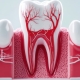
Your gums bleed when you brush. You’ve noticed your teeth look longer than they used to, with recession creeping up that you can’t ignore anymore. Maybe one or two teeth feel slightly loose, and you’re terrified of what that means. Understanding periodontal disease treatment options is often the first step toward stopping damage and saving your teeth. You’re not alone; nearly half of American adults over 30 experience some form of gum disease. Left untreated, it doesn’t stay in your mouth; research links periodontal disease to systemic health effects including heart disease and diabetes complications.
Written by Dr. Kris Owens, DDS, MS, Periodontist at Optima Dental Surgery Center
Dr. Owens is a board-eligible periodontist with advanced specialty training in periodontal surgery, dental implants, and the long-term management of gum disease. Practicing in Round Rock and Austin, he has guided hundreds of patients through every stage of periodontal treatment, from early gingivitis to full-arch reconstruction following advanced bone loss.
I know this because I’ve sat across from hundreds of patients at Optima Dental Surgery Center who waited months or years to address their gum disease, convinced treatment would be painful, complicated, or impossibly expensive. Here’s what I’ve learned: gum disease progresses in predictable stages, and each stage has specific periodontal disease treatment options that can stop the damage and restore your oral health.
What you’re about to read breaks down exactly how periodontal disease develops, from early inflammation to advanced bone loss, and which treatments work at each stage. I’ll explain both non-surgical and surgical options, what to expect during recovery, and how we determine the right approach for your specific situation.
How Gum Disease Progresses and When Periodontal Disease Treatment Becomes Necessary
Periodontal disease doesn’t happen overnight. Knowing the early warning signs of gum disease can mean the difference between a simple cleaning and surgery months down the line. The type of periodontal disease treatment required depends on how far the disease has progressed, and understanding where you fall on this spectrum determines which treatment options will work for you. The earlier we catch it, the simpler and less invasive your treatment can be.
Here’s what happens as gum disease progresses:
