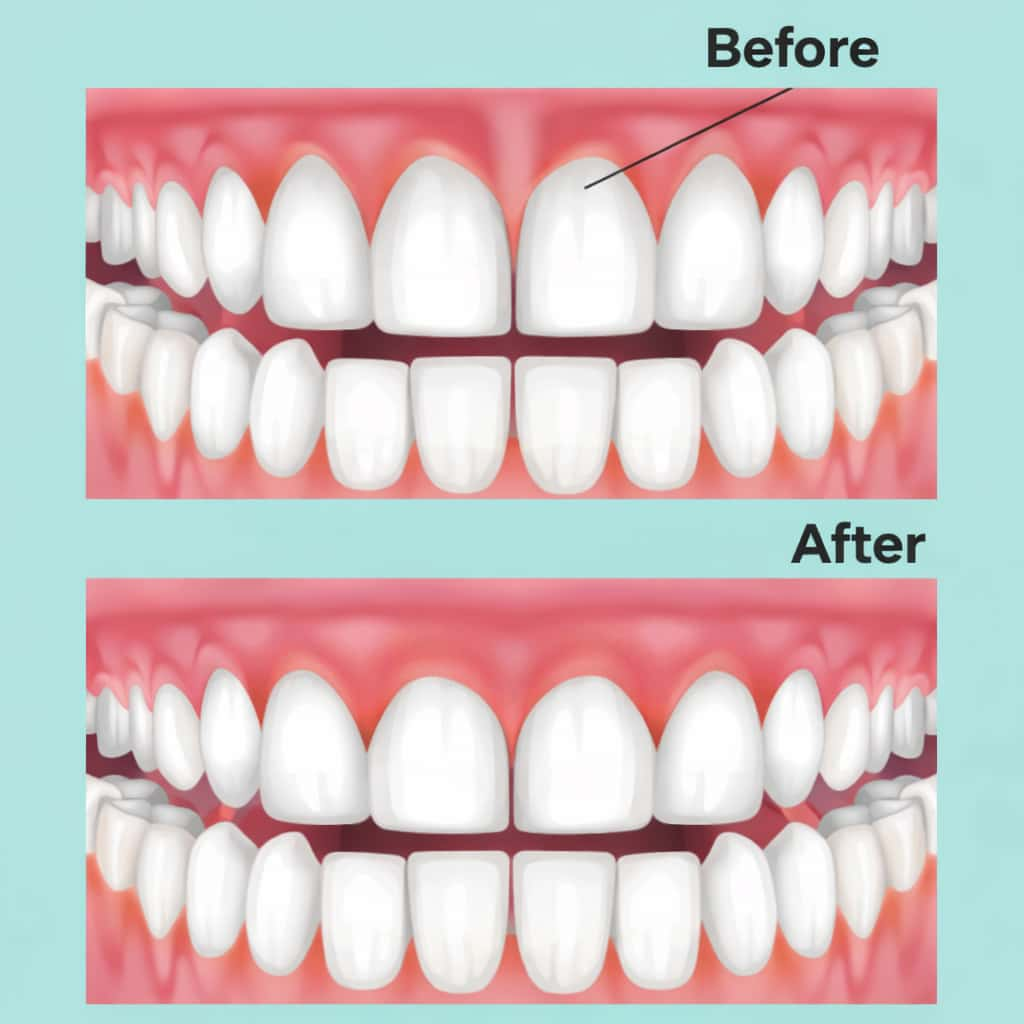
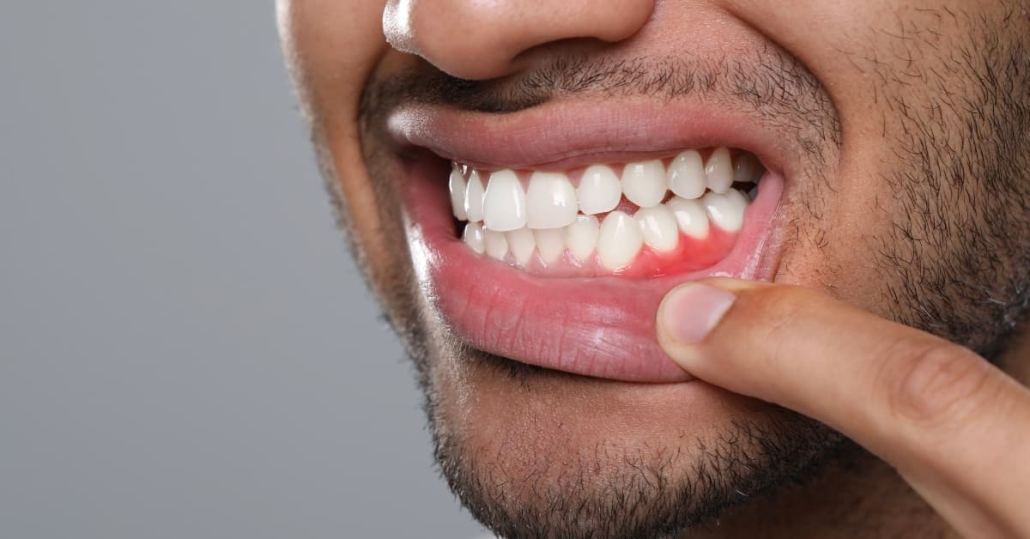
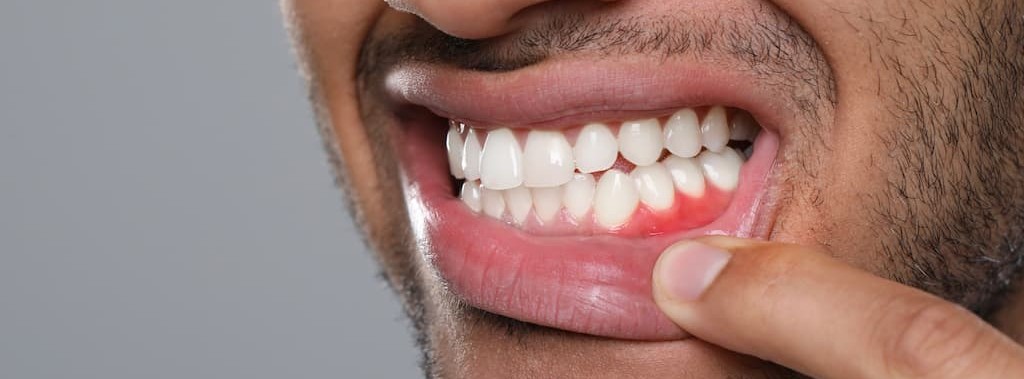
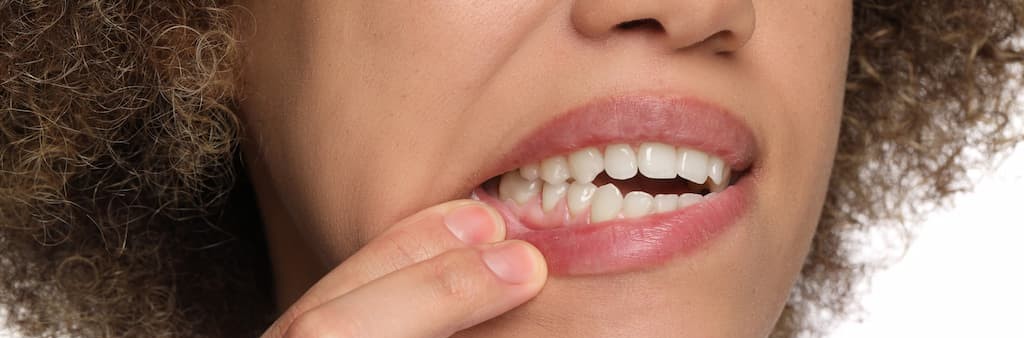
Your gums have been receding for years. You notice it every time you brush – longer teeth, exposed roots, sharp sensitivity when you drink something cold. You’ve convinced yourself it’s just aging, that maybe it’ll stabilize on its own. Meanwhile, your smile looks different in photos, and you’re avoiding certain foods because the sensitivity stops you cold.
I know this because gum recession rarely announces itself with drama. It creeps in gradually, tooth by tooth, until you realize the damage has already progressed. I’ve guided hundreds of patients through gum grafting procedures, and most wish they’d addressed the problem sooner – before the recession compromised more tissue, before the sensitivity became daily interference, before the aesthetic impact affected their confidence. Understanding when gum grafting is necessary and how it works is the first step in stopping recession before it causes permanent damage.
Here’s what you need to understand about gum grafting – the procedure types that restore coverage, the recovery process that’s more manageable than you think, and the results that protect both your health and your smile. This isn’t about cosmetic perfection. This is about stopping progression, reducing sensitivity, and giving your teeth the support they need for long-term stability.
