The doubt arrives after weeks of research. Maybe your bone scan shows significant loss, your doctor flagged your diabetes as a potential complication, or you stumbled across something alarming about age cutoffs. Suddenly you're not sure whether dental implants are even realistic for you - and that uncertainty feels worse than the missing teeth themselves.
At Optima Dental Surgery Center in Austin and Round Rock, TX, we evaluate dental implant candidacy daily. What I see repeatedly is that most patients who arrive convinced they don't qualify are wrong about that. The reality is more layered. Yes, specific conditions and anatomical factors affect your candidacy - but the majority of those factors are manageable rather than disqualifying.
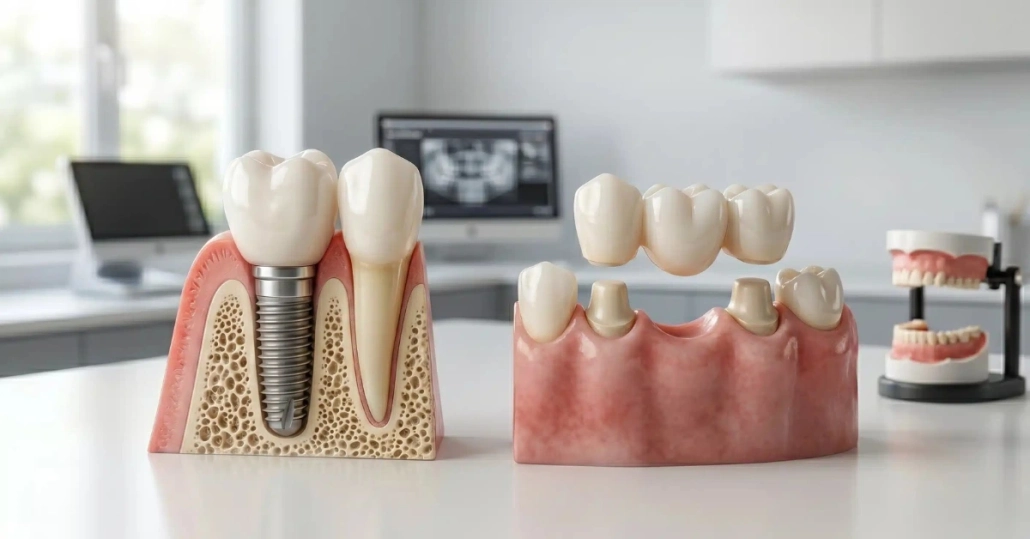
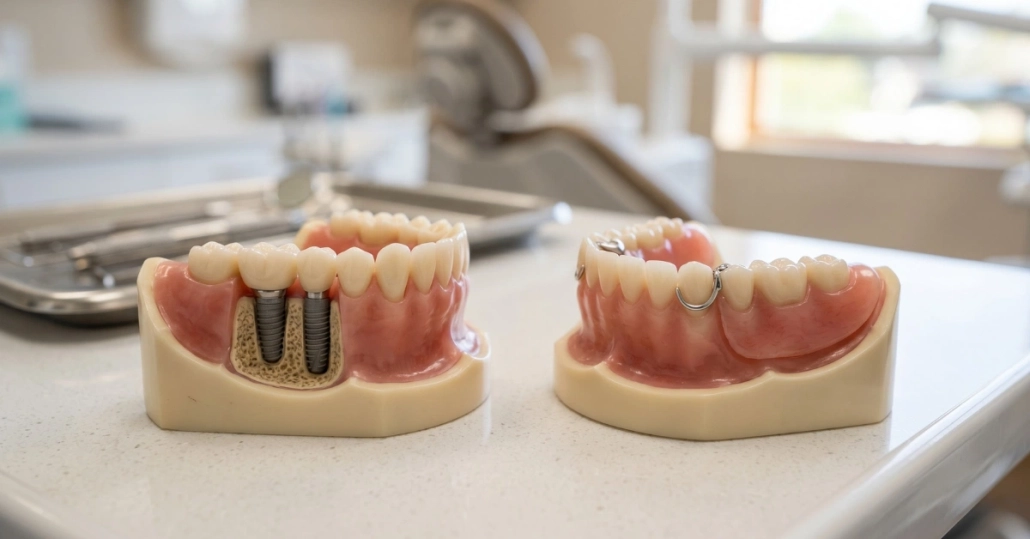
Can anyone get dental implants? Most adults with missing or failing teeth are candidates, either immediately or after preparatory treatment. If you're still comparing your options before deciding, our overview of replacing missing teeth covers the full range of solutions available. What follows is the honest breakdown of what actually determines dental implant candidacy, which health conditions create temporary barriers versus real limitations, and how to figure out exactly where you personally stand.
