You’re researching full-arch implants but you’re not sure if you qualify. Maybe you’ve worn dentures for years and worry about bone loss. Maybe you have diabetes or osteoporosis and wonder if these conditions disqualify you. Maybe you’re just not sure what makes someone a good full-arch implant candidate versus someone who needs additional preparation or different treatment. I know this uncertainty because Central Texas patients tell me they spend weeks researching before calling, afraid they’ll schedule a consultation only to hear they don’t qualify.
Here’s the reality about full-arch implant candidacy. Most adults with missing or failing teeth can receive full-arch treatment, though some need preparatory procedures like bone grafting before implant placement. The evaluation looks at bone density, overall health, oral health status, and lifestyle factors that affect healing. Some conditions require management before surgery, but few outright prevent treatment – and when they do, alternative solutions usually exist.
This guide walks through every factor that determines full-arch candidacy with honest assessments about what qualifies you, what requires additional work, and what might lead us toward different solutions. You’ll understand the evaluation process, know which medical conditions need addressing, and learn how our Austin-area team determines whether you’re ready for immediate treatment or need preparation steps first. By the end, you’ll know whether to schedule a consultation with confidence or what questions to ask about your specific situation.
Core Requirements for Full-Arch Implant Candidates
Full-arch implant candidacy starts with four fundamental requirements – adequate bone to support implants, healthy oral tissues for healing, general health that supports surgery and integration, and commitment to the treatment process including recovery and maintenance. These requirements apply to every patient regardless of age, dental history, or how long you’ve had missing teeth.
Bone density and volume determine whether your jaw can support implant posts. Full-arch systems need sufficient bone in specific locations – anteriorly where straight implants place and posteriorly where angled implants engage deeper bone structures. You don’t need perfect bone throughout your entire jaw, but you need adequate support in the sites where implants will be positioned. CT scan imaging reveals your bone anatomy with precision, showing exactly what’s available and whether additional bone building procedures might help.
Oral health means freedom from active infections, untreated periodontal disease, or conditions that compromise healing around implant sites. We can treat gum disease before placing implants. We can extract failing teeth during your implant surgery. But active infections need resolution first because placing implants into infected tissue increases failure risk and can spread bacteria into your bloodstream during the procedure.
General health requirements focus on conditions affecting healing and infection risk rather than requiring perfect health. Controlled diabetes works fine – uncontrolled diabetes delays healing and increases complications. Managed osteoporosis rarely prevents treatment – severe untreated bone disease may require medication adjustments. Most medical conditions can be worked with when properly managed, though some require consultation with your physician before proceeding.
Here are the specific factors we evaluate for full-arch candidacy:
- Bone Density in Implant Sites – CT scans measure bone density using Hounsfield units. Density above 250 HU provides good primary stability for implants. Lower density can work with careful surgical technique and possibly extended healing times. Density below 150 HU may require grafting or alternative implant protocols. Most Central Texas patients have adequate density in at least some areas of their jaw.
- Sufficient Bone Volume – Implants need minimum bone height and width for stability. Standard implants require roughly 10mm height and 6mm width, though newer short and narrow designs accommodate less. Severe resorption from years of denture wear sometimes means grafting becomes necessary before implant placement can proceed safely.
- Healthy Gum Tissue – Soft tissue needs to be free from active infection, have adequate thickness to cover implant sites, and possess good blood supply for healing. Thin tissue may need grafting. Infected tissue requires treatment first. Most gum issues can be addressed during treatment planning rather than preventing candidacy entirely.
- Adequate Mouth Opening – Surgery requires access to place implants and attach temporary teeth. Limited jaw opening from TMJ problems or anatomical restrictions can complicate procedures. Severe limitations may prevent proper implant placement, though most patients have sufficient access for standard techniques.
- Realistic Expectations – Understanding that full-arch implants require surgery, healing time, dietary restrictions, and ongoing maintenance helps ensure satisfaction with outcomes. Patients expecting instant perfect results without any discomfort or adjustment period often experience disappointment even when treatment succeeds technically.