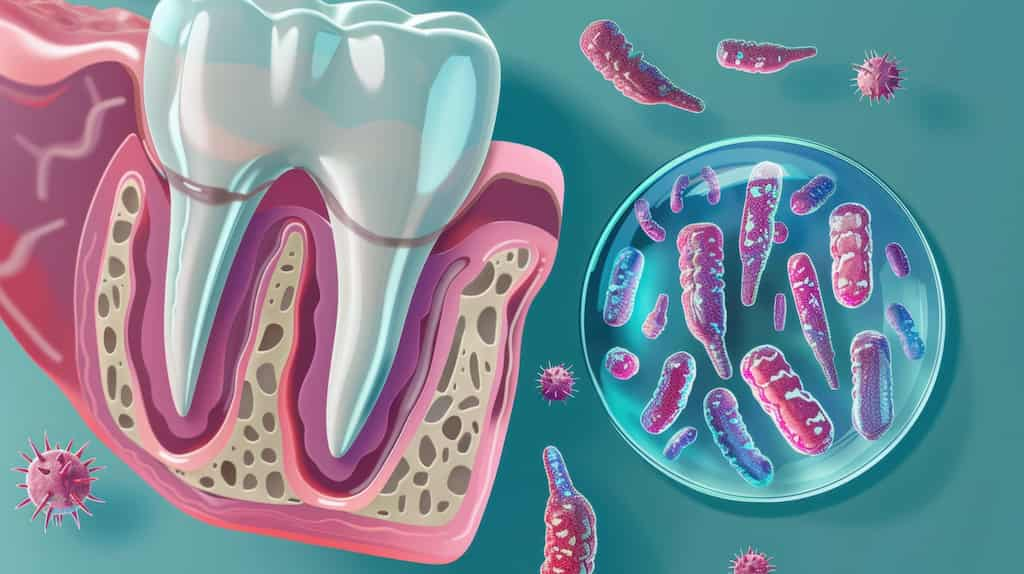
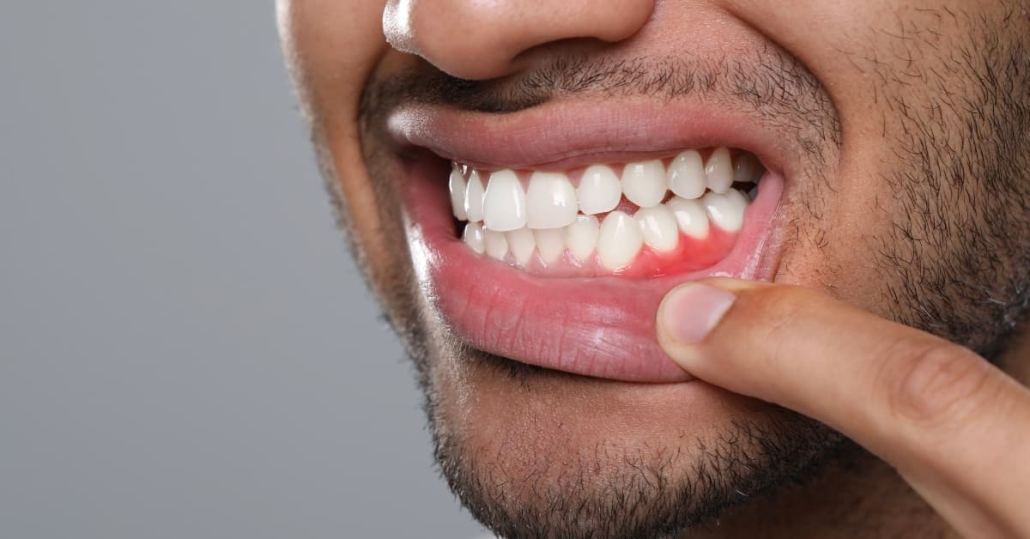
- Gingivitis: The Reversible Stage This is pure inflammation without any permanent damage. Plaque buildup irritates your gums, causing them to bleed when you brush or floss. The good news? At this stage, professional cleaning is often the only periodontal disease treatment needed to completely reverse the condition. No bone loss has occurred yet, and your teeth remain firmly attached.
- Early Periodontitis: When Bone Loss Begins Once bacteria work their way below the gumline, they start attacking the bone that holds your teeth in place. Pockets form between your gums and teeth, typically measuring 4-5mm deep. You might notice persistent bad breath, minor gum recession, or increased sensitivity. This stage requires professional periodontal disease treatment because the damage can’t reverse on its own, though progression can be stopped.
- Moderate Periodontitis: Deepening Destruction Pocket depths increase to 6-7mm, and bone loss becomes more significant. Your gums may pull away from your teeth noticeably, creating that “long tooth” appearance. Some teeth might feel slightly loose. At this stage, you’re at real risk of tooth loss without intervention. Non-surgical treatment might still work, but surgical options become more likely.
- Advanced Periodontitis: Severe Bone Loss This is the stage where teeth become mobile, shifting position or even falling out. Pocket depths exceed 7mm, and more than half the supporting bone may be gone. You’ll likely experience pain when chewing, severe bad breath, and gum abscesses. Treatment at this stage focuses on saving whatever teeth we can while planning for replacement of those too damaged to preserve.
Progression speed varies. Genetics plays a role, but controllable factors matter more: oral hygiene, smoking, diabetes management, and stress levels all influence how quickly the disease advances.
Non-Surgical Gum Disease Treatment Options: When Deep Cleaning Is Enough
If we catch your periodontal disease at the gingivitis or early periodontitis stage, there’s a good chance non-surgical gum disease treatment options will stop the progression and help your gums heal. The primary non-surgical approach is scaling and root planing, essentially a deep cleaning that goes below the gumline to remove the bacteria and calculus causing your inflammation.
