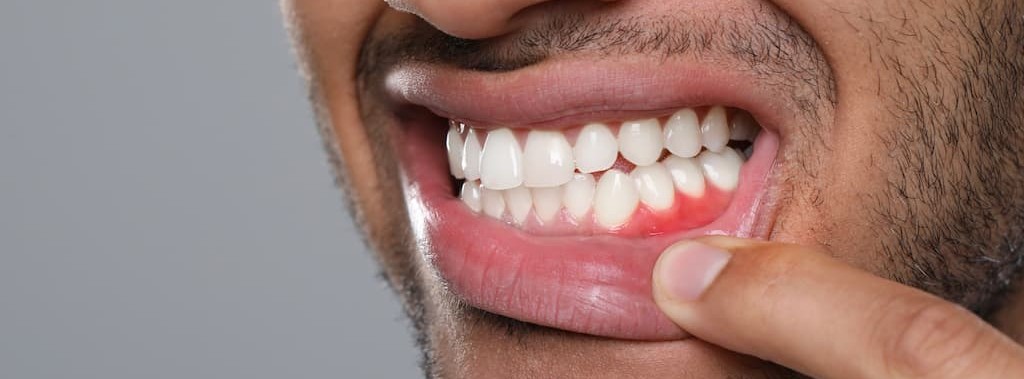
You’ve noticed your teeth look slightly longer in the mirror. Or maybe cold water triggers a sharp sting in one spot when it never bothered you before. You tell yourself it’s normal aging, that everyone’s gums change over time, that it’s probably nothing worth mentioning to a dentist. These early changes are often the first subtle indicators of gum recession developing below the surface.
I know this pattern because most patients with significant gum recession dismissed the early signs for months or years before seeking evaluation. They noticed the changes but rationalized them away until the recession became obvious, the sensitivity became constant, or someone commented on their changing smile. By that point, more tissue has been lost, more root surface exposed, and treatment becomes more complex. This pattern is common because gum recession often progresses slowly and without obvious discomfort at first.
Here are the specific gum recession signs that warrant attention – the visual indicators you can see in the mirror, the physical sensations that signal tissue loss, the progression patterns that help you understand severity, and the timing that determines whether simple monitoring or active intervention makes sense. This isn’t about creating anxiety over minor variations. This is about recognizing legitimate warning signs early enough to protect your teeth and preserve your options for treatment. Early identification of gum recession gives you more control over treatment timing and outcomes.