- Financial Readiness – Treatment costs $20,000-$35,000 per arch in Central Texas. Financing helps, but you need approval and commitment to payment plans. Starting treatment without financial clarity creates stress that affects your experience and can complicate care if payment issues arise mid-treatment.
- Time Availability – Full-arch treatment takes three to six months from surgery to final restoration. You need availability for surgery day, multiple follow-up appointments, and final teeth placement. Patients with unpredictable schedules or frequent extended travel may struggle with the appointment requirements during the healing period.
Meeting these core requirements doesn’t guarantee candidacy – the medical and lifestyle factors we’ll discuss next play equally important roles. But lacking these fundamentals usually means either preparatory work is needed or alternative treatments make more sense for your situation.
Medical Conditions That Affect Full-Arch Candidacy
Medical conditions rarely prevent full-arch implants outright, but many require management, medication adjustments, or coordination with your physician before proceeding safely. The goal is identifying and addressing health factors that affect healing, infection risk, or long-term implant success rather than simply declining treatment for anyone with medical history.
Diabetes represents the most common medical consideration for full-arch candidates. Controlled diabetes with HbA1c below 7% typically allows normal treatment and healing. Poorly controlled diabetes with HbA1c above 8% increases infection risk and slows healing significantly, often requiring stabilization before surgery. We coordinate with your endocrinologist to optimize blood sugar control, then proceed once your diabetes management reaches appropriate levels. Most diabetic patients in Central Texas successfully receive full-arch implants after proper preparation.
Osteoporosis itself doesn’t prevent implant treatment – the jawbone responds differently to implants than the spine or hips respond to fracture risk. However, bisphosphonate medications taken for osteoporosis can affect jaw healing and increase risk of complications. Oral bisphosphonates usually allow treatment with precautions. IV bisphosphonates may require consultation with your physician about drug holidays or alternative osteoporosis management during the implant integration period.
Here’s how specific medical conditions affect full-arch candidacy:
- Uncontrolled Diabetes – High blood sugar impairs healing, increases infection risk, and can prevent proper bone integration with implants. Candidacy requires diabetes stabilization first. This might mean medication adjustments, dietary changes, or working with your endocrinologist for several months before surgery. Once controlled, diabetic patients often achieve outcomes comparable to non-diabetic patients.
- Autoimmune Conditions – Conditions like rheumatoid arthritis, lupus, or Sjogren’s syndrome can affect healing and infection resistance. Medication management matters more than the diagnosis itself. Some immunosuppressive drugs require timing adjustments around surgery. We coordinate with your rheumatologist to balance disease control with healing requirements. Many autoimmune patients successfully receive implants with proper planning.
- Heart Disease and Blood Thinners – Cardiovascular disease doesn’t prevent implants, but blood thinners like warfarin, Plavix, or newer anticoagulants need management. Some can continue through surgery with precautions. Others require temporary discontinuation with your cardiologist’s approval. We never tell you to stop cardiac medications – that decision comes from your physician based on your specific risks.
- Smoking and Nicotine Use – Smoking significantly increases implant failure risk by constricting blood vessels and reducing oxygen delivery to healing tissues. Candidacy often requires smoking cessation for at least two weeks before surgery and continuing abstinence through osseointegration. Some patients choose to continue smoking and accept higher complication risks. Others use implant treatment as motivation to quit permanently.
- Radiation Therapy to Head or Neck – Previous radiation affects bone healing capacity and increases complications. Timing matters – recent radiation within the past year requires caution and possibly hyperbaric oxygen therapy before implants. Radiation from years ago may have minimal impact depending on dose and location. Each case needs individual assessment based on radiation details and current bone health.
- Bisphosphonate Medications – Oral bisphosphonates taken for less than four years with no other risk factors usually allow treatment. Longer use or IV bisphosphonates increase jawbone complication risk. We coordinate with your physician about drug holidays, alternative bone medications, or proceeding with enhanced precautions depending on your osteoporosis severity and treatment duration.
