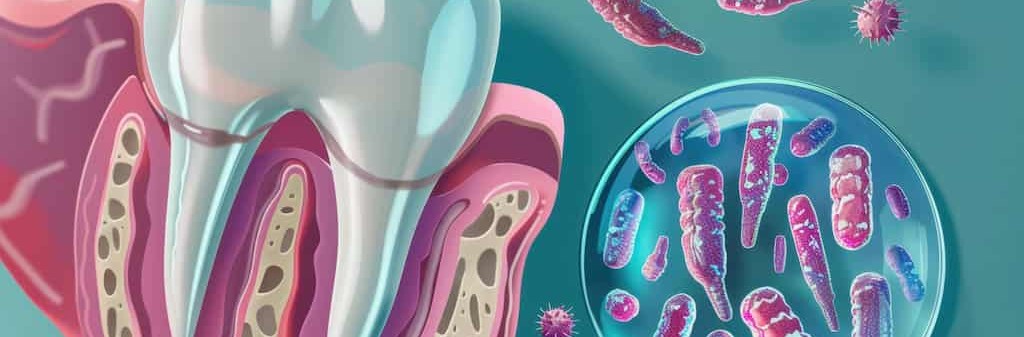
Your teeth get most of the attention. Brushing, whitening, straightening – the focus almost always lands on the teeth themselves. But the tissue holding those teeth in place is where gum disease quietly starts, and where it does its real damage before most people notice anything is wrong.
I’ve treated patients across Austin and Round Rock who had no idea their gums were in trouble until significant bone loss had already occurred. That’s not a failure of intelligence – it’s a failure of information. Gum disease prevention doesn’t require complicated routines or expensive products. It requires understanding what actually drives the problem, and then building a few consistent habits around that understanding.
That’s what this article is about. Not a lecture on what you’re doing wrong – a practical look at what works, why it works, and how to make it stick.
Why Gum Disease Starts Where It Does
Gum disease – clinically called periodontal disease – begins at the gumline. That’s where bacteria in plaque accumulate if they aren’t cleared away regularly. Left undisturbed, plaque hardens into tartar within 24 to 72 hours. Tartar can’t be removed by brushing at home. It requires professional cleaning.
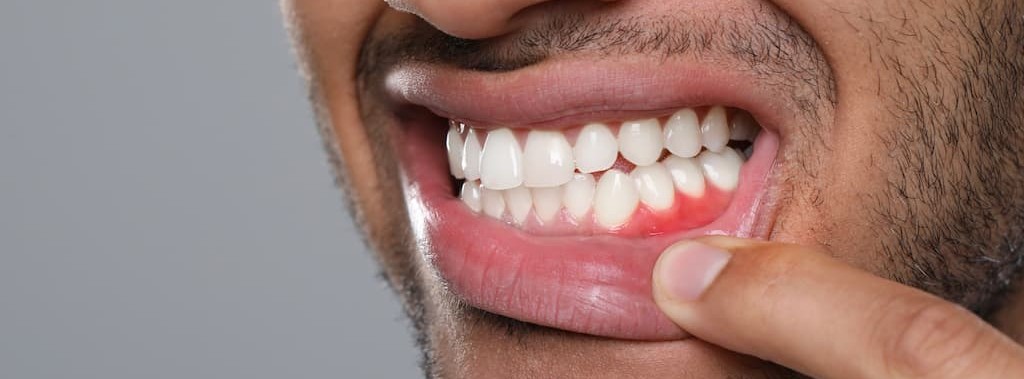
The earliest stage, gingivitis, shows up as red, swollen, or bleeding gums. At this stage the damage is reversible. Most people feel no pain, which is why it’s easy to dismiss the occasional bleed during brushing as normal. It isn’t.
When gingivitis goes unaddressed, it can progress to periodontitis – a deeper infection that affects the bone and connective tissue supporting the teeth. This stage is not reversible. It can be managed and slowed, but the bone loss that occurs doesn’t grow back on its own.
That progression – from preventable to manageable – is exactly the gap that daily habits are designed to close.
The Brushing Habits That Actually Matter
Most people brush. Fewer people brush in a way that actually clears bacteria from the gumline, which is the location that matters most for gum disease prevention.
