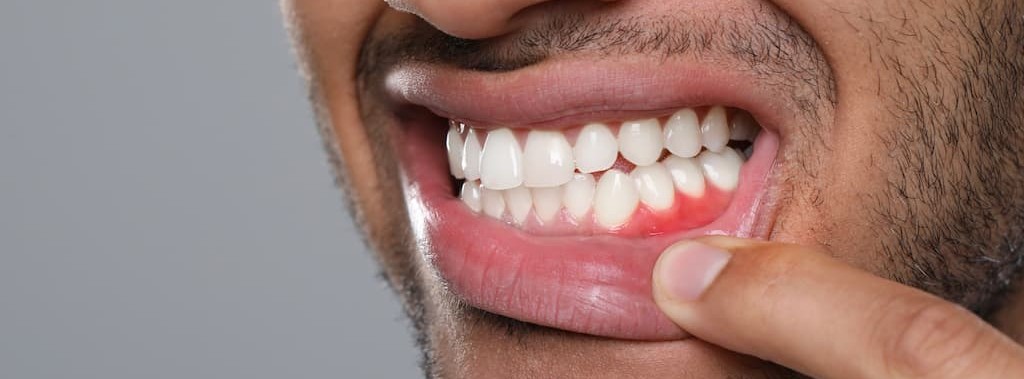
Your doctor mentioned something about your gum health affecting your diabetes control. Or maybe you read an article linking bleeding gums to heart disease and now you’re wondering if there’s really a connection. You brush it off thinking your mouth can’t possibly affect your heart, your blood sugar, or your overall health. These gum disease health effects impact your heart, blood sugar regulation, immune response, and long-term disease risk.
I know this because I’ve sat across from countless patients at Optima Dental Surgery Center who were shocked to learn that their periodontist and their cardiologist were concerned about the same inflammatory process. The bacteria causing your gums to bleed don’t stay confined to your mouth. They enter your bloodstream multiple times daily, and the chronic inflammation they trigger affects your entire body.
What you’re about to read explains exactly how gum disease contributes to serious health conditions like heart disease, diabetes, stroke, and more. I’ll break down the science in straightforward terms and show you why treating periodontal disease is about protecting your overall health, not just saving your teeth.
What the Gum Disease Health Effects Are On Your Entire Body
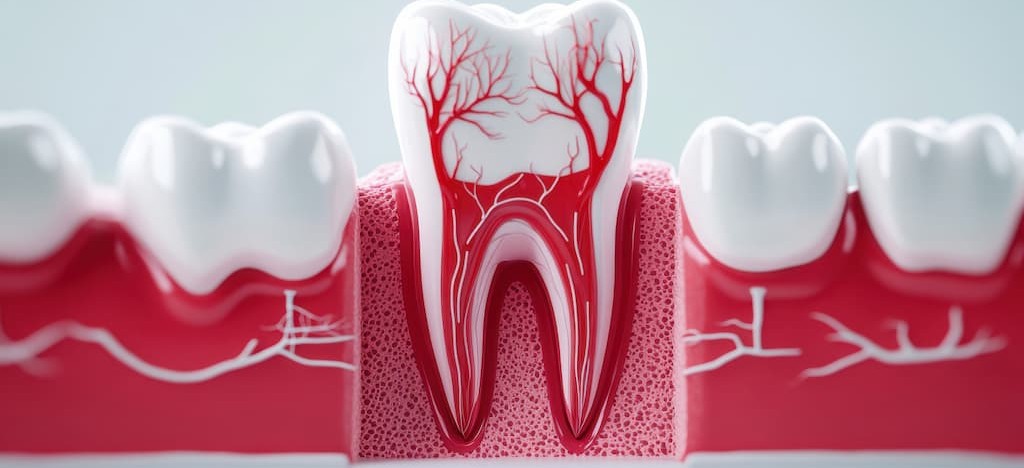
The connection between gum disease and systemic health—and the root of many gum disease health effects—comes down to one word: inflammation. When bacteria accumulate below your gumline, your immune system responds by sending inflammatory chemicals to fight the infection. In healthy gums, this response stays localized and temporary. But with chronic periodontal disease, the inflammation never stops.