- Immune Suppression – Organ transplant patients on anti-rejection drugs, chemotherapy patients, or others with suppressed immune systems face higher infection risk. Timing treatment between chemotherapy cycles, coordinating with transplant teams, or adjusting immunosuppression temporarily may allow safe treatment. Each situation requires individual evaluation and coordination with your medical team.
- Bleeding Disorders – Hemophilia, platelet disorders, or other bleeding conditions need hematology consultation before surgery. Factor replacement, platelet transfusions, or other preparations can often allow safe treatment. We work with your hematologist to develop protocols that protect you during and after surgery.
Having one or more of these conditions doesn’t automatically disqualify you from full-arch treatment. It means we need additional information, possibly coordination with your physicians, and careful planning to address the specific challenges your medical history presents. Most patients with managed medical conditions proceed successfully once appropriate precautions are in place.
When Bone Grafting Makes Full-Arch Implants Possible
Inadequate bone doesn’t automatically disqualify you from full-arch implants – it means grafting procedures can build the foundation implants need for long-term stability. Bone grafting adds volume or density to areas where natural bone has resorbed from tooth loss, periodontal disease, or years of denture wear. The procedures extend your timeline and increase investment, but they convert many non-candidates into viable candidates for permanent tooth replacement.
Several grafting techniques address different bone deficiencies. Sinus lifts add bone to the upper posterior jaw when sinus cavities have expanded downward after tooth loss. Ridge augmentation builds width or height in areas where bone has thinned. Onlay grafts place bone material on top of existing bone to increase volume. Socket preservation at the time of tooth extraction prevents bone loss before implant placement. The specific technique depends on where you need additional bone and how much volume must be created.
Grafting materials come from several sources. Autografts use your own bone harvested from another site – this provides reliable results but requires a second surgical site. Allografts use processed human donor bone from tissue banks – this avoids harvesting but relies on your body incorporating foreign material. Xenografts use processed animal bone, typically bovine – this provides a scaffold your bone grows into. Synthetic materials offer alternatives to biological sources. I select materials based on the grafting location, amount needed, and your preferences about graft sources.
Timeline implications matter when grafting becomes necessary. Simple grafting done during implant placement doesn’t extend healing – you follow the standard three-to-six month integration period. Major grafting requiring substantial bone building needs four to six months healing before implant placement, then another three to six months for implant integration. This means final teeth might be twelve months away instead of six. The extended timeline frustrates some patients, but rushing bone integration risks implant failure and potentially losing both the graft and the implants.
Cost considerations affect grafting decisions. Simple grafting adds $500-$1,500 per area to full-arch treatment costs. Major grafting like sinus lifts or significant ridge augmentation adds $2,000-$5,000 per area depending on complexity and materials used. Insurance rarely covers grafting for implants since they classify it as cosmetic rather than medically necessary. The additional investment in grafting protects the larger investment in implants by ensuring adequate foundation for long-term success.
Success rates for grafted implant sites approach those of non-grafted sites when healing proceeds properly. The grafted bone integrates with your natural bone, creating a solid foundation that functions like original bone. Complications can occur – graft failure, infection, inadequate new bone formation – but these remain uncommon when patients follow post-operative instructions and grafts have adequate healing time before implant loading.
Not every bone deficiency requires grafting. Modern implant designs include short implants, narrow implants, and angled placement techniques that work with available bone instead of requiring augmentation. All-on-4 protocols specifically avoid grafting in many cases by using strategic angulation. The decision between grafting, alternative implant approaches, or different treatment options comes from CT scan analysis showing your specific anatomy and discussing priorities around timeline, investment, and long-term stability.
Age Considerations for Full-Arch Implants
Age alone rarely determines full-arch candidacy – bone quality, health status, and healing capacity matter more than your birthdate. I’ve placed successful full-arch restorations in patients from their 30s through their 90s. The youngest candidates need complete jaw development. The oldest candidates need adequate health for surgery and healing. Between these extremes, age becomes just one factor among many in the candidacy evaluation.
