The surgery is done. The crown is placed. You’ve made a significant investment in your oral health – and now the outcome depends almost entirely on what happens at home and at your follow-up appointments.
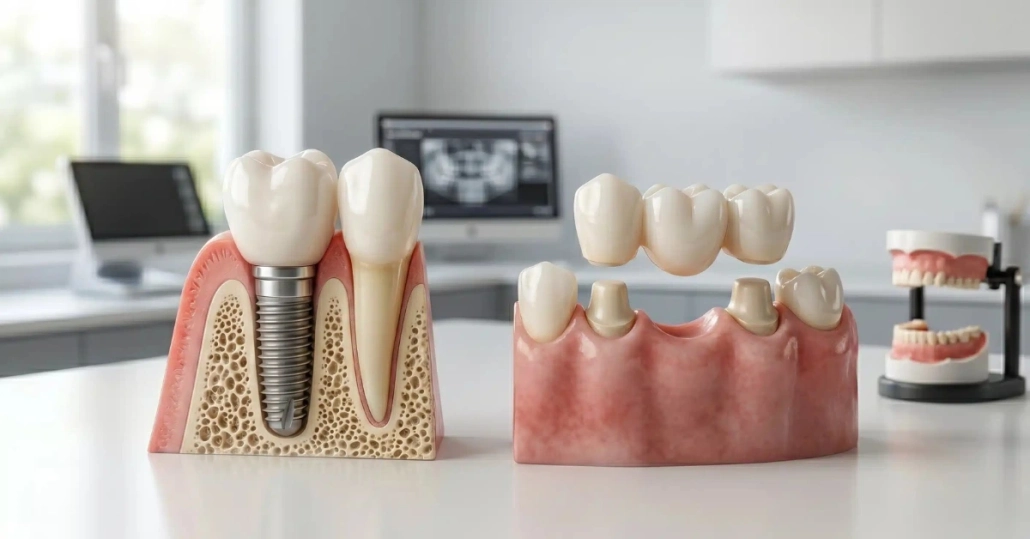
Dental implants don’t get cavities. But the tissue and bone surrounding them are fully susceptible to the same bacterial environment that damages natural teeth. Peri-implantitis – infection and inflammation around an implant – is the primary reason implants fail after successful placement. It’s also largely preventable when patients understand what daily care actually involves and why the monitoring appointments matter as much as they do.
This guide covers the full picture: daily habits, cleaning tools that make a difference, what your checkup schedule should look like, and the warning signs that warrant a call before your next scheduled visit.
Daily Dental Implant Care: The Non-Negotiables
Implant crowns and natural teeth share the same enemies – plaque, bacteria, and neglect. The cleaning routine that protects implants is similar to what you’d do for natural teeth, with a few specific considerations for the implant-gum junction.
Brush twice daily with a soft-bristle brush. Hard bristles can irritate gum tissue around the implant collar over time. A soft brush used with light pressure cleans effectively without trauma to the tissue. Electric toothbrushes are fine – many patients find them easier to use consistently at the gumline.
Pay attention to the gumline, not just the crown surface. Bacteria accumulate where the crown meets the gum. This junction is where peri-implantitis typically begins. Angling the brush toward the gumline and spending deliberate time there matters more than vigorous scrubbing of the crown itself.
Floss daily around every implant. Standard floss works well for single-implant crowns. Thread it under the contact point and move it in a C-shape around the base of the crown, just beneath the gumline on each side. For full-arch restorations like Stabili-teeth®, a water flosser or implant-specific floss threaders are typically more practical than standard floss alone.
Use a water flosser as a supplement, not a replacement. Water flossers are valuable for flushing debris from around implants and under bridge pontics, but they do not remove plaque the way physical flossing does. Use both for the most thorough result.
Choose non-abrasive toothpaste. Some whitening toothpastes contain abrasive particles that can scratch implant crown surfaces over time, making them more prone to staining and bacterial accumulation. A standard fluoride toothpaste is appropriate for most patients.