Why Gum Recession Demands More Than Watching and Waiting
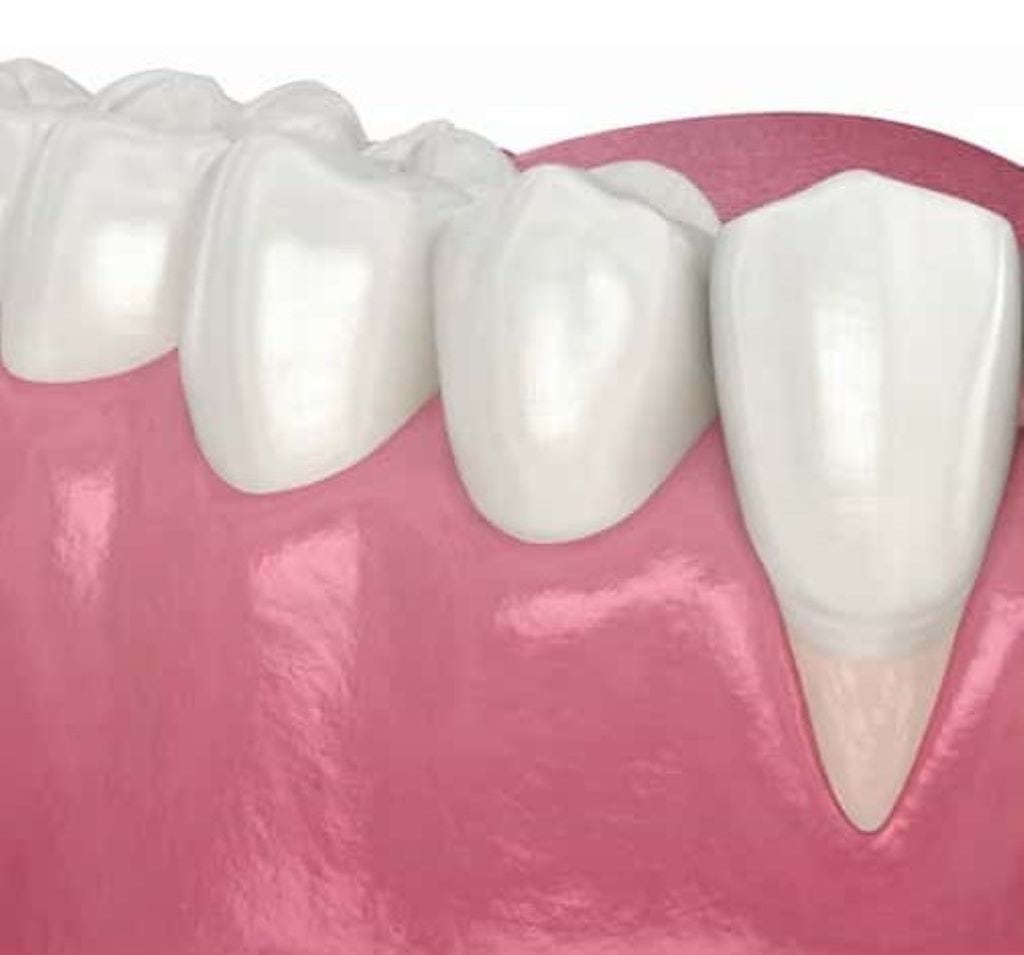
Gum grafting is often the only predictable way to stop progressive gum recession once tissue and bone loss begin. You might be thinking the recession will stop on its own, that it’s just a minor cosmetic issue you can live with. That thinking costs people teeth.
Gum recession is progressive. Without gum grafting, lost tissue does not grow back, and exposed roots remain vulnerable to decay and sensitivity. When gums recede, they take the underlying bone with them. That bone supports your teeth. Less bone means less stability, which eventually leads to tooth mobility and potential tooth loss.
The exposed root surface creates another problem – it’s softer than enamel and more susceptible to decay. Root cavities develop faster than crown cavities, and they’re harder to treat because they’re below the gum line. You’re fighting a battle on two fronts – structural compromise from bone loss and increased decay risk from exposed roots.