Two changes make the biggest difference:
- Angle the bristles toward the gumline – Position your brush at roughly a 45-degree angle where the tooth meets the gum. This is where plaque accumulates and where most people’s brushing misses entirely
- Use gentle, circular motions – Scrubbing side to side with pressure doesn’t clean better – it irritates gum tissue and can wear down enamel over time. Small circular movements are more effective and less damaging
- Brush for two full minutes – Most people brush for 45 seconds. Use a timer once to see where you actually land. Two minutes, twice daily, is the standard that allows thorough coverage of all surfaces
- Don’t skip the last molars – The back teeth are consistently the most neglected and the most common site for early periodontal problems. Slow down and spend extra time there
- Replace your toothbrush every three months – Worn bristles don’t clean effectively. If the bristles are splayed, it’s already past time to replace it
Electric toothbrushes with oscillating heads can be helpful, particularly for patients who tend to apply too much pressure or rush through brushing. They’re not required for good gum health – technique matters more than the tool.
Why Flossing Matters More Than Brushing for Gum Health
If you have to choose between brushing and flossing for gum disease prevention specifically, floss. Brushing cleans the surfaces you can see. Flossing cleans the spaces between teeth and just below the gumline where a toothbrush cannot reach – and where periodontal disease most commonly begins.
The two most common reasons people skip flossing are that it takes time and that it causes bleeding. Both are worth addressing directly.
On time: flossing an entire mouth takes about 90 seconds when it becomes a habit. The barrier is almost never time – it’s the friction of remembering and starting. Keeping floss on the bathroom counter rather than in a drawer removes that friction considerably.
On bleeding: bleeding gums during flossing are a sign of inflammation, which is typically a sign of gum disease in early stages – not a sign that flossing is causing damage. For most patients, consistent flossing reduces bleeding within one to two weeks as the inflammation resolves. If bleeding persists beyond that window, it warrants a professional evaluation.
Floss picks and water flossers are useful alternatives for patients with dexterity challenges or dental work that makes traditional floss difficult. Water flossers in particular have solid evidence for reducing gingival inflammation and are worth considering if you’ve never been able to maintain a traditional flossing routine.
The Diet Connection Most Patients Don’t Think About
What you eat doesn’t just affect your teeth – it directly affects your gum tissue and your body’s ability to control oral bacteria.
Sugar is the most obvious factor. Oral bacteria feed on simple sugars and produce acids as a byproduct. Those acids irritate gum tissue and fuel the inflammatory response that drives periodontal disease. Reducing added sugar – particularly in forms that linger in the mouth, like sticky snacks and sweetened drinks sipped throughout the day – reduces the bacterial fuel source.
Less discussed but equally important:
- Vitamin C – Deficiency in vitamin C is directly linked to gum tissue breakdown. The connection was documented centuries ago in sailors who developed scurvy – a condition characterized by bleeding gums and tooth loss. Modern deficiency is less severe but still measurable. Citrus, bell peppers, strawberries, and broccoli are reliable sources
- Vitamin D – Plays a role in immune regulation and may help the body control the bacterial infection component of periodontal disease. Many adults are deficient, particularly those with limited sun exposure
- Omega-3 fatty acids – Found in fatty fish, flaxseed, and walnuts, omega-3s have anti-inflammatory properties that some research suggests may support periodontal health alongside standard care
- Water – Saliva is your mouth’s natural defense system. It neutralizes acids, remineralizes enamel, and clears food debris. Staying well-hydrated supports saliva production. Dry mouth – whether from dehydration, medications, or other causes – creates conditions where bacteria multiply more readily
None of this requires a complete diet overhaul. Small, consistent shifts – less sugar in beverages, more vegetables, adequate water – move the needle meaningfully over time.
Lifestyle Factors That Affect Your Gum Health
Daily habits extend beyond the bathroom. Several lifestyle factors have well-documented effects on periodontal health, and understanding them helps patients see gum disease prevention as part of broader health maintenance rather than a separate dental concern.
Smoking and tobacco use are the single most significant modifiable risk factors for periodontal disease. Tobacco reduces blood flow to gum tissue, impairs the immune response, and masks the early warning signs – particularly bleeding – that would otherwise signal inflammation. Smokers develop more severe periodontal disease faster and respond less well to treatment than non-smokers. If there is one lifestyle change that moves the needle most on gum health, this is it.