Cleaning Tools Worth Using
The right tools make consistent implant care easier. These are worth having in your routine:
- Soft-bristle or extra-soft toothbrush – manual or electric; replace every three months or when bristles splay
- Interdental brushes – small tapered brushes that fit between teeth and around implant crowns; particularly useful where standard floss is difficult to thread
- Water flosser – especially valuable for full-arch implant patients and anyone with limited dexterity that makes traditional flossing difficult
- Floss threaders or implant floss – designed to pass under bridge frameworks and around implant collars where standard floss cannot reach
- Antimicrobial mouth rinse – alcohol-free formulas can help reduce bacterial load around implants without drying out oral tissue; discuss with your provider before making it a daily habit, as some rinses are recommended for specific periods rather than indefinitely
What to Avoid to Protect Implant Longevity
Some habits place unnecessary stress on implant crowns and the surrounding tissue. None of these are absolute prohibitions for every patient, but they’re worth being deliberate about:
- Chewing ice – the hardness and unpredictability of ice can chip or crack crown material; it’s one of the more common causes of crown damage across both natural teeth and implants
- Using teeth as tools – opening packages, tearing tape, holding objects – all of these apply off-axis force to crowns that they aren’t designed to handle
- Grinding or clenching – bruxism places significant repetitive force on implant crowns and can affect the implant-bone interface over time; if you grind at night, a custom nightguard is worth discussing with your provider
- Smoking after implant placement – smoking is associated with impaired healing, reduced blood flow to gum tissue, and higher rates of peri-implantitis; patients who smoke after implant placement take on a meaningfully higher risk of long-term complications
- Skipping professional cleanings – home care maintains day-to-day cleanliness, but professional instruments reach areas your brush and floss cannot; and clinical monitoring catches what you cannot see
Your Dental Implant Checkup Schedule
Maintenance appointments are not optional extras – they’re a clinical requirement for protecting an implant over time. At each monitoring visit, we’re assessing things you cannot evaluate at home.
Here’s what a reasonable checkup schedule looks like for most implant patients:
- First few post-surgical visits – more frequent early appointments confirm that osseointegration is progressing, the surgical site is healing cleanly, and there are no early signs of infection or implant instability
- Every six months ongoing – once the implant is fully integrated and the restoration is complete, twice-yearly professional cleanings at a minimum and implant assessments are the standard recommendation for most patients
- Annual imaging – periodic X-rays or 3D imaging allows us to monitor bone levels around the implant over time; this is how early peri-implantitis is caught before it becomes significant bone loss
- More frequent monitoring for higher-risk patients – patients who smoke, have a history of periodontal disease, or show early signs of peri-implantitis may need appointments every three to four months rather than every six
If your general dentist is managing your cleanings, let them know you have implants so they can use instruments appropriate for implant surfaces. Certain metal scalers can scratch titanium; implant-compatible instruments are widely available and should be used instead.
Warning Signs That Warrant a Call Before Your Next Visit
Most implants, once fully integrated, are not something you notice day-to-day. That’s by design. When you do start noticing something around an implant, it’s worth paying attention to rather than waiting for the next scheduled appointment.
Contact your provider if you experience any of the following:
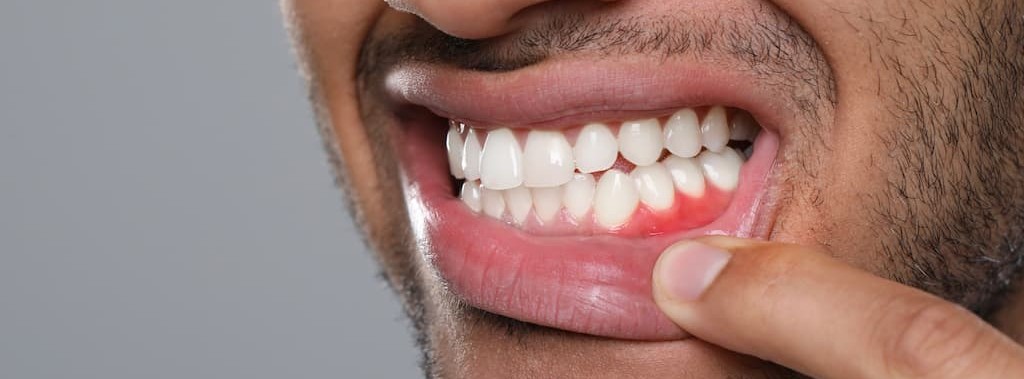
- Bleeding around an implant during brushing or flossing – occasional minor bleeding can occur from improper technique, but consistent bleeding at an implant site is a signal that tissue health needs to be assessed
- Swelling, redness, or tenderness at the implant site – these are the hallmarks of early peri-implantitis; caught early, the condition can often be managed without significant intervention
- The implant crown feels loose or different when you bite – a well-integrated implant should feel completely stable; any sensation of movement or shift in bite warrants timely evaluation
- Pain or pressure around an implant site – a fully healed implant should not be painful; localized discomfort that persists or develops after a period of no symptoms should be investigated
- Visible changes at the gumline – recession around an implant crown, exposure of the implant collar, or a change in how the crown sits relative to the tissue can indicate bone loss or tissue changes underneath
- A foul taste or odor localized to the implant area – this can indicate bacterial activity or infection at the implant site that isn’t visible from the outside
Peri-implantitis progresses. It does not resolve on its own. Early intervention is significantly less involved – and less costly – than treatment required after substantial bone loss has occurred.