The Visual Signs Your Gums Are Receding
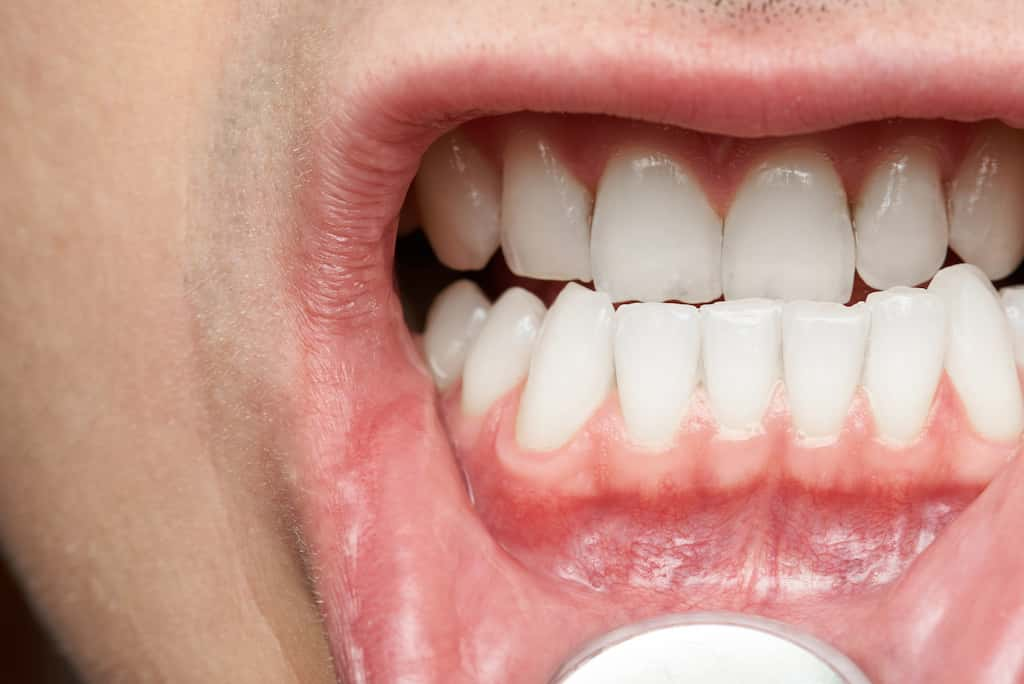
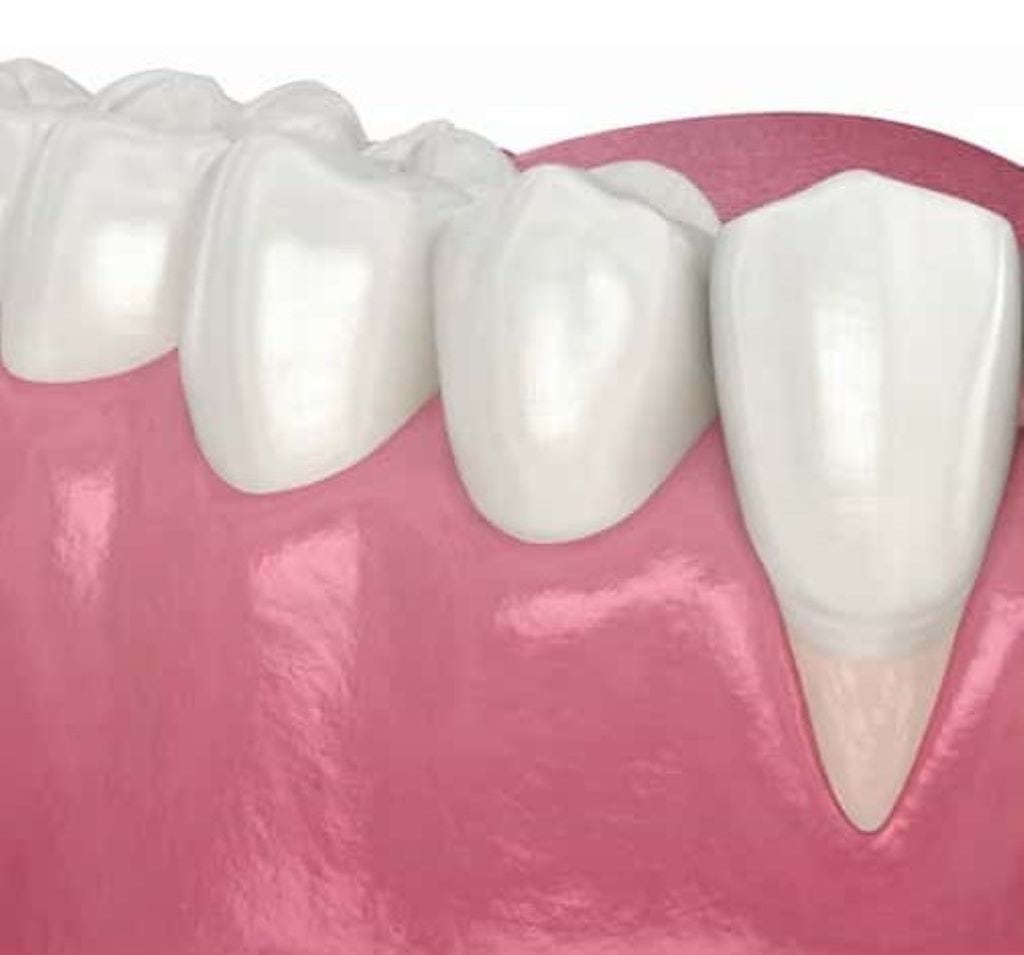
Gum recession creates visible changes you can identify by examining your smile in good lighting. These visual signs of gum recession are often easiest to detect when compared over time. Stand in front of a mirror with natural daylight or bright bathroom lighting and look for these specific indicators:
- Teeth appearing longer than before – recession exposes more tooth structure, making teeth look elongated; compare current appearance to photos from a year ago
- Visible root surfaces – roots appear darker yellow or tan compared to whiter enamel crowns; this color difference marks exposed areas
- Triangular gaps between teeth – dark triangles appear where gum tissue used to fill spaces at the gum line
- Uneven gum line – one tooth shows more root than adjacent teeth; irregular pattern instead of smooth arc
- Notches at gum line – small grooves or wedge-shaped defects where tooth meets gum, often from aggressive brushing
- V-shaped patterns – gum pulls away in sharp V pointing toward root, typically indicating mechanical trauma
- U-shaped patterns – broader, rounded recession suggesting periodontal disease or genetic factors
When several of these indicators appear together, gum recession is often actively progressing rather than stable.