Here’s what happens: the bacteria living in deep periodontal pockets trigger a constant immune response. Your body floods the area with inflammatory proteins called cytokines, trying to destroy the infection. These inflammatory markers don’t stay in your gums. They spill into your bloodstream every time you chew, brush, or floss, spreading throughout your entire body.
This constant immune activation explains why gum disease health effects extend far beyond the mouth. Your immune system stays constantly activated, and those inflammatory chemicals circulating through your blood vessels cause damage far from your mouth. The same inflammation that destroys the bone supporting your teeth also damages blood vessel walls, interferes with insulin function, and contributes to disease processes in distant organs.
Gum disease creates systemic problems through three main pathways:
- Direct bacterial invasion: Periodontal bacteria enter your bloodstream during normal activities like chewing food or brushing teeth. These bacteria can colonize in other parts of your body, including your heart valves and arterial plaques.
- Inflammatory chemical spread: The cytokines and other inflammatory proteins your immune system produces to fight gum infection travel throughout your bloodstream, affecting blood vessels, organs, and metabolic processes far from your mouth.
- Chronic immune activation: Your immune system never gets to rest. This constant state of alert damages healthy tissues over time and makes it harder for your body to fight other infections or regulate normal processes like blood sugar control.
This isn’t speculation. Researchers have found the same bacteria that cause periodontal disease living in arterial plaques, heart valves, and other tissues throughout the body. The mouth-body connection is real, measurable, and has serious implications for your overall health.
The Link Between Gum Disease and Heart Health Effects
The relationship between periodontal disease and cardiovascular disease represents one of the strongest and most-studied gum disease health effects in mouth-body research. People with gum disease face a 19% higher risk of cardiovascular disease overall. For adults over 65, that risk jumps to 44%.
The mechanism works like this: periodontal bacteria enter your bloodstream regularly when you have active gum disease. Some make their way to your arterial walls, where they contribute to atherosclerosis – the buildup of plaque inside your arteries. Researchers have found the same bacterial species in arterial plaques that cause periodontal disease.
The chronic inflammation from untreated gum disease weakens blood vessel walls and promotes arterial plaque formation. Those inflammatory chemicals circulating through your system make your blood more likely to clot and your vessels more prone to narrowing.
Here are the cardiovascular conditions with established links to gum disease:
- Coronary artery disease: Periodontal bacteria contribute to arterial blockages that cause heart attacks. The inflammation makes existing plaques less stable and more likely to rupture.
- Stroke: The inflammation from gum disease increases stroke risk by 2-3 times. Weakened blood vessel walls in the brain are more vulnerable to blockage or rupture.
- High blood pressure: Chronic inflammation affects blood vessel function. Studies show that treating periodontal disease can lead to modest blood pressure improvements.
- Bacterial endocarditis: This serious heart valve infection occurs when oral bacteria enter the bloodstream and colonize on damaged or artificial heart valves.
Cardiologists increasingly recognize that managing cardiovascular disease means addressing all sources of chronic inflammation – and gum disease is a significant, treatable source.
The Two-Way Relationship Between Diabetes and Gum Disease Health Effects
The connection between diabetes and gum disease stands apart from other systemic relationships because it works in both directions. Diabetes makes gum disease worse, and gum disease makes diabetes harder to control. This bidirectional relationship creates a vicious cycle that compounds the damage of both conditions.
When your blood sugar runs high, several things happen that favor periodontal bacteria. Elevated glucose in your saliva and gum tissue feeds bacterial growth. Your immune response weakens, making it harder to fight infection. Blood vessels become less efficient at delivering nutrients and removing waste, which slows healing. The result: diabetics develop gum disease more frequently and experience more severe progression.