What causes this recession in the first place? Several factors work alone or in combination:
- Aggressive brushing habits – Scrubbing with hard bristles wears away gum tissue over time, creating V-shaped notches at the gum line that expose roots and weaken tooth structure
- Periodontal disease progression – Bacterial infection destroys the connective tissue and bone that hold gums in place, causing tissue to pull away from teeth and creating pockets that deepen over time
- Genetic predisposition to thin tissue – Some people are born with naturally thin, delicate gum tissue that’s more prone to recession regardless of oral hygiene quality
- Teeth positioned outside the bone – When teeth sit too far forward or outside the natural bone envelope, there’s insufficient tissue to cover them properly, making recession inevitable
- Grinding and clenching patterns – Excessive force from grinding damages the thin tissue at the gum line, causing it to recede and creating wear patterns that compound the problem
The severity determines urgency. Mild recession – one or two millimeters – might be monitored if it’s stable and causing no symptoms. Moderate to severe recession – three millimeters or more, especially with root sensitivity or aesthetic concerns – requires intervention. Waiting doesn’t improve outcomes. It just gives the recession more time to progress.
The Three Main Types of Gum Grafting: Which One Fits Your Situation
Each gum grafting technique addresses different patterns of recession, tissue thickness, and aesthetic concerns.
Gum grafting is not a single procedure but a category of surgical techniques designed to restore lost gum tissue and protect exposed roots. The type you need depends on the location and severity of recession, the amount of existing tissue, and your specific goals for function and aesthetics.
Connective Tissue Graft – The Most Common Approach
This technique addresses recession while maintaining natural appearance. I take a small piece of tissue from the roof of your mouth – specifically from under the surface layer – and position it over the exposed root. The donor site heals quickly because I’m only removing the connective tissue layer, leaving the surface tissue intact. This form of gum grafting is the most common option for patients concerned about both appearance and sensitivity.
This graft type works exceptionally well for covering exposed roots on front teeth where aesthetics matter most. The transplanted tissue integrates with your existing gums, creating coverage that looks natural and feels normal. Most patients need connective tissue grafts when they’re concerned about both the appearance of recession and the sensitivity it causes.
Free Gingival Graft – Building Attached Tissue
In some cases, gum grafting focuses less on root coverage and more on rebuilding protective tissue. Sometimes the problem isn’t just recession – it’s insufficient attached gum tissue. Attached gums are the thick, coral-pink tissue that surrounds your teeth and protects the underlying structures. When you don’t have enough attached tissue, recession accelerates and treatment options become limited.
Free gingival grafts take tissue directly from the roof of your mouth and transplant it to areas that need more attached gum. The grafted tissue is thicker and creates a band of protective tissue around teeth. This approach is less about aesthetics and more about creating stable, healthy tissue that resists future recession.
I use free gingival grafts when patients have minimal existing tissue, when orthodontic treatment is planned and additional tissue is needed for stability, or when previous grafts have failed due to insufficient tissue quality. This type of gum grafting is especially valuable when future orthodontic movement or ongoing recession risk is present.
Pedicle Graft – Using Nearby Tissue
When you have adequate gum tissue next to the recession area, a pedicle graft moves that tissue laterally to cover the exposed root. The tissue stays partially attached to its original location, maintaining its blood supply throughout the procedure. This approach works only when there’s sufficient donor tissue adjacent to the recession site.
Pedicle grafts heal faster than other graft types because the tissue never loses its blood supply. The downside is limited applicability – most patients with recession don’t have excess tissue in the right location to make this technique viable. While effective in select cases, this gum grafting technique is only appropriate when nearby tissue quality allows predictable coverage.
Which type makes sense for your situation?
That determination happens during examination, when I assess recession severity, tissue quality, root anatomy, and your priorities for treatment. Single-tooth recession with good adjacent tissue might need one approach, while multiple areas of recession require a different strategy. The goal stays consistent regardless of technique – restore coverage, reduce sensitivity, create stable tissue that resists future recession.
What Actually Happens During Gum Graft Surgery
A gum grafting procedure is carefully planned to maximize tissue survival and long-term stability. Every gum grafting procedure is methodical and precise, with careful attention to tissue handling and blood supply.
I start with local anesthesia to completely numb both the recipient site – where the graft goes – and the donor site on the roof of your mouth. You’ll feel pressure during the procedure, but no sharp discomfort. Most patients are surprised by how manageable the experience is compared to their anxiety beforehand.