Take photos of your smile from the same angle and distance every few months. Phone cameras work fine – just ensure consistent lighting and positioning. These photos create a visual timeline that reveals changes you might miss in daily mirror checks. Recession happens gradually enough that your brain adjusts to the new normal, making it hard to notice progression without photographic comparison. This type of tracking is especially helpful for identifying gradual gum recession before it becomes severe.
Pay particular attention to lower front teeth and upper canines. These areas show recession most frequently. If you see exposed root surfaces on these teeth, check the rest of your mouth carefully – recession often affects multiple areas simultaneously.
The challenge with visual assessment is distinguishing between stable, long-term recession and active, progressing recession. Both look similar in a single snapshot. That’s why tracking changes over time matters more than evaluating your current state alone.
The Physical Sensations That Signal Recession

Gum recession creates distinctive physical sensations that often appear before visual changes become obvious. These feelings provide early warning signs that tissue loss is occurring. These symptoms frequently accompany early-stage gum recession.
Temperature sensitivity emerges as the most common early indicator. Ice water or hot coffee triggers sharp, immediate stings in specific teeth. This happens because exposed root surfaces lack protective enamel and contain tubules connecting directly to nerves. Sensitivity caused by gum recession often worsens as more root surface becomes exposed.
Brushing sensitivity appears when bristles contact exposed roots. Certain areas hurt when brushed, even with gentle pressure. You start avoiding those spots, creating a cycle – less cleaning leads to more plaque, which accelerates recession.
Rough texture along the gum line becomes noticeable. Running your tongue across teeth reveals distinct textural changes where smooth enamel transitions to rougher root surface.
Food catching in new spaces happens when recession creates gaps at the gum line. Meat fibers and vegetables lodge where they never used to catch.
Early Stage vs Advanced Recession: Understanding Severity
Gum recession severity determines treatment urgency and available options. Accurately measuring gum recession is essential for determining next steps. Understanding these categories helps you assess whether your situation needs immediate attention or periodic monitoring.
Mild Recession (1-3mm) shows slight tooth elongation or minimal root exposure. Sensitivity may be absent or occasional. Often monitored rather than immediately treated unless on front teeth or clearly progressing.
Moderate Recession (3-5mm) displays obvious root exposure with noticeably longer teeth. Darker root surfaces create visible contrast with crowns. Sensitivity is common. Black triangles between teeth appear. This level typically requires intervention.
Severe Recession (5mm+) shows extensive root exposure with teeth appearing twice as long as adjacent teeth. Bone loss accompanies tissue recession. Tooth mobility may develop. Root decay becomes serious concern. Demands immediate attention.
Recession is measured during dental examinations using a periodontal probe – a thin instrument marked in millimeters. The probe measures the distance from where the gum should naturally attach to where it currently sits. This clinical measurement provides objective severity assessment that visual inspection alone can’t deliver. This objective approach ensures gum recession is neither underestimated nor overtreated.
You can estimate severity by looking for the indicators described, but you cannot accurately measure recession at home. Professional assessment with proper measurement tools determines actual severity and appropriate treatment timing. What looks minor to you might measure as moderate recession requiring intervention. What seems severe might be stable, long-standing recession that needs monitoring but not immediate grafting.
The Progression Timeline: How Fast Recession Advances
Recession doesn’t follow a universal timeline. Some patients experience slow progression over many years. Others see rapid advancement within months. Understanding the pace of gum recession helps guide timely intervention.
Slow recession progresses one to two millimeters over several years. You might not notice changes from year to year, but comparing photos from five years apart shows clear tissue loss. This pattern typically occurs with mild mechanical trauma – brushing with moderate pressure using medium bristles – or in patients with genetic predisposition to thin tissue but good oral hygiene habits.
Slow recession still requires monitoring because it will continue unless the causative factors change. The advantage is you have time to address contributing factors and consider treatment options without urgent pressure.
Rapid recession advances multiple millimeters within months to a year. This aggressive pattern usually indicates active periodontal disease, severe mechanical trauma from hard-bristle brushing with excessive pressure, or other significant contributing factors like tobacco use or clenching.
Rapid recession demands immediate intervention. The speed of progression means significant tissue loss occurs quickly, and the window for optimal treatment outcomes closes fast. What starts as mild recession becomes moderate or severe within a year if the causative factors aren’t addressed and the recession isn’t treated.