But here’s what makes this relationship unique—gum disease health effects actively interfere with blood sugar control. The inflammatory response triggered by periodontal infection makes your cells resistant to insulin. Think of inflammation as static on the signal between insulin and your cells. The more inflammation you have, the harder it becomes to regulate blood sugar, even with medication.
This creates a destructive cycle:
- Elevated blood sugar weakens your immune response, making it harder to control the bacterial infection in your gums.
- Gum infection triggers widespread inflammation, which travels through your bloodstream affecting how your body processes insulin.
- Reduced insulin sensitivity drives blood sugar higher, creating more fuel for bacterial growth and further weakening infection resistance.
- Higher blood sugar damages blood vessels, including those in your gums, impairing healing and allowing the infection to progress.
- The cycle continues with each condition worsening the other until both are addressed.
The stakes are serious. Type 2 diabetics with severe periodontitis face 3.2 times higher mortality risk compared to diabetics with healthy gums. But there’s a silver lining: treating gum disease can reduce HbA1c levels by 0.4-0.7%, which represents meaningful improvement in blood sugar control. When diabetic patients commit to treating both conditions simultaneously, they see better outcomes for both.
Additional Health Risks Connected to Gum Disease
Beyond cardiovascular disease and diabetes, research reveals additional gum disease health effects connected to other serious health conditions. While some links are still being studied, the pattern is clear: chronic oral infection affects multiple body systems.
- Respiratory infections: You aspirate small amounts of saliva into your lungs throughout each day. When your saliva contains periodontal bacteria, those bacteria can cause pneumonia or worsen COPD. This risk increases significantly in elderly and hospitalized patients.
- Alzheimer’s disease and cognitive decline: Researchers have found P. gingivalis – a primary periodontal pathogen – in brain tissue of Alzheimer’s patients. The chronic inflammation from gum disease may contribute to inflammatory processes associated with dementia.
- Rheumatoid arthritis: Both conditions involve similar inflammatory markers. People with rheumatoid arthritis have eight times higher risk of severe gum disease. Treating periodontitis in RA patients has shown to reduce arthritis severity in some studies.
- Pregnancy complications: Pregnant women with gum disease face 2-3 times higher risk of preterm birth and low birth weight babies. The inflammatory response can affect placental development and trigger early labor.
- Certain cancers: Chronic inflammation may increase risk for pancreatic cancer and other malignancies, though direct mechanisms are still being established.
- Chronic kidney disease: Inflammation from periodontal disease affects kidney function. Patients with both conditions experience worse outcomes than those with kidney disease alone.
What ties these conditions together? Inflammation. That constant immune activation creates vulnerability across multiple organ systems.
Risk Factors That Multiply the Danger
Some people face compounded risk when gum disease health effects intersect with other health factors. If you fall into these high-risk categories, treating periodontal disease becomes critical for protecting overall health.
- Current smokers: Smoking weakens immune response, impairs healing, and increases inflammation. The combination of smoking and gum disease creates exponentially higher risk for heart disease, stroke, and respiratory problems.
- Adults with diabetes: The bidirectional relationship means each condition worsens the other. Diabetics with untreated gum disease face worse outcomes for both conditions and substantially higher mortality risk.
- People with family history of heart disease: If genetics already elevate your cardiovascular risk, additional inflammation from gum disease compounds that inherited vulnerability.
- Adults 65 and older: Immune function naturally declines with age, making infection control harder. The cumulative inflammatory burden affects overall health more severely.
- Those with existing autoimmune conditions: Your immune system is already overactive. Adding chronic gum infection to that inflammatory load makes managing autoimmune disease more difficult.
- People with limited dental access: Untreated gum disease progresses over years. The longer it goes without intervention, the more severe both oral and systemic effects become.
For these groups, regular dental care is medical necessity that affects survival and quality of life.
Scientific Evidence Behind the Connections

These mouth-body connections—and the resulting gum disease health effects—aren’t theoretical. They’re backed by decades of peer-reviewed research involving hundreds of thousands of patients. The evidence has become strong enough that major medical organizations now acknowledge the relationships and recommend integrated care.