For connective tissue grafts, I make a small incision in the roof of your mouth and remove a thin layer of tissue from beneath the surface. The incision is typically one to two centimeters, just large enough to harvest the tissue needed. I close the donor site with sutures, and it heals within two weeks with minimal discomfort.
At the recipient site, I prepare the area by gently lifting the existing gum tissue to create a pocket. The harvested connective tissue slides into this pocket and gets positioned over the exposed root. Sutures hold everything in place while healing occurs. The technique requires precision – the graft must contact the root surface directly and integrate with the surrounding tissue for optimal results.
Free gingival grafts work differently. I take tissue from the palate surface rather than from underneath, which means the donor site takes slightly longer to heal. The harvested tissue gets trimmed to size and sutured directly onto the prepared recipient site. This creates a thicker band of tissue, though the color match isn’t quite as seamless as connective tissue grafts.
The entire procedure takes 30 to 60 minutes for a single site, longer if we’re addressing multiple areas. I work deliberately, checking tissue positioning and blood flow throughout the process. Rushed grafts fail more often – proper technique takes time.
Pain management extends beyond the surgery itself. I prescribe medication for the first few days when discomfort peaks, along with specific instructions for managing both the graft site and the donor site. Most patients report the palate donor site causes more discomfort than the graft itself, particularly during the first 48 hours. That discomfort is temporary and manageable with proper medication and care protocol.
Recovery Timeline: The First Two Weeks and Beyond
Recovery after gum grafting follows a predictable and manageable timeline. Understanding what to expect during each phase helps you manage the process without unnecessary worry.
The First 24 to 48 Hours – Critical Protection Phase
This period demands the most attention. The graft is vulnerable and needs protection from any disruption. You’ll experience swelling and discomfort, particularly at the donor site. Ice packs applied externally help control swelling during the first day. Pain medication keeps discomfort manageable – most patients need prescription medication for two to three days, then transition to over-the-counter options.
Eating requires modification. Soft foods that require minimal chewing become your diet – yogurt, smoothies, mashed potatoes, protein shakes. Nothing hot, nothing crunchy, nothing that requires significant jaw movement. You’re protecting the graft while it begins initial integration with surrounding tissue.
Oral hygiene changes completely during this phase. You cannot brush the surgical sites. I provide a prescription antimicrobial rinse that you’ll use gently – no vigorous swishing – to keep the area clean without mechanical disruption. The rest of your mouth gets brushed normally, just avoiding the grafted areas entirely.
Days 3 Through 7 – Stabilization Period
Swelling peaks around day three, then begins subsiding. Discomfort decreases noticeably as the tissue starts healing. You’ll still maintain the soft food diet, though you can gradually add foods that require slightly more chewing if they don’t contact the surgical sites.
The graft tissue might appear white or yellowish during this phase – that’s normal healing, not infection. The tissue is integrating with the blood supply from surrounding areas, and the color indicates healthy fibrin formation. Some patients worry about the appearance, but this discoloration resolves as healing progresses.
You’ll continue using the antimicrobial rinse and avoiding brushing the grafted areas. The palate donor site typically feels better by the end of this week, though the graft itself remains tender to touch.
Week Two – Transition to Normal Function
By day 10 to 14, most patients return for suture removal. The tissue has integrated enough that sutures are no longer needed to maintain position. After suture removal, you can begin gentle brushing of the grafted areas with an ultra-soft toothbrush. The tissue is still healing and requires gentle care, but normal oral hygiene resumes gradually.
Diet restrictions ease significantly. You can eat most foods, though extremely crunchy or hard items should wait another week or two. The palate donor site is typically healed enough that it no longer limits your eating choices.
Following gum grafting instructions closely during the first two weeks significantly improves healing outcomes.
Weeks Three Through Six – Maturation Phase
The graft continues maturing and integrating with surrounding tissue. Color match improves as blood supply becomes fully established. Sensitivity decreases progressively as the tissue thickens and stabilizes. You’ll return to completely normal brushing and eating during this period.
Final results become apparent around the three-month mark. The tissue has fully matured, color has normalized, and you can see the actual amount of root coverage achieved. Some recession areas achieve complete coverage, while others gain partial coverage – the outcome depends on initial recession severity, tissue quality, and your healing response.
The Results You Can Expect: Function and Aesthetics

Successful gum grafting delivers measurable improvements in both how your mouth functions and how your smile appears. The sensitivity that stopped you from enjoying cold drinks diminishes within weeks as the newly grafted tissue covers previously exposed roots. That coverage creates a protective barrier between temperature changes and the nerve endings that caused sharp pain.