The “watching and waiting” approach fails with recession because tissue doesn’t regenerate on its own. Once gum tissue recedes, it stays receded unless grafting restores it. Monitoring makes sense only for very mild, stable recession with no symptoms. Active progression or symptomatic recession needs intervention, not observation. For this reason, untreated gum recession leads to cumulative and permanent tissue loss.
Bone loss accompanies significant gum recession. The bone that supports your teeth follows the gum tissue as it recedes. This bone loss is permanent – grafting can restore gum tissue coverage, but lost bone doesn’t fully regenerate. The longer recession continues, the more bone you lose, which compromises long-term tooth stability even after successful grafting. This makes long-term management of gum recession increasingly complex the longer treatment is delayed.
There’s a point of no return where natural restoration becomes impossible. Severe recession with extensive bone loss cannot always be fully corrected, even with grafting. Early intervention preserves more tissue, maintains more bone, and achieves better long-term outcomes. Waiting until recession becomes severe dramatically limits what treatment can accomplish.
Common Patterns and Where Recession Starts
Recession follows predictable patterns based on tooth anatomy, position, and the forces acting on gum tissue. These patterns explain why gum recession often appears first in predictable areas. Knowing these common locations helps you target your self-examinations effectively.
Lower front teeth show recession most frequently – they sit in thin bone with naturally thin tissue coverage. Check these first during self-examination.
Upper canines and premolars rank second for recession, experiencing significant chewing force and often positioned where tissue is thinner.
Aggressive brushing areas develop V-shaped patterns from mechanical trauma. Typically affects one or two adjacent teeth while surrounding teeth remain unaffected.
Thin tissue biotype affects patients with delicate, almost translucent gum tissue. These patients develop recession more readily than those with thick, dense tissue.
Teeth outside bone envelope lack adequate coverage when positioned too far forward. Recession is nearly inevitable without sufficient tissue foundation.
Risk Factors That Accelerate Recession

Multiple factors contribute to gum recession. In most cases, gum recession develops from multiple overlapping causes rather than a single issue. Identifying which ones affect you helps explain why recession is occurring and what you can modify to slow progression.
- Brushing technique and pressure – scrubbing with hard or medium bristles using horizontal strokes wears away tissue over time; excessive pressure damages delicate gum margins even with soft bristles; proper technique uses gentle circular motions with soft bristles and minimal pressure
- Periodontal disease presence – bacterial infection destroys the connective tissue fibers and bone that support gums; inflammation from chronic disease causes tissue breakdown and recession; untreated periodontal disease is the leading cause of widespread recession affecting multiple teeth
- Genetic predisposition to thin tissue – some people inherit thin, delicate gum tissue that recedes more easily regardless of oral hygiene quality; you can’t change genetics, but knowing you have thin tissue helps you take preventive measures and monitor closely
- Grinding and clenching habits – bruxism creates excessive force on teeth that damages the thin tissue at the gum line; this mechanical stress causes inflammation and tissue breakdown; the constant pressure can also shift teeth into positions with inadequate tissue coverage
- Tobacco use impact – smoking and chewing tobacco restrict blood flow to gum tissue, impair healing capacity, and increase susceptibility to periodontal disease; nicotine constricts blood vessels, starving tissues of oxygen and nutrients needed for health
- Aging and hormonal changes – tissue naturally becomes thinner and less resilient with age; hormonal fluctuations during pregnancy, menopause, and other life stages affect tissue quality and inflammation levels; these factors don’t cause recession directly but increase vulnerability
- Oral piercings and mechanical trauma – lip or tongue jewelry creates constant friction against gum tissue; the repetitive contact wears away tissue around specific teeth; removing piercings often stops progression but doesn’t reverse existing damage
Most recession results from multiple factors working together rather than a single cause. You might have thin tissue genetics, brush with moderate pressure, and grind your teeth at night. Each factor alone might not cause severe recession, but the combination accelerates tissue loss.
Addressing modifiable risk factors slows recession progression. Switching to an electric toothbrush with pressure sensors prevents brushing trauma. Treating periodontal disease stops inflammation-driven tissue loss. Wearing a nightguard protects against grinding damage. Quitting tobacco improves tissue health and healing capacity. These steps are critical for slowing gum recession and preserving remaining tissue.
You cannot control genetic predisposition or reverse aging effects, but you can minimize other contributing factors to slow recession and preserve the tissue you have. Even if grafting becomes necessary, controlling risk factors improves graft success rates and long-term stability.
