions or a digital scan of your mouth are taken so the laboratory can fabricate your crown to the exact dimensions of the space and the shade of your surrounding teeth.
Stage Six: Crown Placement
The final stage is attaching the custom crown to the abutment. By this point, the hard clinical work is done – this appointment is about fit, bite, and aesthetics.
The crown is checked for fit, your bite is assessed to confirm nothing is off, and adjustments are made as needed before the crown is permanently secured. You leave with a complete, fixed tooth.
Most patients describe this appointment as straightforward. There’s something satisfying about it – you’ve been through a process that took months, and this is where it becomes tangible.
Recovery: What to Expect After Implant Surgery
Post-operative experience varies between patients, but there are patterns worth knowing.
Day one and two – swelling peaks in the first 48 hours. Ice packs applied in intervals during the first day help. Soft foods, no straws, and gentle rinsing. Most patients manage with prescribed or over-the-counter pain relief.
Days three through seven – swelling reduces, discomfort decreases. Most patients return to normal activity within a few days. Dissolving sutures typically release within this window.
Week two onward – the surgical site continues healing below the surface. Normal eating and activity resume. The implant site may feel slightly tender when pressed, but should not be acutely painful at this stage. Persistent or worsening pain after the first week warrants a call to us.
Smoking significantly impairs healing and is associated with higher rates of implant complications. If there was ever a medically motivated reason to stop, this is it.
The Role of Maintenance After the Procedure Ends
An implant that goes without regular monitoring is an implant at risk. Peri-implantitis – inflammation of the tissue and bone around an implant – is largely preventable but develops silently if hygiene lapses and professional monitoring is skipped.
Daily brushing and flossing around implant crowns, combined with regular professional cleanings and implant stability checks, are what protect a long-term outcome. The procedure creates the foundation. Maintenance determines what’s built on it.
At monitoring appointments, we assess tissue health, check implant stability, and review bone levels around the post through imaging. Catching early peri-implantitis allows intervention before significant bone loss occurs. Waiting until something feels wrong is often waiting too long.
What Patients Getting Implants Often Worry About Most
After years of these conversations, the concerns I hear most consistently are worth addressing directly.
Pain during surgery – the most common fear, and the one patients most frequently walk back afterward. Local anesthesia means you will not feel discomfort during the procedure. The injection itself can sting briefly. After that, the sensation is pressure – not discomfort. If you ever feel sharp discomfort during surgery, you raise your hand and we stop. That’s the agreement.
The length of the overall process – the timeline is real. Several months from start to finish is not unusual, and for patients who need grafting first, it can be longer. What helps reframe this is understanding that the waiting periods aren’t inconvenient – they’re biological requirements. The bone needs time to integrate. Rushing it risks the outcome.
Whether it will look natural – crowns are fabricated to match surrounding teeth in shade and shape. For front teeth especially, achieving a natural emergence from the gumline is part of the treatment planning process. A well-placed, well-restored implant is typically indistinguishable from a natural tooth.
What happens if it fails – implant failure is uncommon but real, and it’s fair to ask about it. The most common factors associated with failure are smoking, uncontrolled systemic disease, and infection at the surgical site. In most cases, a failed implant can be removed, the site allowed to heal, and a second attempt made after addressing the contributing factors. Failure is not the end of the road in most cases.
Frequently Asked Questions About the Dental Implant Procedure
How long does dental implant surgery take?
A single implant placement typically takes between twenty minutes and one hour. More complex cases involving multiple implants or simultaneous bone grafting take longer. Full-arch procedures are more involved and may take several hours under a deeper level of sedation.
Are you awake during dental implant surgery?
Most single implant procedures are performed under local anesthesia – you are awake but numb. Sedation options are available for patients with significant dental anxiety or for more complex surgical cases. Your comfort level and the scope of the procedure both factor into which approach is appropriate.
How long is recovery after dental implant surgery?
Most patients return to normal activity within two to three days of surgery. Swelling peaks in the first 48 hours and resolves over the following week. Full biological healing – osseointegration of the implant post – takes three to six months, but that process is not painful or disruptive to daily life.
Can the dental implant procedure fail?
Implant failure occurs in a minority of cases. Smoking, uncontrolled systemic conditions, and infection are the factors most commonly associated with poor integration. A failed implant can typically be removed and the process retried after addressing contributing factors. Your surgeon will discuss your individual risk profile during the consultation.
If you’re ready to understand what the dental implant procedure would look like for your specific situation, a consultation at Optima Dental Surgery Center gives you the imaging and clinical assessment to answer that question accurately. We serve patients throughout Austin, Round Rock, and Temple – and we start every consultation with your 3D scan, not a general conversation about general timelines.
This article is intended for educational purposes only and does not constitute medical advice. Individual treatment outcomes vary. Consult with a qualified dental professional to assess whether dental implant treatment is appropriate for your specific situation.