Researchers have found identical bacterial DNA in arterial plaques and infected gums, proving direct migration from mouth to cardiovascular system. Population studies tracking tens of thousands of people over decades show consistent patterns – those with severe gum disease develop cardiovascular disease, diabetes complications, and other conditions at significantly higher rates than those with healthy gums.
Clinical trials demonstrate that treating periodontal disease improves systemic health markers. When patients receive periodontal therapy, their inflammatory markers decrease, blood sugar control improves, and cardiovascular risk factors decline. The intervention affects outcomes beyond the mouth.
Some connections show direct causation – we can trace the bacteria from mouth to disease site. Others show strong correlation through shared inflammatory pathways. Either way, the practical implication remains the same: treating gum disease reduces systemic disease risk.
The American Heart Association recognizes the cardiovascular connection. The American Diabetes Association includes oral health in diabetes management guidelines. Medical and dental professionals increasingly coordinate care because the evidence demands it. Your dentist and your doctor should be talking about your gum health, because it affects conditions they both treat.
Protecting Your Overall Health Through Oral Care
Understanding the gum disease health effects means nothing without action. The good news: periodontal disease is treatable and preventable. Taking control of your oral health directly reduces your systemic disease risk.
Here’s what you need to do:
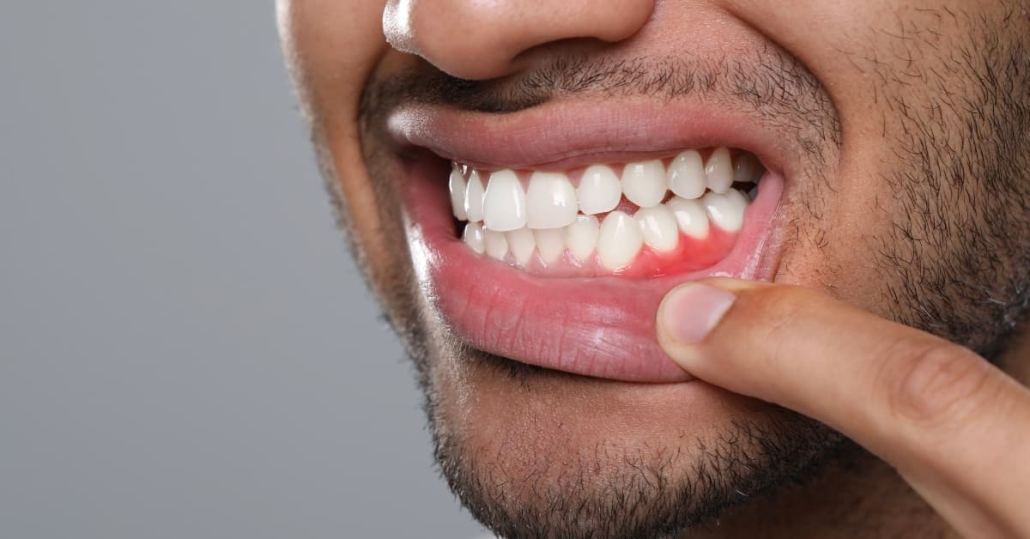
- Get a comprehensive periodontal evaluation if you notice bleeding gums, recession, bad breath, or loose teeth. Don’t wait for your regular cleaning – schedule a focused examination.
- Treat existing gum disease aggressively. This isn’t about aesthetics. You’re reducing inflammation that affects your heart, blood sugar, and overall health. Treatment becomes a medical intervention, not just dental care.
- Maintain regular professional cleanings every three to four months if you have a history of gum disease or are managing diabetes, heart disease, or other chronic conditions.
- Share your complete medical history with your dentist, including all medications, chronic conditions, and recent hospitalizations. Medications like blood thinners and immunosuppressants affect treatment planning.
- Inform your physician about any gum disease diagnosis. They need this information for comprehensive disease management, especially if you’re diabetic or have cardiovascular disease.
- Never skip dental appointments when managing chronic health conditions. Your oral health directly affects your disease control.