For many patients, scaling and root planing is the most effective first-line periodontal disease treatment before surgery is considered. During the procedure, we numb the treatment area to keep you comfortable, then carefully clean the root surfaces of your teeth beneath the gum tissue. This removes the hardened plaque (calculus) that regular brushing can’t reach and smooths the root surfaces so bacteria have fewer places to hide. The procedure typically takes two to four appointments, treating one section of your mouth at a time.
You’ll notice some gum tenderness for a few days after each session, but most patients manage fine with over-the-counter pain relievers. Your gums will feel tighter and healthier within a few weeks as the inflammation subsides and the tissue reattaches to your teeth. We’ll bring you back in about six weeks to measure your pocket depths again and confirm the treatment worked.
Here are the signs you’re a good candidate for non-surgical periodontal disease treatment:
- Pocket depths measure 4-5mm: Deep enough to harbor bacteria but shallow enough for cleaning to reach effectively
- Minimal bone loss on x-rays: Early-stage disease where the supporting structure remains largely intact
- No significant tooth mobility: Teeth are still firmly attached despite the inflammation
- Commitment to maintenance: You’re willing to return every three to four months for professional cleanings and maintain excellent home care
The catch? Scaling and root planing works beautifully for early disease, but it has limits. Once pocket depths exceed 5-6mm or bone loss becomes substantial, we often need surgical access to thoroughly clean the root surfaces and reshape the damaged tissue. That’s not a failure; it’s simply matching the treatment to the severity of the disease.
Surgical Periodontal Treatment: Options Your Austin Periodontist May Recommend
When periodontal disease progresses to moderate or advanced stages, surgical periodontal disease treatment often becomes necessary. I know that sounds intimidating, but surgical treatment gives us direct access to thoroughly clean areas that deep cleaning alone can’t reach, allowing us to rebuild or reshape the damaged tissue supporting your teeth.
Surgical periodontal disease treatment is designed not only to clean infected areas, but also to stabilize teeth and rebuild lost support. The specific approach depends on your pocket depths, bone loss pattern, and treatment goals. Here’s what each option addresses:
- Flap Surgery (Pocket Reduction): This is the most common surgical approach for moderate periodontitis. We lift back the gum tissue to expose roots and bone, thoroughly clean the root surfaces, remove diseased tissue, and reshape irregular bone contours. Then we position the gum tissue snugly against the teeth and suture it in place. Recovery takes about two weeks, and pocket depths typically reduce from 6-7mm down to 3-4mm.
- Bone Grafting: When periodontal disease destroys bone around your teeth, we can rebuild it using grafting material: your own bone, donor bone, or synthetic material. We often combine bone grafting with flap surgery. The graft acts as a scaffold, and over several months, your body replaces it with your own bone tissue. This is particularly valuable for saving teeth with substantial support loss.
- Gum Grafting: Recession exposes your tooth roots, creating sensitivity and increasing your risk of root decay. Gum grafting takes tissue from your palate or uses donor tissue to cover these exposed areas. This protects the roots, reduces sensitivity, and prevents further recession. The procedure also improves aesthetics if recession has created that “long tooth” appearance. Recovery typically takes two to three weeks. For detailed information about what the procedure involves and what to expect week by week, read our complete guide to gum grafting.
- Guided Tissue Regeneration: We place a biocompatible membrane between gum tissue and bone during healing to prevent fast-growing gum tissue from filling the space where bone should regenerate. The membrane gives slower-growing bone cells time to rebuild lost structure. We typically combine this with bone grafting for areas with significant bone loss.
Each surgical option targets specific aspects of periodontal disease damage. Many patients need a combination of these procedures: flap surgery in some areas, bone grafting where support is weakest, and gum grafting where recession is most severe. That’s why the thorough evaluation matters so much.
What Your Austin Periodontist Uses to Build Your Treatment Plan

Periodontal disease treatment isn’t one-size-fits-all, and the right approach depends on several clinical and personal factors. During your consultation at Optima Dental Surgery Center, we gather detailed information to build a treatment plan that addresses your disease severity while respecting your goals and concerns.