Success Rate
Success Rate
Candidates
The Core Requirements for Dental Implant Candidacy
Dental implant candidacy isn't a single yes-or-no question. It depends on multiple factors working together. When patients ask whether anyone can get dental implants, these are the requirements that ultimately determine the answer. Meeting all of them creates optimal conditions for success, while gaps in certain areas either prevent placement or require corrective procedures first.
Dental Implant Requirements Checklist
Before moving forward with any treatment plan, here are the foundational dental implant requirements every candidate needs to meet or work toward:
✔ Candidacy Requirements
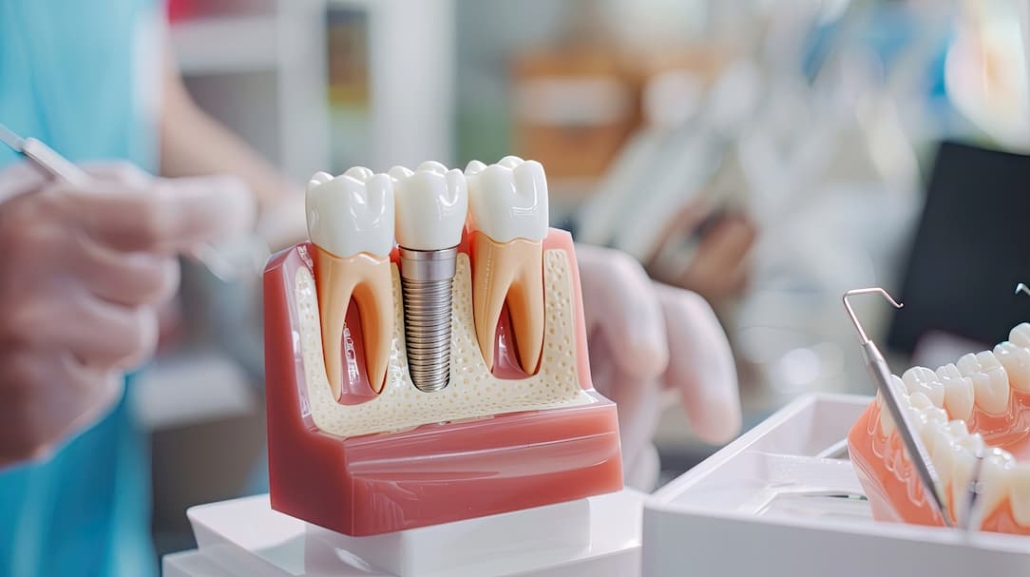
- Adequate bone volume and density — Implants require sufficient bone height, width, and quality for stability. Studies suggest minimum benchmarks of approximately 10mm of bone height and 5mm of width in the lower jaw. Bone must be dense enough to support titanium posts through a process called osseointegration.
