You’ve lost a tooth – or you’re about to – and now you’re sorting through options that all sound similar until you start reading the fine print. A single-tooth denture, a flipper, an implant, a bridge. Each one gets described as a “solution,” but they work very differently, cost very differently, and hold up very differently over time.
Most patients I see at this stage are mid-decision. They’ve done some research, they have a ballpark sense of what implants cost, and they’re wondering whether a less expensive option is worth the tradeoff. That’s a reasonable place to be, and it deserves a straightforward comparison rather than a sales pitch.
Here’s what I can tell you as a dental specialist: the right answer depends on your specific tooth, your bone health, your timeline, and your long-term goals. This article gives you the clinical framework to have that conversation with confidence.
What Is a Single-Tooth Denture?
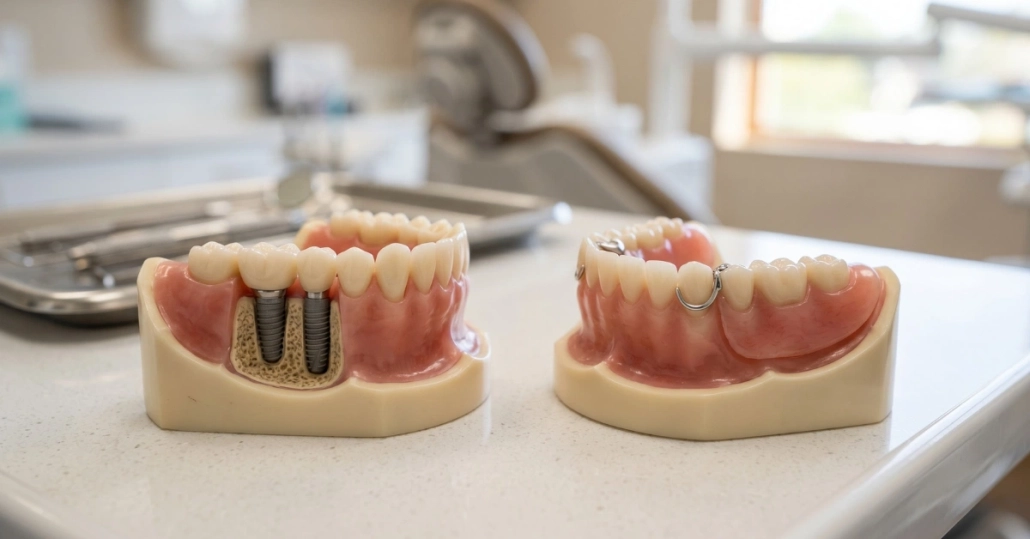
A single-tooth denture, often called a flipper or a partial denture, is a removable appliance that fills the gap left by a missing tooth. It typically consists of an acrylic base with a prosthetic tooth that clips or rests against surrounding teeth and gum tissue. The tooth is visible and functional to a degree, but the appliance comes in and out of your mouth.
Flippers are frequently used as temporary restorations while patients heal from extractions or wait for implant osseointegration. They are not designed as permanent solutions, though some patients use them long-term due to cost or health factors that prevent implant surgery.
A removable partial denture is a more durable version of the same concept – constructed with a metal framework rather than acrylic alone, and designed for longer-term wear. It still comes out for cleaning and at night, but it holds up better than a flipper under daily use.
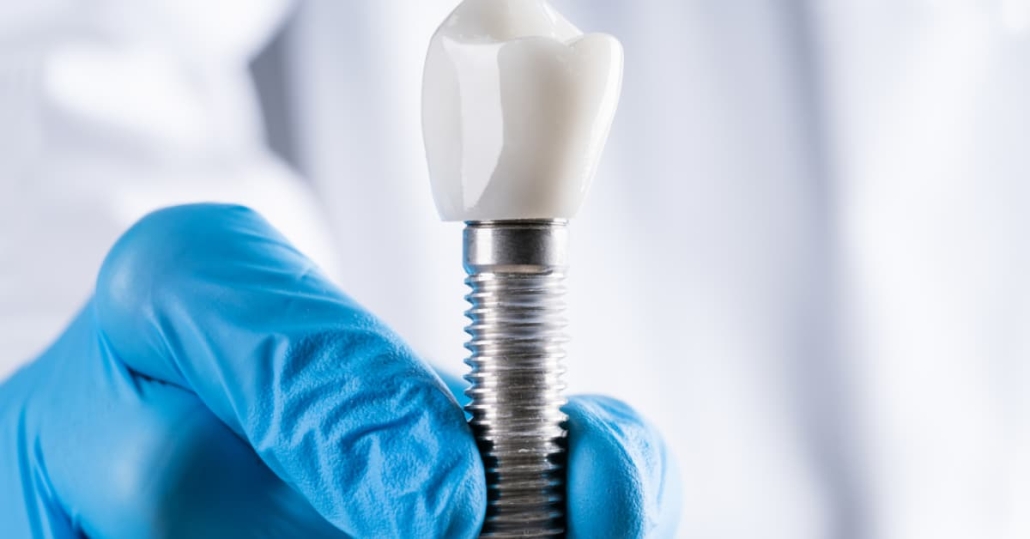
What Is a Single-Tooth Implant?