Here’s what guides our treatment recommendations:
- Pocket depth measurements: We probe around each tooth to measure how deep the space has become between your gum and tooth. Depths of 1-3mm are healthy, 4-5mm indicate early disease treatable non-surgically, and 6mm or deeper typically require surgical intervention.
- Bone loss severity and pattern: X-rays and CT scans show us how much bone you’ve lost and where. Horizontal bone loss (even across multiple teeth) responds differently than vertical defects (crater-like loss around individual teeth). This determines whether we can save teeth or need to plan for replacement.
- Tooth mobility and prognosis: Some teeth can be saved with treatment, while others have lost too much support. I’ll be honest about which teeth have a good long-term outlook and which might need extraction even with aggressive treatment.
- Overall health and healing capacity: Conditions like uncontrolled diabetes, autoimmune disorders, or smoking can affect both disease progression and surgical healing. We factor this into treatment timing and expected outcomes.
- Your goals and timeline: Are you focused on saving every possible tooth, or are you ready to replace hopeless teeth and move forward? Do you need treatment completed quickly, or can we take a staged approach?
- Cost and insurance coverage: We’ll explain what your insurance typically covers and discuss payment options for any out-of-pocket costs. Treatment decisions should make financial sense alongside clinical sense.
Your consultation includes a complete examination, necessary imaging, and a detailed discussion of your options. No pressure, no surprises. Just clear information to help you make the right choice.
Not sure how far your gum disease has progressed? Schedule a periodontal evaluation with Dr. Owens in Austin or Round Rock; he'll measure your pocket depths, review your X-rays, and walk you through your options with no pressure and no surprises.
Schedule Your Evaluation - (512) 341-2321What to Expect After Periodontal Disease Treatment
Regardless of the approach, successful periodontal disease treatment depends on proper healing and consistent follow-up care. After scaling and root planing, expect some gum tenderness for three to five days. Surgical procedures require longer healing, typically two to three weeks before you feel back to normal, with complete tissue maturation taking three to six months.
You’ll see improvement quickly. Bleeding should decrease within the first week, and swelling subsides within days of surgical treatment. Your gums will gradually tighten and look healthier as inflammation resolves. Most patients tell me they wish they’d pursued treatment sooner once they experience how much better their mouth feels.
The critical point: periodontal disease treatment stops the destruction, but it doesn’t cure the underlying susceptibility. You’ll need ongoing maintenance to keep your gums healthy long-term.
Here’s what maintaining your results requires:
- Frequent professional cleanings: Every three to four months initially, possibly extending to every six months once your condition stabilizes
- Meticulous home care: Brushing twice daily and flossing once daily become non-negotiable, not just recommendations
- Regular pocket depth monitoring: We’ll continue measuring your pockets at each visit to catch any areas showing signs of disease reactivation
- Immediate intervention if problems arise: If you notice bleeding or swelling between visits, call us right away rather than waiting for your next appointment
- Addressing risk factors: If you smoke, quitting dramatically improves your long-term success. Managing diabetes and stress also helps control inflammation
Think of periodontal maintenance as the insurance policy that protects the results of your treatment. The patients who commit to this schedule keep their teeth; the ones who skip it often end up back where they started.
Understanding Periodontal Disease Treatment Costs in Austin
The investment in periodontal disease treatment varies significantly based on disease severity and which procedures you need. As of 2026, scaling and root planing typically costs $200-$300 per quadrant, with full-mouth treatment ranging from $400-$4,000 depending on complexity. Surgical procedures cost more: gum grafting averages $600-$1,200 per tooth, while advanced laser treatments like LANAP range from $1,250-$3,000 per quadrant.
Most dental insurance plans cover periodontal treatment, recognizing it as medically necessary rather than cosmetic. Coverage typically includes 50-80% of the cost after your deductible, though annual maximums usually cap at $1,000-$2,000. Once you reach this limit, additional costs become your responsibility until the next benefit year. We’ll verify your specific benefits before treatment and provide a clear breakdown of your expected out-of-pocket costs.