Stress affects gum health through two pathways. First, elevated cortisol suppresses immune function, making it harder for the body to control oral bacteria. Second, stress-related behaviors – skipping dental visits, poor sleep, teeth grinding – all create conditions where periodontal disease can progress. Chronic stress isn’t always within easy control, but awareness of its oral health effects can motivate patients to be more consistent with the habits that compensate for it.
Certain medications cause dry mouth as a side effect, and a dry oral environment significantly accelerates bacterial growth. Common culprits include antihistamines, antidepressants, blood pressure medications, and diuretics. If you take medications regularly and notice persistent dry mouth, mentioning it at your dental visit allows your care team to adjust recommendations accordingly.
Diabetes has a well-established bidirectional relationship with periodontal disease – uncontrolled blood sugar increases susceptibility to gum infection, and active gum disease can make blood sugar harder to control. Patients managing diabetes should be particularly consistent with both their periodontal care and their dental visit schedule.
How Often You Actually Need Professional Cleanings
Home care handles what happens between appointments. Professional cleanings handle what home care cannot.
Tartar accumulation – hardened plaque that can only be removed with professional instruments – is inevitable for most patients regardless of how well they brush and floss. The standard recommendation of two cleanings per year is appropriate for patients with healthy gums and low risk factors. For patients with a history of periodontal disease, smokers, or those with conditions like diabetes, more frequent visits – typically every three to four months – are often recommended to stay ahead of progression.
The professional cleaning appointment does more than remove tartar. It includes a periodontal evaluation – measuring pocket depths around each tooth – that detects early changes before they become visible symptoms. That monitoring is how gum disease is caught at the reversible gingivitis stage rather than after bone loss has begun.
Skipping cleanings to save money is one of the more expensive decisions patients make in the long run. The cost of a cleaning is significantly lower than the cost of treating periodontitis, performing bone grafting, or replacing teeth that were lost to disease that could have been caught earlier.
| Factor | Gingivitis | Periodontitis |
|---|---|---|
| Stage | Early gum disease | Advanced gum disease |
| Reversible? | Yes – with proper care | No – manageable but not reversible |
| Bone loss? | No | Yes – progressive without treatment |
| Common symptoms | Red, swollen, or bleeding gums | Receding gums, loose teeth, bad breath |
| Treatment | Improved home care + professional cleaning | Scaling, root planing, possible surgery |
| Key action | Act now – it’s still reversible | Don’t delay – progression can be slowed |
Warning Signs You Should Not Wait Out
Gum disease prevention is the goal. But knowing when prevention has already been outpaced matters just as much.
Contact a periodontist or dental professional if you notice any of the following:
- Gums that bleed consistently during brushing or flossing, particularly if it continues past two weeks of improved home care
- Persistent bad breath that doesn’t resolve with brushing – this is often a sign of bacterial activity below the gumline
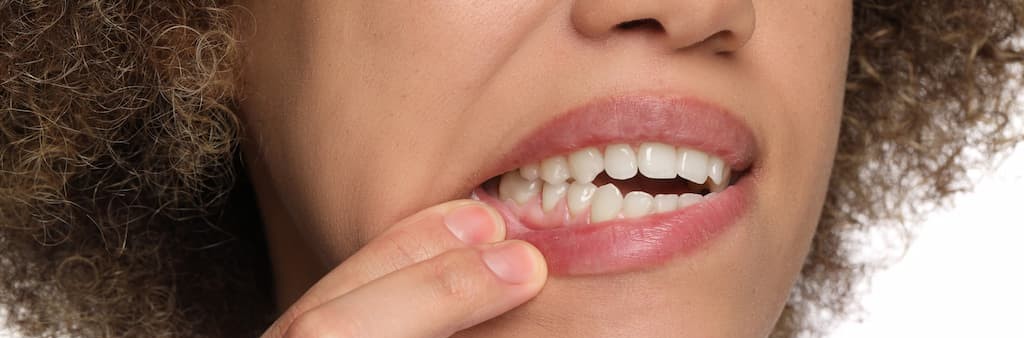
- Gums that appear to be pulling away from teeth – receding gum tissue exposes the root surface and indicates progressing disease
- Teeth that feel loose or have shifted position – this signals bone loss that requires professional evaluation
- Pain when chewing that wasn’t present before
- Sensitivity along the gumline rather than in the tooth itself
None of these symptoms resolve on their own. Early evaluation keeps options open. Delayed evaluation narrows them.