Minimum age requirements focus on jaw development rather than arbitrary numbers. Jaw growth typically completes by late teens for women and early twenties for men. Placing implants before growth finishes risks complications as the jaw continues developing around fixed implant positions. Most practitioners wait until age 18-21 depending on growth assessments, though some younger patients with complete development and unusual circumstances receive treatment earlier.
Younger patients often have good bone density and healing capacity, making them strong candidates from a biological perspective. The challenges tend toward financial readiness, lifestyle stability, and long-term maintenance commitment. A 25-year-old with severe dental trauma might be a candidate medically but needs to understand they’re committing to decades of implant maintenance and eventual prosthetic replacements as materials wear over time.
Older patients face different considerations. Bone density may decrease with age, particularly in women after menopause. Healing can slow compared to younger patients. Medical conditions accumulate. But many patients in their 70s and 80s remain good candidates when overall health supports surgery and their bone quality provides adequate foundation. Age-related changes require evaluation rather than automatic disqualification.
The oldest patients I treat successfully are often those most motivated to improve quality of life. They’ve struggled with dentures for years, avoided social situations because of dental embarrassment, or limited their diet to soft foods they can manage. Full-arch implants offer freedom from these limitations during their remaining years. The three-to-six month healing process represents a small fraction of the potentially two to three decades of improved function and confidence they might gain.
Health assessment matters more than age for older candidates. Can you tolerate several hours of surgery under sedation or general anesthesia? Does your cardiovascular system handle the stress of the procedure? Will your bone heal properly given your medical conditions and medications? These questions determine candidacy more than whether you’re 65 or 85. Many healthy older adults proceed successfully while some younger patients with significant medical issues need additional preparation or alternative approaches.
Lifestyle Factors in Full-Arch Success
Lifestyle choices affect full-arch candidacy as much as medical conditions. Oral hygiene habits, smoking status, alcohol consumption, and commitment to maintenance all influence both immediate healing and long-term success. These factors remain within your control, making them opportunities to improve candidacy rather than barriers you can’t change.
Oral hygiene predicts long-term implant health. Patients who couldn’t maintain natural teeth due to poor hygiene often struggle with implant maintenance. Plaque accumulates around implants just like natural teeth, causing inflammation that can lead to bone loss and implant failure. If you’re considering full-arch implants because you “don’t want to deal with dental care anymore,” you may be disappointed – implants require daily cleaning and regular professional maintenance throughout their lifespan.
Smoking remains a significant modifiable risk factor for implant failure. Nicotine constricts blood vessels, reducing blood flow and oxygen delivery to healing implant sites. Studies show smokers have higher implant failure rates than non-smokers. Some practices refuse treatment to active smokers. Others require smoking cessation for defined periods before and after surgery. I discuss smoking honestly during consultation – if you can’t or won’t quit, you deserve to know how this affects your complication risk.
Here are the lifestyle factors that affect candidacy and success:
- Oral Hygiene Commitment – Brushing twice daily, water flossing around implants, and attending professional cleanings every four to six months aren’t optional. Poor hygiene leads to peri-implantitis – inflammation and bone loss around implants that can cause failure years after successful integration. If maintaining this routine feels unrealistic, traditional dentures or other options may serve you better long-term.
- Smoking and Vaping – All tobacco and nicotine products increase complications. Candidacy often includes cessation at least two weeks before surgery and abstinence through the six-month integration period. Some patients successfully receive implants while smoking, accepting higher failure risk. Others can’t or won’t quit and choose different treatment options. Honesty about smoking allows realistic discussion about risks and alternatives.
- Alcohol Consumption – Heavy alcohol use impairs healing, affects medication metabolism, and can indicate compliance concerns. Occasional drinking doesn’t affect candidacy. Regular heavy consumption may require addressing before surgery. Alcohol use disorder needs treatment to support successful recovery from any surgical procedure, including implant placement.