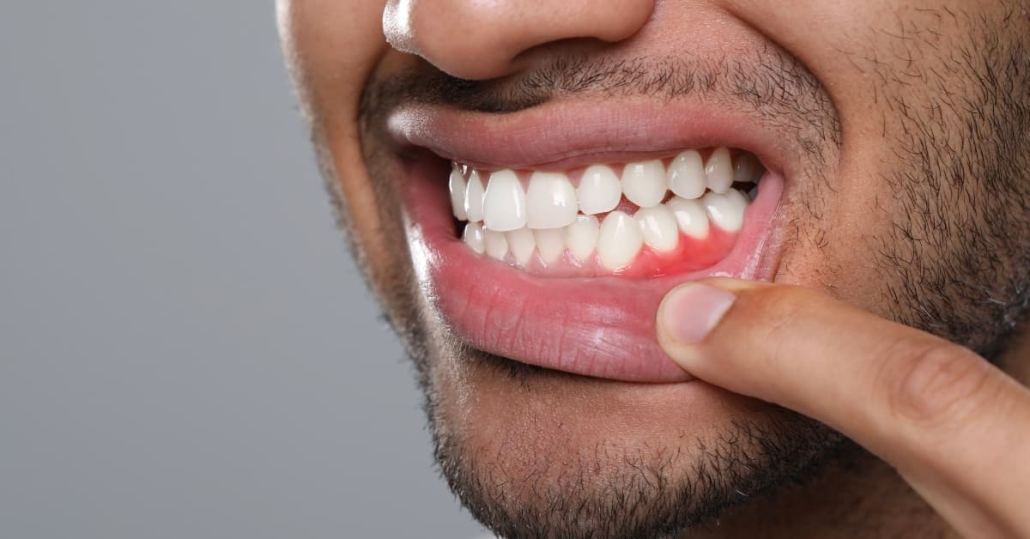
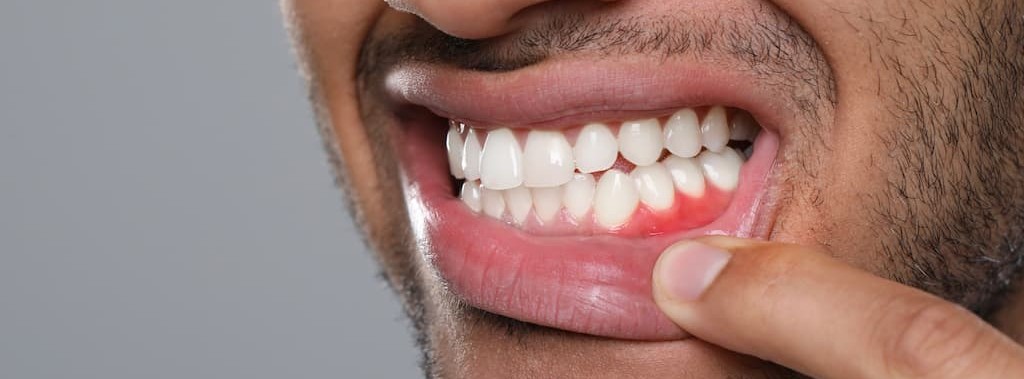
- Healthy gum tissue — Active periodontal disease requires treatment before placement. Healthy tissue provides the biological foundation for long-term success. If you're wondering can you get dental implants with gum disease - not while it's active, but after treatment, most patients qualify.
- Controlled systemic health conditions — Diabetes, autoimmune disorders, and other conditions need medical management to acceptable levels. Uncontrolled systemic disease impairs the healing process that makes implants successful.
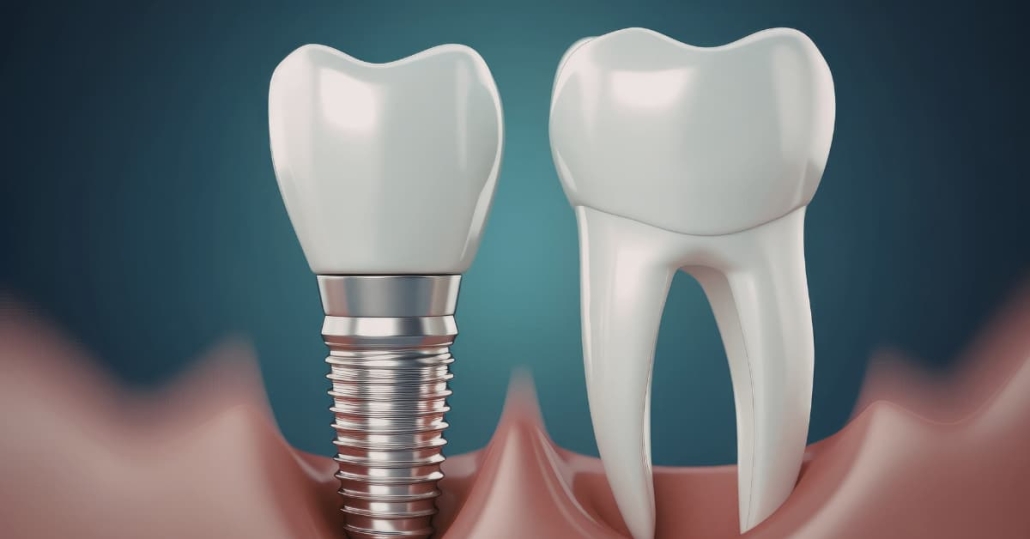
- Functional healing capacity — Your body must successfully integrate titanium with bone through osseointegration. Smoking, certain medications, and prior radiation can impair this process significantly.