If you’re in Austin or Round Rock and haven’t had a periodontal evaluation recently, our periodontal disease treatment page covers what that assessment involves and what treatment may look like if disease is found. For patients already managing gum disease, our scaling and root planing page explains the most common non-surgical treatment in detail.
Building a Routine That Sticks
The habits that prevent gum disease aren’t complicated. The challenge is consistency, and consistency comes from making habits automatic rather than intentional.
A few approaches that work:
- Attach new habits to existing ones – Flossing immediately after brushing rather than as a separate step removes the decision of when to do it
- Keep supplies visible – Floss left on the counter is used far more reliably than floss stored under the cabinet
- Set a two-minute timer once – Most patients are surprised how long two minutes actually feels. Experiencing it calibrates your sense of whether you’re brushing long enough
- Schedule your cleaning before you leave the last one – Future-you will not feel more motivated to call. Booking the next appointment on the way out removes the friction entirely
Small, repeatable actions compounded over months are what separate patients who maintain healthy gums from those who cycle in and out of active treatment. The daily investment is modest. The long-term payoff – keeping your teeth and avoiding the cost and complexity of treating advanced disease – is not.
Frequently Asked Questions About Gum Disease Prevention
Can gum disease be reversed with better brushing and flossing?
At the gingivitis stage – the earliest form of gum disease – yes. Consistent brushing at the gumline, daily flossing, and a professional cleaning can resolve gingivitis completely because no permanent bone loss has occurred yet. Once disease progresses to periodontitis and bone loss begins, it cannot be reversed, only managed. This is why catching it early matters.
How do I know if I already have gum disease?
Common early signs include gums that bleed when you brush or floss, persistent bad breath, or gums that look red or swollen rather than pink and firm. Many patients have no noticeable symptoms in early stages, which is why professional periodontal evaluations – where pocket depths are measured around each tooth – are the most reliable detection method.
Is gum disease genetic?
Genetic factors do play a role in susceptibility. Some patients develop periodontal disease more readily than others even with good home care, due to how their immune system responds to oral bacteria. If gum disease runs in your family, more frequent professional monitoring and particularly consistent home care are worth prioritizing. Genetics influence risk but don’t determine outcome.
What is the connection between gum disease and heart health?
Research has identified associations between periodontal disease and cardiovascular conditions, though the precise nature of that relationship continues to be studied. The leading explanation involves oral bacteria entering the bloodstream through inflamed gum tissue and contributing to systemic inflammation. While this doesn’t mean gum disease causes heart disease, it does reinforce that periodontal health is part of whole-body health – not a separate concern.
How often should I see a periodontist versus a general dentist for gum care?
For patients with healthy gums and no history of periodontal disease, a general dentist typically handles routine monitoring and cleaning. Patients with active or past gum disease, those with significant risk factors like smoking or diabetes, or those showing signs of progression benefit from evaluation by a periodontist – a specialist with additional training in diagnosing and treating the full spectrum of periodontal conditions.
Can children get gum disease?
Gingivitis is common in children and adolescents, particularly during puberty when hormonal changes can increase gum tissue sensitivity to plaque. More severe forms of periodontal disease are less common in younger patients but do occur, particularly in the presence of certain systemic conditions. Establishing good brushing and flossing habits early is both protective and practical.
The Simplest Investment in Your Long-Term Oral Health
Gum disease prevention doesn’t ask much. A few minutes a day, attention to what you eat and drink, awareness of the risk factors that apply to your situation, and regular professional care to catch what home routines can’t.
What it offers in return is significant – teeth that stay in place, gum tissue that stays healthy, and the avoidance of treatments that become necessary when disease is caught late. I’ve seen patients work their way back from advanced periodontitis, and while that path is manageable, it is far harder than the path that prevents it.
If you’re due for a periodontal evaluation or have noticed any of the warning signs covered here, Optima Dental Surgery Center serves patients across Austin, Round Rock, and Temple. Our team includes periodontists who specialize in the full range of gum disease prevention, evaluation, and treatment. You can learn more about our approach to laser periodontal therapy as an alternative to traditional gum surgery, or contact us to schedule a consultation.
Due for a Periodontal Evaluation?
Early detection is what keeps gum disease reversible. Schedule a consultation at Optima Dental Surgery Center in Round Rock – no referral needed.
Call (512) 341-2321 or visit optimaimplants.com/contact-us/