- Medication Compliance – Following post-operative instructions, taking antibiotics as prescribed, and using pain medication appropriately affects healing outcomes. Patients with history of non-compliance with medical instructions face higher complication risks. The implant procedure itself is just the beginning – successful integration depends on your actions during recovery.
- Follow-Up Attendance – Missing post-operative appointments prevents early detection of healing problems. Professional cleanings during integration monitor implant health and remove accumulations you can’t eliminate at home. Patients who struggle attending regular appointments may develop problems that could have been addressed if caught earlier.
- Dietary Compliance – Following dietary restrictions during healing protects temporary teeth and reduces stress on integrating implants. Patients who test restrictions by eating hard foods prematurely risk damage to temporary restorations or stress on implants before bone integration completes. Patience with diet progression supports successful outcomes.
- Financial Responsibility – Maintaining payment plan commitments matters for treatment continuity. Financial stress affects health and healing. Starting treatment without clear financial planning creates complications if payment issues arise before final restoration placement. Honest discussion about costs and payment options prevents problems later.
These lifestyle factors don’t require perfection – they require honest self-assessment and willingness to make changes that support treatment success. Improving oral hygiene before implant placement, quitting smoking permanently, or addressing alcohol issues creates better candidacy and better long-term outcomes regardless of what dental treatment you pursue.
What If You’re Not a Full-Arch Candidate Right Now
Some patients aren’t ready for full-arch implants immediately – active infections need treatment, medical conditions require stabilization, or bone deficiencies demand grafting before implant placement. Not being ready now doesn’t mean never. It means identifying what needs to happen first and creating a path toward candidacy when appropriate.
Preparatory steps address specific barriers to candidacy. Treating periodontal disease eliminates infection and inflammation that would compromise implant integration. Stabilizing diabetes improves healing capacity. Quitting smoking reduces failure risk. Completing bone grafting builds the foundation implants need. These steps take time and often additional investment, but they convert non-candidates into viable candidates for permanent restoration.
Some situations genuinely prevent full-arch implants long-term. Severe medical conditions that can’t be stabilized, inability to tolerate surgery even with sedation or general anesthesia, anatomical limitations that prevent implant placement even with grafting, or unwillingness to commit to required maintenance and follow-up mean alternative solutions serve you better than pursuing implants that might fail or cause complications.
Alternative treatments provide solutions when full-arch implants don’t fit your situation:
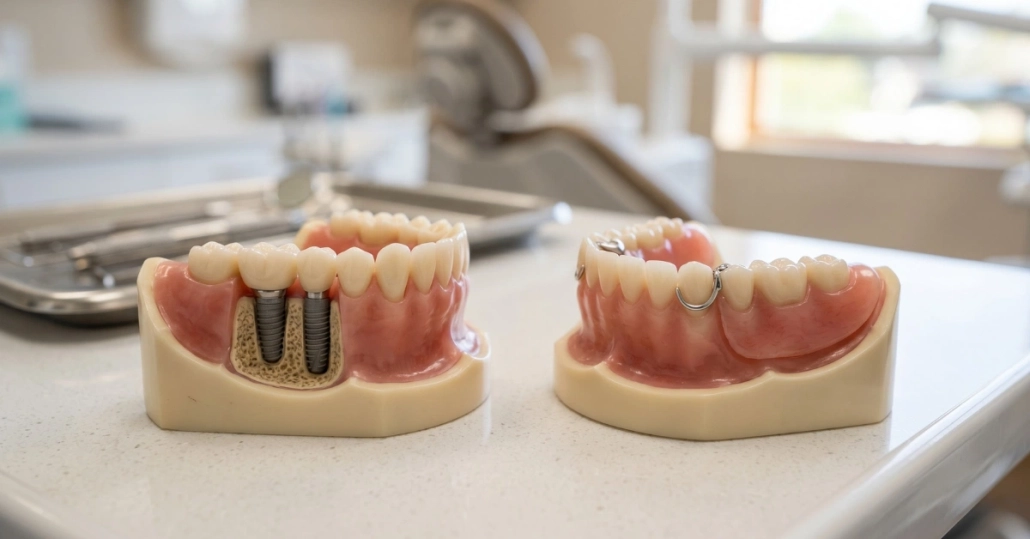
- Traditional Complete Dentures – Removable prosthetics remain the standard solution for complete tooth loss. Modern dentures offer improved aesthetics and fit compared to older designs. They require less investment than implants, need no surgery, and suit patients with medical conditions preventing implant treatment. The trade-offs include reduced chewing efficiency, movement during eating or speaking, and need for adhesives or adjustments as your jaw changes over time.