- Commitment to oral hygiene — Implants require consistent cleaning and maintenance after placement. Inadequate hygiene increases failure risk from peri-implantitis, a condition that destroys the bone supporting implants.
- Realistic expectations — Understanding the treatment timeline, the maintenance commitment, and the anticipated outcomes matters for long-term satisfaction.
Most candidacy obstacles are correctable. Insufficient bone gets augmented through grafting. Periodontal disease receives treatment before placement. Systemic conditions get optimized through your medical team. The real question for most patients isn't "Can I ever get implants?" but rather "What needs to happen first, and how long will that take?"
Patients with metal sensitivities may also qualify through alternatives - for instance, ceramic implants offer a metal-free option for those who can't receive traditional titanium posts. For patients needing full-arch restoration, All-on-4 dental implants offer a different path when traditional single-tooth placement isn't the right fit. For a deeper look at every full-arch system Optima offers, see our complete guide to full-arch dental implants.
Health Conditions That Affect Dental Implant Eligibility
Certain medical conditions influence implant success rates and healing capacity. This is why the question of dental implant candidacy is less about having a diagnosis and more about how well that diagnosis is managed. The American Academy of Implant Dentistry emphasizes that most systemic conditions are manageable, not disqualifying - and our clinical experience at Optima confirms that consistently.
Diabetes and Dental Implants
Well-controlled diabetes - typically defined as an A1C below 7.0 - generally doesn't prevent implant placement. Research shows success rates for well-managed diabetic patients that are comparable to non-diabetic patients. When A1C climbs above 8.0, medical optimization needs to happen first. That might mean several months of improved glucose management before we proceed - but it's time well spent. Proceeding before adequate control substantially increases failure risk.
Autoimmune Disorders and Implant Candidacy
Conditions like rheumatoid arthritis or lupus can affect healing in certain presentations. Many patients with well-controlled autoimmune conditions successfully receive implants. The key consideration is whether immunosuppressive medications impair healing to a significant degree. We coordinate with your rheumatologist or treating physician to assess that risk and determine appropriate timing.
Osteoporosis and Bone Medications
Osteoporosis itself doesn't prevent dental implants - the condition affects systemic bone density, and dental implant sites can often maintain sufficient local bone quality for successful integration. The greater concern is bisphosphonate medications used to treat osteoporosis. Oral bisphosphonates may require a drug holiday before surgery. Intravenous bisphosphonates need more thorough evaluation due to elevated osteonecrosis risk. This is a conversation that happens directly with your prescribing physician before any surgical planning.
Heart Conditions and Blood Thinners
Most patients on anticoagulant medications can undergo implant surgery without stopping their medications - we modify surgical protocols accordingly. Certain heart conditions require antibiotic prophylaxis before dental procedures. The FDA guidance on dental implants reinforces that proper medical screening before surgery is what makes the difference between safe and unsafe outcomes. Coordination with your cardiologist ensures appropriate management throughout the process.
Cancer Treatment History
Radiation to the head and neck region significantly affects implant success in radiated areas - the reduced blood supply to irradiated bone changes how healing occurs. We typically recommend waiting six months to a year after completing radiation before considering implant placement. Most patients can proceed after chemotherapy completion and adequate recovery. Each case requires individual review of the specific treatment history, dosage, and anatomical location of treatment.
Smoking and Dental Implant Success Rates
Smoking represents the most controllable risk factor that affects dental implant candidacy. Research published in PubMed (PMID 17274726) found implant failure rates of approximately 15.8% in smokers versus 7.3% in non-smokers - roughly double the failure risk. Nicotine impairs circulation, slows tissue healing, and directly compromises the osseointegration process that anchors implants to bone.