A single-tooth implant replaces the entire tooth structure – root and crown. A titanium post is placed surgically into the jawbone, allowed to integrate over several months, and then topped with a custom-made crown that matches the surrounding teeth. The result is a fixed restoration that does not come out and functions like a natural tooth.
The implant post serves as an artificial root. This is clinically significant because it stimulates the jawbone the way a natural root does, helping to preserve bone volume in the area. No other single-tooth replacement option provides this effect.
For a detailed walkthrough of the implant process from consultation through recovery, our dental implants guide covers the full timeline and candidacy factors.
Side-by-Side Comparison
The table below compares the most clinically relevant factors for patients choosing between a single-tooth denture and a single-tooth implant.
| Factor | Single-Tooth Denture / Flipper | Single-Tooth Implant |
|---|---|---|
| Fixed or removable | Removable | Fixed (permanent) |
| Bone preservation | None – bone resorption continues | Yes – implant stimulates jawbone |
| Impact on adjacent teeth | Clips onto neighboring teeth; may cause wear | None – stands independently |
| Typical lifespan | 6 months-5 years for flippers; longer for partials | Implant post: decades with proper care |
| Approximate cost range | $450 – $1,500 | $3,000 – $5,500+ |
| Surgery required | No | Yes |
| Healing timeline | Days to weeks | 3-6+ months for full osseointegration |
| Eating restrictions | Significant – hard and sticky foods avoided | Minimal after full healing |
| Maintenance | Remove nightly, soak, clean separately | Brush and floss like a natural tooth |
Cost ranges above are general estimates. Actual costs vary based on location, the specific tooth being replaced, whether preparatory procedures are needed, and the materials used. Always get a detailed breakdown after a clinical evaluation – not a phone quote.
The Cost Conversation: Upfront vs. Long-Term
The price gap between a flipper and an implant is real, and I won’t minimize it. For patients managing a tight budget, a removable option has a clear short-term advantage.
Where the math shifts is over time. A flipper typically lasts six months to five years before it needs replacement or repair. A removable partial denture holds up longer but still requires adjustments as the jawbone changes shape – and without a root stimulating the bone, that change is ongoing. You may find yourself paying for refitting and replacement across a decade that adds up closer to implant costs without the functional benefits.
The jawbone resorption factor compounds this. Once bone volume is lost, restoring it for a future implant requires grafting – a procedure that adds cost and time to a treatment plan that could have been simpler earlier. Patients who initially defer implants sometimes find that the longer they wait, the more preparatory work is needed.
This is not an argument that everyone should get an implant regardless of circumstance. It’s context for evaluating the real cost comparison across a realistic timeframe rather than at a single point in time.
When a Removable Option Actually Makes Sense
There are genuine clinical and personal situations where a single-tooth denture or partial is the appropriate choice – not a compromise, but a considered decision.
- As a temporary restoration – a flipper is commonly used during the months between extraction and final implant crown placement, keeping the space occupied and aesthetically acceptable while osseointegration occurs
- When surgery is medically contraindicated – certain health conditions, medications, or uncontrolled systemic disease may make implant surgery inadvisable; in these cases, a well-fitted removable partial is a reasonable long-term path
- When bone loss is too significant for implant placement – if inadequate bone is present and the patient is not a candidate for grafting, removable options may be the viable solution
- Budget constraints with plans to upgrade – for patients who need the gap addressed now but intend to pursue an implant when finances allow, a temporary flipper buys time without foreclosing future options
- The tooth being replaced is not a high-function area – a back molar that took heavy chewing load has different replacement priorities than a front tooth primarily affecting appearance
When an Implant Is the Stronger Clinical Choice