- Implant-Supported Overdentures – Two to four implants anchor a removable denture, providing stability without the cost or complexity of full-arch fixed restoration. You remove the denture for cleaning but it snaps securely onto implants during wear. This option suits patients with adequate bone for a few implants but insufficient foundation for full-arch treatment, or those preferring removability with improved stability over traditional dentures.
- Partial Solutions – Some patients address their most problematic areas with individual implants or partial restorations while using traditional solutions elsewhere. This allows addressing functional or aesthetic priorities within budget constraints or medical limitations. A few strategic implants can significantly improve denture retention or replace key teeth affecting appearance.
- Staged Treatment – Breaking full-arch treatment into phases spreads costs over time and allows addressing preparation needs before final surgery. Treating periodontal disease first, completing bone grafting with healing time, then placing implants once foundations are ready creates a longer timeline but may be the only path to candidacy for some patients.
Temporary disqualification differs from permanent barriers. If you’re not a candidate now because of uncontrolled diabetes, active infection, or insufficient bone, addressing these issues can open the path to treatment. Working with your physician to optimize diabetes control, completing periodontal treatment to eliminate infection, or undergoing grafting to build bone creates candidacy where it didn’t exist before. The question becomes whether the preparation work makes sense given your overall health, goals, and investment capacity.
How We Determine Your Full-Arch Candidacy
Full-arch candidacy evaluation combines imaging analysis, medical history review, clinical examination, and honest discussion about your goals, expectations, and readiness for treatment. The process takes 45-60 minutes at our Austin-area locations and concludes with clear answers about whether you’re ready for immediate treatment, need preparatory procedures first, or should consider alternative solutions.
CT scan imaging provides the foundation for candidacy assessment. Three-dimensional scans show your bone density, measure available bone height and width in potential implant sites, reveal anatomical structures like sinuses and nerves that affect implant placement, identify existing pathology like cysts or infections, and allow virtual implant positioning to determine if adequate foundation exists. This imaging eliminates guesswork – we see exactly what’s available before making recommendations.
Medical history review identifies conditions affecting healing, medications requiring management, and risk factors for complications. I need complete information about your health conditions, current medications including over-the-counter supplements, previous surgeries or treatments, allergies and adverse reactions, and family history of healing problems. Omitting medical information to appear like a better candidate creates danger – better to address concerns upfront than discover problems during or after surgery.
Clinical examination evaluates your current oral health. I assess gum tissue quality and infection status, check existing teeth for disease or mobility, evaluate your bite and jaw relationship, test mouth opening and jaw function, and identify any oral lesions or abnormalities requiring attention. This hands-on assessment combined with imaging reveals the complete picture of your oral health and treatment needs.
Your goals and expectations matter as much as clinical findings. Understanding why you’re seeking full-arch implants – improved function, aesthetic concerns, denture frustration, or preventing further deterioration – helps ensure treatment aligns with your priorities. Discussing realistic expectations about recovery, timeline to final teeth, maintenance requirements, and long-term outcomes prevents disappointment when reality doesn’t match assumptions.
Financial readiness affects candidacy practically if not medically. Full-arch treatment represents significant investment. We discuss exact costs based on your specific needs, available financing options, timeline for payment, and what happens if complications require additional procedures. Starting treatment without financial clarity creates stress that affects your experience and can complicate care if payment issues arise before completion.