Long-Term Outlook: What Good Care Produces
Patients who maintain consistent home care and keep their monitoring appointments tend to have implants that perform well for many years. The titanium post itself rarely fails once fully integrated – the variables that determine long-term success are almost entirely in the tissue and bone surrounding it, which is exactly what daily care and professional monitoring protect.
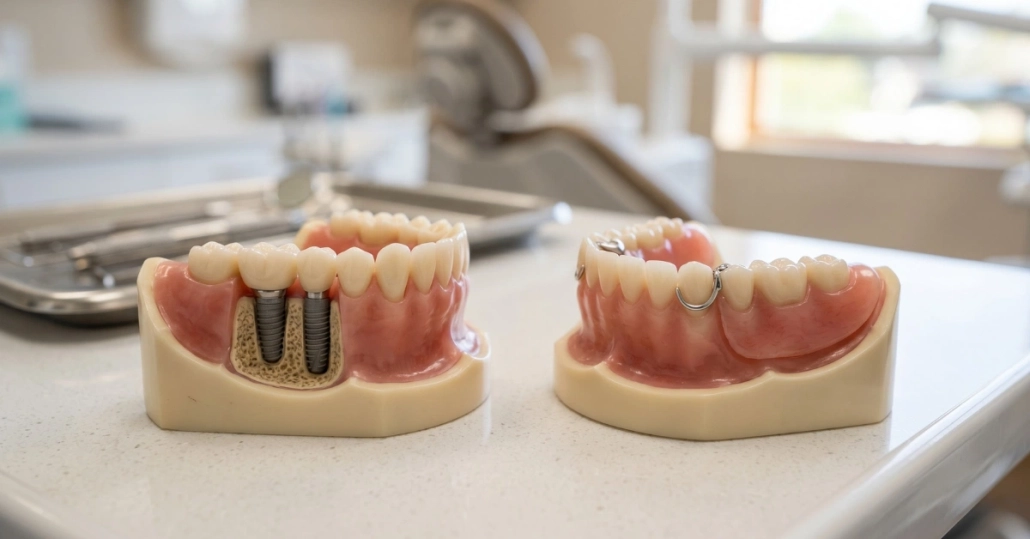
A full-arch restoration like Stabili-teeth® carries the same principles at a larger scale. More implants, more surface area to keep clean, and more reason to develop a consistent daily routine rather than treating it as an afterthought.
At Optima Dental Surgery Center, we don’t consider treatment finished at crown placement. Patients in Austin, Round Rock, and Temple who had their implants placed with us have access to ongoing monitoring designed to keep those implants performing the way they should. The investment you made deserves that follow-through.
Frequently Asked Questions About Dental Implant Care
How do you clean dental implants at home?
Brush twice daily with a soft-bristle brush, angling toward the gumline around each implant. Floss daily using standard floss for single crowns or implant floss threaders for bridge restorations. A water flosser adds value as a supplement. Non-abrasive toothpaste is recommended to avoid scratching crown surfaces.
Can dental implants get infected?
Yes. Peri-implantitis is a bacterial infection affecting the tissue and bone around an implant. It does not develop overnight – it progresses from early gum inflammation to deeper bone involvement over time if untreated. Consistent daily cleaning and regular professional monitoring are the primary tools for prevention.
How often should dental implants be checked by a dentist?
Most implant patients benefit from professional cleanings and implant assessments every six months, with periodic imaging to monitor bone levels around the implant post. Patients with a history of periodontal disease or other risk factors may need more frequent visits – typically every three to four months.
What are the signs of a failing dental implant?
Warning signs include bleeding or swelling around the implant, pain or pressure at the site, visible recession of gum tissue, a loose or shifting crown, and localized bad taste or odor. Any of these symptoms warrant a call to your provider rather than waiting for the next scheduled appointment.
This article is intended for educational purposes only and does not constitute medical advice. Individual treatment outcomes vary. Consult with a qualified dental professional regarding the care and monitoring schedule appropriate for your specific implant restoration.