For most healthy adults without significant bone loss, a single-tooth implant yields outcomes that removable options cannot replicate over time. The situations where an implant is particularly worth prioritizing:
- Front teeth – aesthetics, speech, and the visibility of a fixed result versus a removable appliance are most pronounced for anterior teeth
- Younger patients – someone replacing a tooth in their 40s or 50s is looking at decades of use; an implant that lasts that timeframe is a different value proposition than for someone in their 80s
- Patients who already have adjacent tooth concerns – a partial denture that clips onto neighboring teeth can accelerate wear on those teeth and increase bone loss; an implant does not touch them
- Patients with active bone loss concerns – if the jaw has already experienced some resorption from a previous missing tooth, placing an implant while adequate bone remains is more straightforward than waiting
- Patients who want predictability – an implant integrated into bone is not going to shift, slip, or need adhesive; for patients where that stability matters day-to-day, the tradeoffs of a removable option are often not acceptable
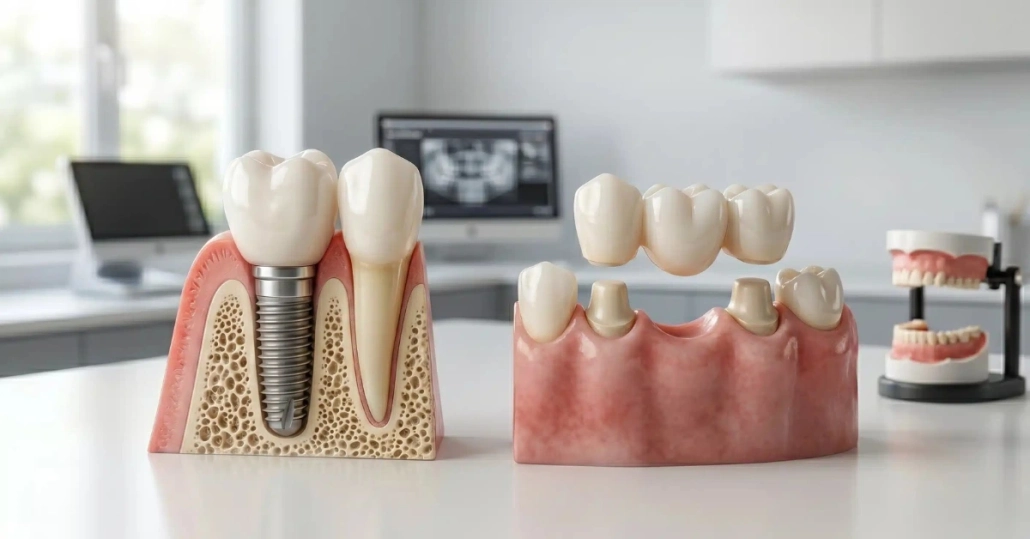
What About a Dental Bridge?
Patients comparing single-tooth options often encounter bridges in their research. A bridge fills a gap by anchoring to the teeth on either side, which are permanently shaped down to support crowns. The middle tooth – the “pontic” – hangs between them.
A bridge is fixed, which patients appreciate compared to a removable partial. But the permanent alteration of healthy adjacent teeth is a meaningful clinical trade-off. It also does not address bone resorption under the gap, since there is no root structure present.
For many patients, a bridge represents a middle ground on cost – less than a single implant in many cases, more than a flipper. Whether that middle ground is worth the trade-offs is a case-by-case conversation, but the modification of otherwise healthy teeth is a factor worth weighing carefully.
How We Approach This Decision at Optima
Patients in Austin, Round Rock, and Temple who come to Optima for a missing tooth evaluation get 3D cone beam imaging at their consultation. That imaging tells us the bone volume available, the position of nerves and sinus structures, and whether any preparatory work would be needed before implant placement.
With that information in hand, we can give you a realistic treatment plan – including cost, timeline, and what each option actually involves for your specific anatomy. Not a general range pulled from a website. A number is attached to your situation.
We also work with multiple financing partners, because the upfront cost of an implant is often what gives patients pause when the long-term math would favor it. Knowing your options on both sides of that conversation – clinical and financial – is what allows you to make a decision you’re confident in.
Frequently Asked Questions
Is a flipper the same as a single-tooth denture?
Yes. A flipper is a type of single-tooth partial denture – a removable acrylic appliance used to fill a gap. The term “flipper” comes from how the appliance can be removed by flipping it out with the tongue. It is typically considered a temporary solution.
Can a single-tooth denture look natural?
A well-made partial denture can approximate the appearance of a natural tooth, particularly for back teeth. For front teeth, fixed options like implants typically produce more natural-looking results since they emerge from the gumline the way a natural tooth does, rather than resting on top of the tissue.
Will I need bone grafting before a single-tooth implant?
Not always. Whether grafting is needed depends on how much bone remains at the site. Patients who have had a tooth missing for a long period are more likely to have experienced bone resorption and may require grafting. A 3D scan at consultation determines this with accuracy.
How soon after extraction can an implant be placed?
In some cases, an implant can be placed the same day as extraction – called immediate implant placement. In others, the site requires healing time first. This depends on the condition of the bone and surrounding tissue at the time of extraction, which is assessed clinically.
This article is intended for educational purposes only and does not constitute medical advice. Individual treatment outcomes vary. Consult with a qualified dental professional to determine which tooth replacement option is appropriate for your specific situation.