The cost of periodontal disease treatment reflects not only the procedure itself, but the long-term value of preserving your natural teeth and preventing future tooth loss. At Optima Dental Surgery Center, we work with multiple financing partners to make treatment accessible. Payment plans let you spread the cost over time rather than paying everything upfront.
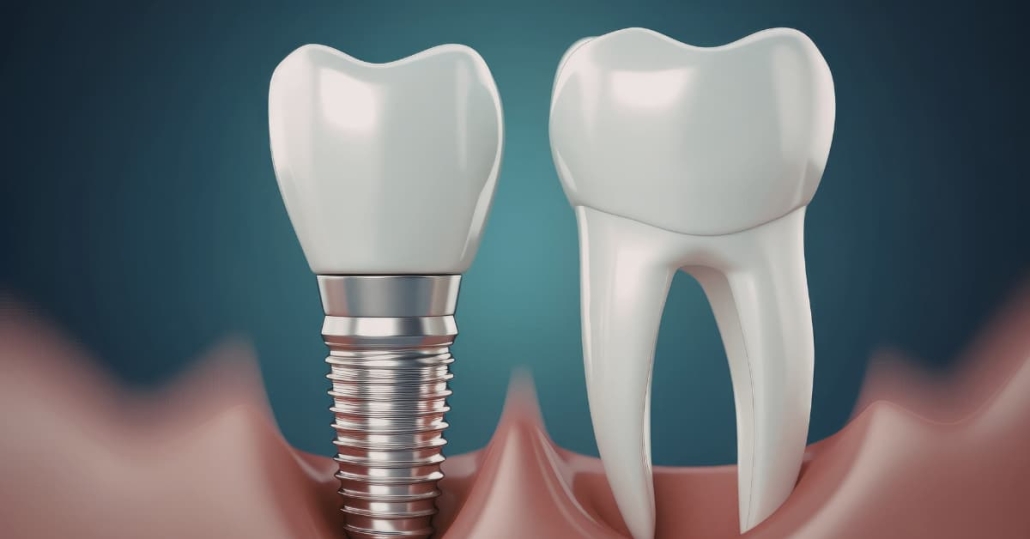
Here’s the financial reality I share with every patient: untreated periodontal disease costs more than treatment, in both dollars and quality of life. Losing teeth to gum disease means facing extraction costs, then the expense of dental implants, bridges, or dentures. A single implant averages around $2,300. Full-arch replacement with systems like Stabili-teeth® runs significantly higher. Treating the disease now prevents those future costs while keeping your natural teeth functioning.
Can You Still Get Dental Implants After Gum Disease?
This is one of the most common questions I hear from patients who are finishing periodontal treatment: “I’ve heard I might need implants someday. Does having gum disease mean I can’t get them?”
The answer is yes: a history of gum disease does not automatically disqualify you from dental implants. But there’s an important condition that must be met first.
Gum disease must be fully controlled before implant placement can happen. Active infection around natural teeth creates the same environment that would attack an implant. We wouldn’t place an implant in a mouth where periodontal disease is still progressing. That’s not a risk worth taking.
What we look for before clearing a patient for implants:
- Stable pocket depths: Measurements that have remained consistent for at least three to six months following treatment
- No active bleeding or infection: Tissues that are firm, pink, and healthy rather than inflamed
- Commitment to maintenance: Patients who keep their three-to-four-month recall appointments demonstrate they can maintain the home care implants require
- Adequate bone volume: Periodontal disease destroys bone, and implants need bone to anchor into. Bone grafting before or at the time of implant placement can address moderate bone loss in many cases
The good news is that many patients who complete periodontal treatment and maintain their results go on to receive implants successfully. The periodontist’s role doesn’t end at gum disease treatment; we coordinate the surgical and restorative phases of implant care for a reason. If you’re wondering whether past or present gum disease affects your implant candidacy, read our detailed breakdown of who qualifies for dental implants and what factors matter most.