When to Seek Evaluation: The Timing That Protects Your Teeth
Knowing when recession requires professional assessment versus simple monitoring prevents both unnecessary anxiety and dangerous delays. Prompt evaluation prevents gum recession from advancing beyond treatable stages.
Seek immediate evaluation if you notice:
- New sensitivity that localizes to specific teeth – sudden cold or hot sensitivity in one or two areas that wasn’t present a few months ago signals recent tissue loss exposing roots
- Visible root surfaces on front teeth – any exposed root on teeth that show when you smile warrants evaluation for both functional and aesthetic reasons
- Progression you can confirm with photos – comparing pictures from six months or a year apart that show clear changes in gum position means active recession requiring intervention
- Moderate to severe recession – significant root exposure, teeth appearing noticeably longer, or multiple millimeters of tissue loss needs assessment regardless of symptoms
Schedule evaluation within a few months if you have mild, stable recession without symptoms but want professional measurement and monitoring protocols established. Annual dental checkups often catch these cases, but if you notice changes between regular visits, contact the office rather than waiting.
Earlier intervention provides better outcomes. Grafting mild to moderate recession achieves more complete root coverage and more predictable results compared to treating severe recession. The tissue quality is better, the bone support is more intact, and the recovery is typically easier when recession is addressed at earlier stages.
Professional measurement with a periodontal probe provides objective data that self-assessment cannot deliver. What you estimate as two millimeters might measure as four millimeters. What looks severe might be stable, long-standing recession that needs monitoring but not grafting. Only clinical measurement determines actual severity.
Cost implications favor early treatment. Addressing recession at mild to moderate stages typically requires less complex grafting procedures, fewer appointments, and lower overall costs compared to treating severe recession with extensive bone loss. Some severe cases need multiple surgical procedures to achieve coverage that might have been accomplished with a single procedure if treated earlier.
Long-term tooth stability depends on maintaining adequate gum tissue and bone support. Allowing recession to progress compromises this support structure. Teeth with severe recession and bone loss have uncertain long-term prognosis even after successful grafting. Early intervention preserves the foundation your teeth need for decades of function.
Documenting Changes: Your Role in Early Detection

You see your teeth daily, which creates both advantage and disadvantage for detecting recession. The advantage is you have constant access for monitoring. The disadvantage is gradual changes become invisible when you see them every day. This daily exposure makes gradual gum recession difficult to recognize without structure.
Monthly self-examination creates structured monitoring. Set a recurring reminder for the same day each month. Check each tooth systematically, looking for visual signs and physical sensations.
Take photos every three to six months from consistent angles with consistent lighting. Date and save them in a dedicated folder. Comparing photos from six months apart reveals progression your daily checks miss.
Track sensitivity changes in a simple note. When cold drinks trigger stings in specific teeth, note the date and location. Increasing frequency or intensity indicates change requiring evaluation.
Self-monitoring has limitations. You cannot measure recession accurately at home. You cannot determine whether recession is stable or actively progressing without professional assessment over time. You cannot see recession on posterior teeth clearly. These limitations mean self-examination supplements but doesn’t replace professional evaluation.
When you notice changes – new sensitivity, visible progression in photos, increasing root exposure – schedule an appointment rather than waiting for your next routine cleaning. Early detection matters only if it leads to timely evaluation and intervention when needed.
At Optima Dental Surgery Center, we evaluate gum recession with clinical measurement, assess contributing factors, and discuss whether monitoring or grafting makes sense for your specific situation. If you’ve noticed signs of recession, sensitivity changes, or aesthetic concerns about your gum line, contact our office for evaluation. Understanding your current status and having a monitoring or treatment plan provides clarity and protects your long-term oral health. Establishing a baseline allows us to monitor gum recession accurately over time.
FAQ: Understanding Gum Recession
What is gum recession and why does it happen?
Gum recession occurs when gum tissue pulls away from the teeth, exposing root surfaces. It often results from brushing trauma, periodontal disease, genetics, or grinding.
Is gum recession reversible without surgery?
Gum recession cannot reverse on its own. Mild cases may be monitored, but advanced gum recession requires grafting to restore coverage.
Does gum recession always cause pain?
Not always. Some patients experience sensitivity early, while others notice visual changes before discomfort appears.
How is gum recession measured?
Dentists measure gum recession in millimeters using a periodontal probe during a clinical exam.
When should gum recession be treated?
Treatment is recommended when gum recession is progressing, causing sensitivity, affecting aesthetics, or compromising tooth stability.
Can gum recession lead to tooth loss?
Yes. Untreated gum recession can lead to bone loss, root decay, and long-term tooth instability.