Root coverage varies by individual factors – the amount of recession present before treatment, the quality of your tissue, your healing capacity, and the specific technique used. Complete coverage happens in many cases, particularly when recession is moderate and tissue quality is good. Severe recession might achieve 70 to 80 percent coverage rather than 100 percent, but even partial coverage significantly reduces sensitivity and protects against further recession.
The aesthetic improvement addresses what many patients found most troubling about their recession – the appearance of longer teeth, visible root surfaces, and an uneven gum line. Grafted tissue blends with existing gums, creating a more uniform appearance across your smile. Front teeth recession correction makes the biggest visual impact, restoring the balance between tooth and gum that defines an attractive smile.
Beyond immediate results, gum grafting provides long-term protection. The grafted tissue is typically thicker and more resistant to future recession than the thin tissue that was there before. This thickness creates a buffer against brushing trauma, periodontal disease progression, and mechanical forces that caused the original recession. Gum grafting protects exposed roots and helps preserve the bone that supports your teeth.
Bone preservation represents another crucial outcome. When gums recede, bone follows. By restoring gum coverage, you’re protecting the underlying bone from continued loss. This matters tremendously for long-term tooth stability – adequate bone support keeps teeth firmly in place and maintains your bite function for years.
The tissue continues improving even after the three-month mark. Minor refinements in contour and color happen over six to twelve months as the graft fully matures. What you see at three months is close to final results, but subtle improvements continue as the tissue completes its integration with your natural anatomy.
Why Experience Matters in Gum Grafting Outcomes
Gum grafting is technique-sensitive. The difference between adequate results and excellent outcomes often comes down to surgical precision, tissue handling expertise, and detailed attention to positioning during the procedure.
Tissue harvesting requires understanding palate anatomy and knowing exactly how much tissue to take and from which location. Too little tissue and the graft won’t provide adequate coverage. Too much trauma to the donor site and recovery becomes unnecessarily difficult. The harvesting technique I use minimizes palate discomfort while securing tissue of optimal thickness and quality.
Graft positioning determines coverage outcomes. The tissue must lay flat against the root surface without gaps or folds. It needs adequate blood supply from surrounding tissue to survive and integrate. Suturing technique holds the graft in proper position during the critical first week when movement could compromise results.
Choosing a provider experienced in gum grafting reduces complications and improves long-term success. At Optima Dental Surgery Center, our approach to gum grafting combines surgical expertise with patient education and support throughout recovery. We explain what you’ll experience during each healing phase, provide detailed care instructions, and remain available when questions arise. You’re not managing recovery alone – you have direct access to our team when you need guidance or reassurance.
If you’re dealing with gum recession, sensitivity, or aesthetic concerns from exposed roots, schedule a consultation. We’ll assess your specific situation, explain which grafting technique fits your needs, and give you realistic expectations for outcomes and recovery. The recession won’t reverse on its own. But with proper treatment, you can restore coverage, reduce sensitivity, and protect your long-term oral health.
Remember: When performed at the right time, gum grafting can halt progression and restore stability before permanent damage occurs. Call our office or request a consultation. Let’s address the recession before it progresses further.
Gum Grafting: Common Questions About Treatment, Recovery, and Results
What is gum grafting and why is it recommended?
Gum grafting is a surgical procedure used to restore lost gum tissue and cover exposed tooth roots. It is recommended to reduce sensitivity, protect roots from decay, and prevent further gum and bone loss.
When is gum grafting necessary?
Gum grafting becomes necessary when recession is progressing, causing root exposure, sensitivity, aesthetic concerns, or increased risk of decay and tooth instability.
What types of gum grafting procedures are available?
The main types of gum grafting include connective tissue grafts, free gingival grafts, and pedicle grafts. The right option depends on recession severity, tissue thickness, and treatment goals.
Is gum grafting painful?
Most patients report mild to moderate discomfort after gum grafting, primarily from the donor site. Pain is temporary and typically well managed with medication and proper post-operative care.
How long does it take to recover from gum grafting?
Initial healing from gum grafting occurs within two weeks, with full tissue maturation taking several months. Most patients return to normal activities within a few days.
How long do gum grafting results last?
With good oral hygiene and proper brushing habits, gum grafting results can last for decades. The grafted tissue is usually thicker and more resistant to future recession.