At Optima Dental Surgery Center, we treat the gum disease first and then evaluate your candidacy for implants from a position of controlled, stable oral health. That’s the right sequence, and it leads to better outcomes on both sides of the equation.
Ready to Save Your Teeth? Schedule Your Periodontal Evaluation in Austin.
Dr. Owens will assess your gum health, measure pocket depths, and explain exactly which treatment approach can stop your periodontal disease. No pressure, no surprises. Just honest answers about your options.
Contact Us TodayFrequently Asked Questions About Periodontal Disease Treatment
Can periodontal disease be cured or only managed?
Gingivitis can be completely reversed with professional cleaning and improved home care. Once the disease advances to periodontitis and bone loss occurs, that structural damage is permanent, but the disease process itself can be stopped and controlled. Long-term success depends on maintaining the results of treatment through regular professional care. That's why we call it management rather than cure; you'll need ongoing maintenance to keep the disease controlled.
Does periodontal disease treatment hurt?
We use local anesthesia for both non-surgical and surgical procedures, so you shouldn't feel pain during treatment. Afterward, expect some tenderness and discomfort, manageable with over-the-counter pain relievers for scaling and root planing, potentially requiring prescription medication for a few days after surgery. Most patients are surprised by how manageable the recovery is and report far less discomfort than they anticipated before their first appointment.
How long does periodontal disease treatment take?
Non-surgical scaling and root planing typically requires two to four appointments spread over several weeks, with a follow-up evaluation around six weeks after the final session. Surgical treatment depends on how many areas need intervention; some patients complete everything in one session, while others need staged procedures over a few months. Complete healing takes three to six months regardless of the approach, and you'll remain in a periodontal maintenance schedule, typically every three to four months, ongoing after that.
Can I still get dental implants after having gum disease?
Yes; a history of gum disease does not automatically disqualify you from dental implants. The key requirement is that the disease must be fully controlled and stable before implant placement. Active infection or ongoing bone loss creates conditions that would threaten an implant the same way it threatens natural teeth. Once your gum disease is treated, pocket depths are stable, and tissues are healthy, we can evaluate your implant candidacy fully, including whether any bone grafting is needed to restore adequate volume for implant anchoring. Many patients successfully receive implants after completing periodontal treatment.
Will I lose my teeth if I have gum disease?
Not necessarily. Many teeth can be saved with appropriate treatment, even with moderate bone loss. The determining factors are how much support remains, whether you address the disease promptly, and whether you commit to maintenance afterward. Advanced disease may mean losing some teeth while saving others. The earlier you seek treatment, the more options we have, and the better the long-term outcome for the teeth you want to keep.
How often will I need maintenance cleanings after treatment?
Initially, every three to four months. Once your condition stabilizes and pocket depths remain healthy for a year or more, we might extend to every six months. The frequency depends on how your gums respond to treatment and how well you maintain your home care routine. Skipping these appointments is the single most common reason patients see their periodontal disease return after successful treatment.
Does insurance cover periodontal disease treatment?
Most dental insurance plans cover periodontal treatment as a necessary procedure, typically at 50-80% after your deductible. However, most plans have annual maximums of $1,000-$2,000, and many require 6-12 month waiting periods for major surgical procedures. Coverage varies by plan, so we'll verify your specific benefits before beginning treatment and give you an accurate estimate of your out-of-pocket costs. Financing through CareCredit and Cherry is also available for any remaining balance.
What happens if I don't treat my gum disease?
Untreated periodontal disease continues destroying the bone and tissue supporting your teeth. Eventually, teeth become loose and fall out or require extraction. Beyond tooth loss, severe periodontal disease has been linked to increased risk of heart disease, stroke, and complications with diabetes. The bacteria causing the infection can affect your overall health, not just your mouth. Early treatment stops this progression and protects both your smile and your broader wellbeing.