Smoking doesn't automatically disqualify you. But cessation for at least two to eight weeks before surgery - and staying tobacco-free through the healing period - is typically required before we proceed. Patients who quit permanently show success rates approaching those of non-smokers. If you smoke and want implants, stopping tobacco use is the single most impactful change you can make.
Controlled Conditions vs. Disqualifying Factors
"Controlled" means the condition is managed to levels that don't significantly compromise healing. For diabetes, that means A1C below 7.0 with stable glucose levels. For autoimmune conditions, it means disease activity is minimal and medication effects aren't severely impairing healing capacity.
Medical clearance from your treating physician documents that your condition is adequately managed for surgical procedures. This clearance isn't administrative paperwork - it's clinical confirmation that proceeding presents acceptable risk given your current health status.
Truly disqualifying factors are rare. Active cancer treatment, severe uncontrolled systemic disease, a recent heart attack or stroke, or a complete inability to heal represent situations where implant surgery isn't appropriate. Even some of these become manageable after adequate recovery time and medical stabilization. The number of patients who are permanently, irreversibly disqualified from dental implants is far smaller than most patients initially assume.
- Well-controlled diabetes (A1C < 7.0)
- Controlled autoimmune conditions
- Osteoporosis (oral bisphosphonates — drug holiday)
- Most heart conditions (modified protocols)
- Smokers (cessation required first)
- Post-chemotherapy (after recovery)
- Active periodontal disease (treat first)
- Active cancer treatment (wait for completion)
- Severe uncontrolled systemic disease
- Recent heart attack or stroke
- IV bisphosphonates (elevated osteonecrosis risk)
- Head/neck radiation (6–12 month wait)
- Complete inability to heal
- Jaw still developing (minimum age)
Active periodontal disease must be treated before implant placement. Treatments like scaling and root planing restore gum health first - then implant eligibility follows. For more advanced cases, laser periodontal therapy offers a less invasive option for clearing infection before implant planning begins. This is a common question we address in consultations, and the answer is consistently the same: treat the disease first, then plan the implants.
Can You Get Dental Implants with Bone Loss?
Insufficient bone volume is the most common candidacy obstacle - and the most correctable one. When a tooth is lost, the surrounding bone begins resorbing immediately. Research published in PMC (Article PMC4934094) indicates that approximately 25% of bone width can be lost within the first year after extraction alone. This is why earlier evaluation is always better than waiting.
Multiple techniques exist to restore bone to levels that support successful implant placement. Bone loss alone rarely means the answer to "can you get dental implants with bone loss" is permanently no. Advanced implant designs like the Zimmer Biomet trabecular metal implant can improve osseointegration in challenging bone conditions - adding more options for patients with compromised bone quality.
Augments areas with inadequate height or width. Graft material integrates over several months, then provides sufficient volume for implant placement. Minor grafting can often happen simultaneously with implant placement.
✓ 85–95% success rateElevates the sinus membrane and places graft material underneath, creating sufficient bone depth in the upper back jaw where the sinus cavity limits available height.
✓ 95%+ success rateRebuilds jaw ridge width using various techniques based on deficiency severity. Most augmentation procedures integrate well within three to six months.
✓ 3–6 month healingLonger implants that anchor in the cheekbone, bypassing areas of severe upper jaw resorption. Allows restoration for patients interested in replacing all upper or lower teeth without the extended grafting timelines that conventional approaches require.
✓ No major grafting neededHow Long Does Bone Grafting Take Before Implants?
Timeline varies based on the extent of grafting required. Minor grafting at the time of implant placement adds little to your overall timeline. Dedicated grafting procedures typically require three to four months of healing before implant placement. Major grafting - ridge augmentation or substantial sinus lifts - may require six months or more before the site is ready. Understanding this upfront prevents frustration with the preparatory phase. The wait is worth it. Proceeding before adequate bone integration compromises the implant from day one.