- Practice meticulous home care – brushing twice daily for two minutes and flossing once daily without exception. This isn’t negotiable when systemic health is at stake.
Consider your dentist part of your medical team. Coordinate care between your physicians and your periodontist. Address oral health with the same seriousness you apply to blood pressure or blood sugar management.
Learn more about treatment options for gum disease, including root planing and scaling.
Your Mouth and Body Are Connected: Protect Both

Your mouth isn’t isolated from the rest of your body. The bacteria causing your gums to bleed enter your bloodstream. The inflammation destroying bone around your teeth spreads throughout your system. Gum disease is a medical condition with serious gum disease health effects that reach far beyond your teeth.
The connections between periodontal disease and conditions like heart disease, diabetes, stroke, and Alzheimer’s aren’t speculation – they’re established through decades of research. Treating gum disease means reducing your risk for these serious health complications. Preventing gum disease means protecting your overall health.
At Optima Dental Surgery Center, we approach periodontal care as medical treatment, not just dental work. Dr. Owens evaluates how your oral health affects your systemic health and coordinates with your physicians when needed.
If you’re managing diabetes, heart disease, or other chronic conditions – or if you simply want to reduce your disease risk – schedule a comprehensive periodontal evaluation. We’ll assess your gum health, explain any systemic health implications, and create a treatment plan that protects both your mouth and your body.
Frequently Asked Questions About Gum Disease Health Effects
Can gum disease really cause a heart attack?
Gum disease doesn’t directly cause heart attacks, but it significantly increases your risk—one of the most serious gum disease health effects documented in medical research. The bacteria from periodontal disease can colonize in arterial plaques, and the chronic inflammation weakens blood vessel walls and makes existing plaques less stable. People with severe gum disease face 19-44% higher cardiovascular disease risk depending on age. It’s a contributing factor that compounds other heart disease risks.
Should I tell my doctor about my gum disease?
Absolutely. If you’re being treated for diabetes, heart disease, or other chronic conditions, your physician needs to know about active periodontal disease. It affects disease management and treatment outcomes. Many doctors now ask about oral health during routine exams because they understand the systemic connections. Don’t assume they’ll ask – volunteer this information.
Will treating my gum disease help my diabetes?
Yes. Research consistently shows that treating periodontal disease improves blood sugar control in diabetics. HbA1c levels can drop by 0.4-0.7% following successful periodontal treatment. That’s meaningful improvement. The reduction in inflammation helps your cells respond better to insulin. Combined with good diabetes management, treating gum disease gives you better control over both conditions.
How do bacteria from my mouth reach my heart?
Every time you chew food, brush your teeth, or floss, bacteria from your gums enter your bloodstream through inflamed, bleeding tissue. In healthy gums, this bacteremia is minimal and quickly cleared. With gum disease, substantial amounts of bacteria enter your blood regularly. These bacteria circulate throughout your body and can colonize in various tissues, including your heart valves and arterial walls.
Is gum disease dangerous if I’m otherwise healthy?
Even in otherwise healthy people, gum disease creates chronic inflammation that affects your body. While the immediate risk may be lower if you don’t have existing health conditions, you’re still experiencing systemic inflammation that could contribute to disease development over time. Prevention and early treatment protect your long-term health, not just your current state.
What should I tell my dentist about my medical conditions?
Share everything: all diagnosed conditions (especially diabetes, heart disease, autoimmune disorders), all medications including supplements, recent surgeries or hospitalizations, and any upcoming medical procedures. Certain medications affect bleeding and healing. Some conditions require antibiotic prophylaxis before dental procedures. Your dentist needs complete information to treat you safely and effectively.
Can improving my oral health reduce my need for medications?
Possibly, but never stop medications without your doctor’s approval. Some diabetic patients see improved blood sugar control after treating gum disease, which might eventually allow medication adjustments. Some people with high blood pressure see modest improvements. These changes should only be made under physician supervision. Think of oral health improvement as supporting your medical treatment, not replacing it.