The candidacy discussion follows evaluation completion. For straightforward candidates, I explain which full-arch approach suits your anatomy, what timeline you can expect from consultation to final teeth, what the recovery process involves, and total investment including all components. You leave with clear understanding of your path forward and can schedule surgery once you’re ready to proceed.
For candidates needing preparation, I outline what must happen before implant placement – periodontal treatment, tooth extractions, bone grafting, medical condition management, or lifestyle changes. We discuss timeline for preparation, how it affects overall treatment length, additional costs involved, and whether phased treatment or alternative solutions make more sense given the preparation required. You understand exactly what stands between you and candidacy, how to address it, and whether doing so aligns with your priorities.
For non-candidates or patients where full-arch implants don’t fit your situation, I explain clearly why implants aren’t appropriate and what alternatives might serve you better. This might mean addressing medical conditions before reconsidering implants in the future, pursuing different implant approaches like overdentures, or choosing non-implant solutions that better match your health status, goals, or budget. Honest discussion about limitations prevents pursuing treatment likely to fail or cause complications.
Some evaluations require additional information before reaching conclusions. This might mean consulting with your physician about medical management, getting updated blood work to assess diabetes control, having specific areas examined by a periodontist for treatment planning, or allowing time to see if lifestyle changes like smoking cessation can be maintained. The goal is making informed recommendations based on complete information rather than rushing to conclusions without adequate data.
Take the First Step Toward Candidacy Answers
Full-arch implant candidacy isn’t mysterious – it follows clear criteria based on bone anatomy, health status, oral health, and lifestyle factors. Most adults with missing or failing teeth qualify for some form of full-arch treatment, though many need preparatory work before implant placement. The only way to know definitively where you stand is completing a thorough evaluation with CT imaging and candidacy assessment.
Wondering about candidacy accomplishes nothing. Years pass while you research online, trying to determine if you qualify based on general information that can’t account for your specific anatomy and circumstances. Meanwhile, bone continues resorbing if you’re wearing dentures or have missing teeth. Health conditions may progress. The path to candidacy often becomes more complex the longer you wait to evaluate your situation properly.
Schedule candidacy evaluation at Optima Dental Surgery Center in Round Rock or Temple. We’ll complete CT imaging, review your medical history, examine your oral health, discuss your goals and expectations, and provide clear answers about candidacy. You’ll know whether you’re ready for immediate full-arch treatment, what preparatory steps might be needed, or whether alternative solutions better fit your situation. The consultation fee applies toward treatment if you proceed, making the evaluation a productive first step rather than just information gathering.
The evaluation reveals your specific candidacy factors. Your bone density measurements, anatomical considerations, medical conditions requiring management, and lifestyle factors affecting success. You’ll see your imaging, understand the clinical reasoning behind recommendations, and know exactly what options exist for your situation. No pressure to commit immediately – take time to consider the information before deciding how to proceed.
For Central Texas patients uncertain about full-arch candidacy, the consultation answers questions no amount of internet research can address. Your bone anatomy is unique. Your medical history creates specific considerations. Your goals and expectations guide which approach makes sense. These individual factors determine candidacy more than general information about what typically qualifies someone for treatment.
Some patients attend consultation expecting to hear they don’t qualify, only to learn they’re good candidates ready for immediate treatment. Others assume they’ll proceed quickly but discover preparatory work is needed first. Many fall somewhere between – candidates with minor preparation requirements or factors requiring management but not preventing treatment. The consultation eliminates uncertainty by providing information specific to your situation rather than generalized candidacy criteria.
Call our Round Rock or Temple office to schedule candidacy evaluation. Bring a list of current medications, any recent dental records if available, and questions about full-arch treatment specific to your situation. We’ll address everything during your visit, provide detailed recommendations based on your evaluation, and discuss timing for next steps whether that’s scheduling surgery, beginning preparatory treatment, or exploring alternative solutions. Your candidacy consultation determines whether full-arch implants fit your situation and creates a clear path forward regardless of the answer.