Are Dental Implants Safe? What the Research Shows
Safety is a legitimate question for any surgical procedure, and dental implants deserve a direct answer. The research is clear: dental implants have a well-established safety record supported by decades of clinical data.
Studies consistently show dental implant success rates between 95% and 98% over a 10-year period when placed by experienced surgeons in appropriately evaluated candidates. The FDA has cleared titanium dental implants as medical devices - the same biocompatible titanium used in orthopedic joint replacements and other long-standing surgical applications. Ceramic implants use zirconia, another well-documented biocompatible material for patients with metal sensitivities.
The risks that do exist are primarily linked to identifiable, manageable factors. Uncontrolled systemic disease increases complications. Active infection at the surgical site affects outcomes. Inadequate bone volume prevents stable osseointegration. Smoking roughly doubles failure risk, as noted above. These aren't random risks - they're predictable variables that thorough pre-surgical screening identifies and addresses before placement.
That's precisely why the evaluation process matters so much. We don't proceed until imaging confirms adequate bone, health status is optimized, and the clinical picture supports a favorable outcome. The patients who experience complications are most often those who received implants without thorough pre-surgical assessment - or those who proceeded before modifiable risk factors were adequately addressed.
When asked are dental implants safe, the honest answer is yes - with the emphasis on "when placed by experienced surgeons following thorough evaluation." The technology is sound. The materials are proven. The success rates are among the highest of any elective surgical procedure in dentistry.
Age Considerations: Dental Implants Age Limit Facts
Age creates candidacy questions at both ends of the spectrum. The answers are more definitive than most patients expect.
There is a minimum age requirement - but it's biological, not arbitrary. Placing implants in a jaw that's still growing creates problems as bone continues developing around fixed implant positions. For most patients, jaw growth completes around age 18 in females and age 21 in males. Younger patients who've lost teeth due to trauma or congenital absence need temporary solutions - bridges, partial dentures, or similar options - until the jaw finishes maturing.
There is no maximum age limit for dental implants. I've successfully placed implants in patients well into their eighties and nineties. Chronological age matters far less than physiological health and healing capacity. An active, healthy 82-year-old with well-controlled health conditions often makes a stronger implant candidate than a 58-year-old with uncontrolled diabetes and poor healing history.
Dental Implant Age Eligibility Spectrum
Minimum age is biological — there is no upper age limit
The question "should a 70-year-old get dental implants?" comes up often. The relevant factors at that age focus on healing ability, systemic health status, and what the treatment investment means relative to the person's quality of life goals. A patient in their seventies or eighties with good health and reasonable life expectancy benefits tremendously from implants - improved nutrition, better confidence, and meaningfully enhanced quality of life during their remaining years.
Older patients sometimes face more extensive bone loss simply due to longer periods of tooth absence. That bone loss responds to grafting just as it does in younger patients. Healing may take slightly longer, but outcomes remain predictable when overall health status is good. The patients I hear most from later are those who wish they'd decided to proceed sooner - not those who regret doing it at all.
The CT Scan Assessment: What It Reveals About Your Candidacy
Three-dimensional CT imaging provides the definitive assessment of your implant candidacy. This scan reveals anatomical detail that clinical examination and standard X-rays simply cannot capture - and without it, any discussion of candidacy is speculation rather than diagnosis.
The scan shows bone quality and quantity in precise, measurable terms. I can evaluate exact bone height, width, and density at each potential implant site - determining whether existing bone is adequate, whether minor grafting at the time of placement will suffice, or whether a staged grafting procedure needs to precede everything else.
Nerve and sinus position mapping prevents serious complications. The CT reveals where the inferior alveolar nerve runs through the lower jaw and exactly how close the maxillary sinuses sit to potential implant sites in the upper jaw. This anatomical information guides surgical planning to protect nerve function and determines whether sinus lift procedures are necessary.
Bone density measurements from the CT predict how well bone will support implants and how quickly osseointegration should occur. Dense bone provides excellent initial stability but may require modified surgical technique. Softer bone requires specific implant designs and sometimes extended healing periods to achieve adequate integration strength.
The scan also guides the decision about which type of implant is most appropriate. It shows whether conventional implants will work, whether angled implants optimize available bone anatomy, or whether alternative approaches like zygomatic implants are the better path. This planning happens entirely before surgery, eliminating surprises and enabling fully informed decision-making.
Online questionnaires and generic candidacy checklists cannot replace this individualized anatomical evaluation. Your specific bone quantity, quality, and anatomical relationships are unique to you - and they determine both your candidacy and your treatment approach in ways that no general assessment can replicate.
Lifestyle Factors You Can Control to Improve Candidacy
While you cannot change your bone anatomy or genetics, several modifiable factors significantly affect both candidacy and long-term success. These changes often matter more than patients initially realize when they're evaluating their options.
These modifications are entirely within your control. Patients who address modifiable risk factors before treatment show substantially better outcomes than those who proceed without optimization. The effort invested before surgery directly protects the investment made during surgery.
Dental Implant Cost and Financial Considerations in Austin
Medical eligibility and financial planning are distinct considerations - but both matter when making this decision, and we address both directly.
Medical qualification determines whether implant treatment can succeed given your anatomy, health, and healing capacity. Financial qualification addresses whether treatment fits your current circumstances and how you'll manage the investment. Meeting medical requirements doesn't guarantee affordability, and having financing available doesn't override medical limitations.
Dental implant cost in Austin, TX varies based on several factors - how many implants you need, whether bone grafting or other preparatory procedures are required, which type of restoration is placed, and which implant system is selected. At Optima Dental Surgery Center, we discuss cost transparently at the start of the process rather than at the end, so you have complete clarity before any commitment is made.
For patients exploring full-arch restoration as an alternative to individual implants, Optima also offers Stabili-teeth® implant-supported dentures - a fixed-arch solution that provides stable results for patients replacing an entire arch. For those comparing removable options, our snap-in dentures guide covers how implant-supported removable options work. Patients comparing full-arch implant systems will also find our All-on-4 vs All-on-6 breakdown useful before booking a consultation.
Dental implant financing in Austin options include payment plans, healthcare credit programs, and various structures that distribute costs over time. These options make treatment accessible to medically qualified candidates who need flexibility in how they manage the investment.
For patients wondering about more affordable options at our other locations, we also serve patients at our dental implants Cedar Park office and additional sites across the Austin metro area.
Some patients medically qualify but decide treatment doesn't fit their current financial priorities. Others discover that preparatory procedures add to the initial estimate they had in mind. These are legitimate and important considerations - separate from whether you can physically receive and maintain implants successfully. Both conversations happen at your consultation, and neither should come as a surprise.
The Consultation Process at Optima Dental Surgery Center
Generic candidacy information helps you understand general requirements. Only individual evaluation determines your specific status and options.
During your consultation with Dr. Faiza Ali, our lead implant specialist, we review your complete medical history, current health status, and medication list. Clinical examination assesses oral health, gum tissue quality, and a preliminary evaluation of bone based on what's visible clinically. CT imaging provides precise anatomical data about bone volume, density, and the critical anatomical structures surrounding potential implant sites.
We discuss your situation directly - whether you qualify now, whether preparatory procedures would make you a candidate, or whether obstacles exist that require a different approach entirely. Nothing is minimized, and nothing is oversold. Our practice model is built on transparency from the first appointment through recovery.
Key questions worth asking at your consultation:
- Do I qualify with my current health status, or do I need preparatory work first?
- What preparatory procedures do I need, and in what order?
- What is the complete treatment timeline from start to final restoration?
- What is the total investment including any grafting or preparatory procedures?
- How do my specific health conditions affect the probability of success?
- What implant options are best suited to my bone quality and anatomy?
The timeline from consultation to completed treatment varies substantially. Straightforward cases may proceed within weeks. Cases requiring bone grafting, health optimization, or medical coordination may span several months before implant placement. Understanding this timeline upfront prevents frustration with necessary preparatory phases - and helps you plan appropriately. Once treatment is complete, our All-on-X aftercare and recovery guide walks you through exactly what to expect post-surgery.
If you're wondering whether you qualify for dental implants, the only reliable way to find out is through a personalized evaluation. Schedule a consultation at Optima Dental Surgery Center to get definitive answers about your candidacy and your options. We also offer wisdom teeth extraction in Round Rock and a range of oral surgery services that support full-scope care planning in the same practice.
Frequently Asked Questions About Dental Implant Candidacy
Can anyone get dental implants, or are some people automatically disqualified?
Very few people are permanently disqualified. Most candidacy issues - bone loss, managed health conditions, smoking history - can be addressed through preparatory treatment or medical optimization. The number of adults who are completely and permanently ineligible is far smaller than most patients assume before evaluation.
Are dental implants safe?
Yes. Dental implants use FDA-cleared biocompatible titanium that has been used safely in medical applications for decades. Studies consistently show success rates of 95-98% over 10 years when placed by experienced surgeons following thorough evaluation. Risks are real but predictable - and proper assessment before surgery identifies and addresses the major ones.
Can you get dental implants with gum disease?
Not during active gum disease. Once active periodontal disease is treated - through scaling and root planing or other appropriate intervention - most patients become eligible for implant placement. The gum tissue and bone must be healthy before implant surgery proceeds.
Who is NOT eligible for dental implants?
True disqualifiers are rare and typically temporary. Active cancer treatment, recent heart attack or stroke, severe uncontrolled systemic disease, or a complete inability to heal represent situations where implants are not appropriate at that time. Most of these conditions can be reassessed after recovery and medical stabilization.
Can anyone get dental implants if they have diabetes?
Patients with well-controlled diabetes - A1C below 7.0 with stable glucose levels - often qualify with success rates comparable to non-diabetic patients. Uncontrolled diabetes requires medical optimization first, which typically means several months of improved glucose management before surgery is appropriate.
Can you get dental implants if you have bone loss?
Bone loss doesn't automatically prevent treatment. Bone grafting, sinus lifts, ridge augmentation, and alternative implant techniques like zygomatic implants can restore eligibility for most patients. The extent of bone loss determines which approach is needed and how long the preparatory phase takes.
Can you get dental implants if you smoke?
Smoking significantly increases failure risk - roughly double compared to non-smokers. It doesn't automatically disqualify patients, but cessation for at least two to eight weeks before surgery and through the healing period is typically required. Patients who quit permanently show outcomes approaching those of non-smokers.
Can anyone get dental implants at an older age?
There is no upper age limit for dental implants. Overall health and healing capacity determine candidacy far more than chronological age. Active, healthy patients in their seventies, eighties, and beyond successfully receive implants regularly at our practice.
Can you get dental implants if you have osteoporosis?
Osteoporosis itself doesn't prevent implants. The primary concern is bisphosphonate medications used to treat it. Oral bisphosphonates may require a drug holiday before surgery, while intravenous bisphosphonates need more thorough assessment due to osteonecrosis risk. This decision happens through coordination with your prescribing physician.
How long does the dental implant process take?
Straightforward cases may be completed in three to six months total. Cases requiring bone grafting, health optimization, or preparatory procedures may span six to twelve months or more before implant placement. Your specific timeline depends on the candidacy factors identified at your evaluation.
What is the dental implant success rate?
Research consistently shows success rates between 95% and 98% over 10 years when implants are placed by experienced surgeons in properly evaluated candidates. Advanced implant designs available at Optima, including the Zimmer Biomet trabecular metal technology, further support osseointegration in cases with challenging bone conditions.
How much do dental implants cost in Austin, TX?
Cost varies based on the number of implants needed, whether bone grafting or preparatory procedures are required, and the type of restoration selected. We provide complete, transparent cost breakdowns at your consultation - including all phases of treatment, not just the implant itself. Dental implant financing plans are available to help manage the investment over time.
If dental implants aren't the right fit, or if you'd like to compare your options, see our full-arch implant candidacy factors guide for more detail on full-mouth restoration pathways.
Can anyone get dental implants? For most adults with missing or failing teeth, the answer is yes - either immediately or with the right preparation. Contact Optima Dental Surgery Center to schedule your evaluation in Austin or Round Rock, TX and get a clear answer about your specific situation.
Find Out Exactly Where You Stand — In One Appointment
CT imaging, a complete candidacy review, and transparent answers about your options. Schedule your consultation in Austin or Round Rock today.
Schedule a Free Consultation