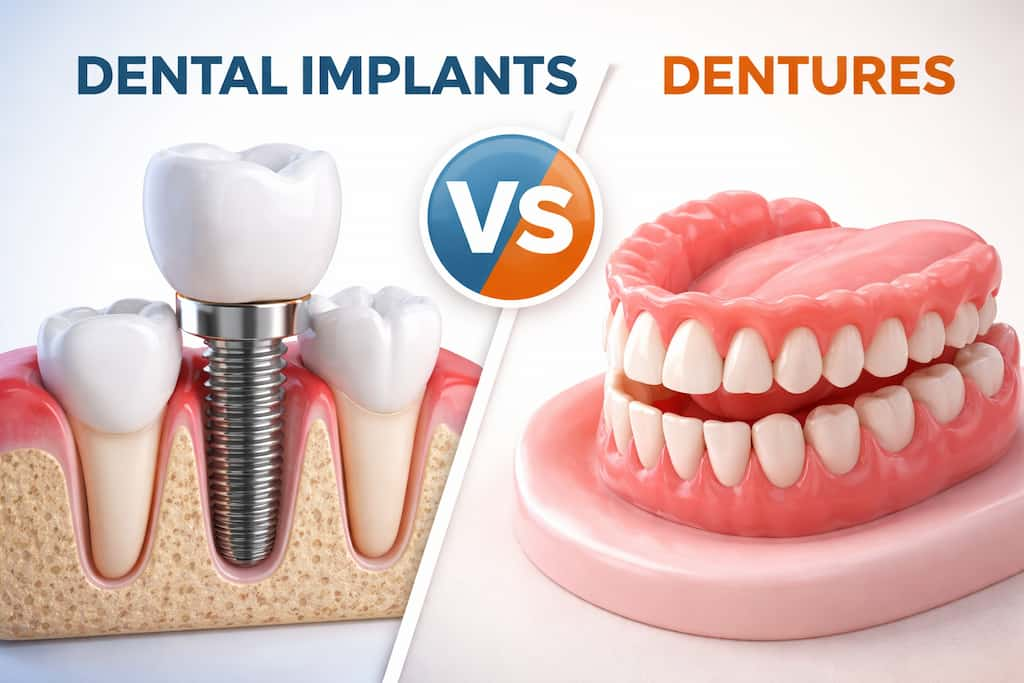
You’ve spent months researching dental implants, convinced they’re the solution you need. Then the doubt creeps in – what if your bone loss is too severe, your diabetes disqualifies you, or your age works against you? You start wondering if you’re even a candidate, if consultation would waste everyone’s time, if you should just accept dentures as your only option. At this stage, most people are really asking the same core question: can anyone get dental implants, or are there limits that apply to them personally?
I know this anxiety because I evaluate implant candidacy daily. Most patients arrive expecting disqualification, already preparing for disappointment. They’ve diagnosed themselves based on internet research, convinced some factor makes them ineligible. The reality is more nuanced – while not everyone qualifies for dental implants immediately, many patients who initially seem poor candidates can become qualified through corrective procedures or medical management. Understanding whether or not can anyone get dental implants depends on identifying which factors are temporary barriers and which are true limitations.
Here’s what actually determines dental implant candidacy – the core requirements that matter, the health conditions that affect eligibility and how they’re managed, the bone loss solutions that restore qualification, and the lifestyle factors you can control to improve your chances. This isn’t about false hope or dismissing legitimate obstacles. This is about understanding where you actually stand and what options exist when initial assessment reveals challenges.
The Core Requirements for Dental Implant Candidacy

Dental implant candidacy depends on multiple factors working together. When patients ask, “can anyone get dental implants,” these requirements are what ultimately determine the answer. Meeting all requirements creates optimal conditions for success, while deficiencies in certain areas either prevent placement or require corrective procedures first.
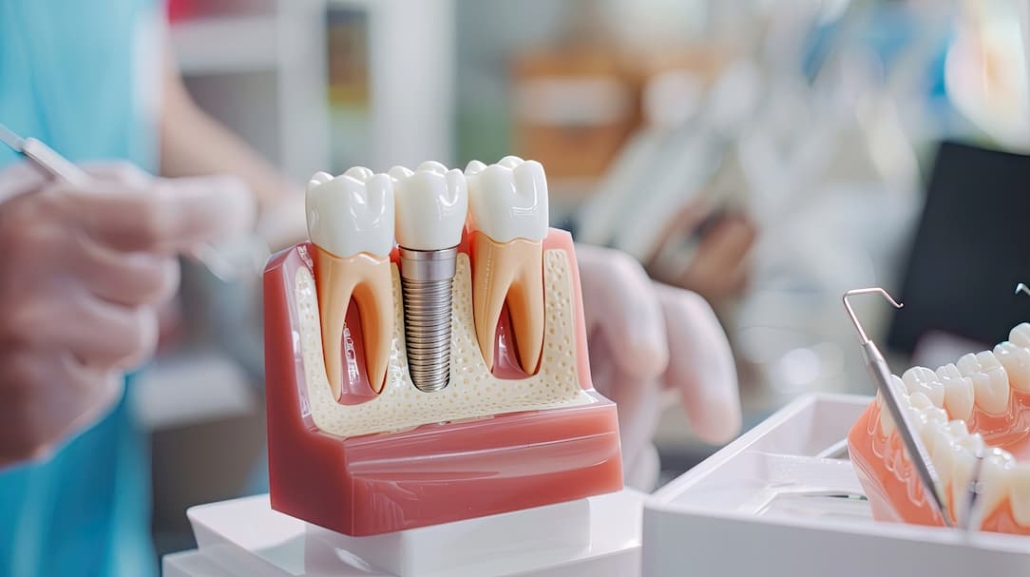
- Adequate bone volume and density – implants need sufficient bone height, width, and quality for stability; bone must be dense enough to support titanium posts
- Healthy gum tissue – active periodontal disease requires treatment before placement; healthy tissue provides foundation for long-term success
- Controlled systemic health conditions – diabetes, autoimmune disorders, and other issues need medical management to acceptable levels; uncontrolled conditions impair healing
- Healing capacity – your body must integrate titanium with bone through osseointegration; smoking, certain medications, and radiation can impair this process
- Commitment to oral hygiene – implants require consistent cleaning and maintenance; inadequate hygiene increases failure risk from peri-implantitis
- Realistic expectations – understanding treatment timeline, commitment required, and anticipated outcomes matters for satisfaction
Most candidacy obstacles can be addressed. Insufficient bone gets augmented through grafting. Periodontal disease receives treatment. Systemic conditions get optimized with physicians. The question isn’t usually “Can I ever get implants?” but rather “What needs to happen first?”
Health Conditions That Affect Candidacy

Certain medical conditions influence implant success rates and healing capacity. This is why the question can anyone get dental implants is less about having a diagnosis and more about how well that condition is managed. Understanding how these conditions affect candidacy helps you assess your situation realistically.
Diabetes – controlled diabetes (A1C below 7.0) typically doesn’t prevent placement. Well-managed diabetes shows success rates comparable to non-diabetic patients. Uncontrolled diabetes (A1C above 8.0) requires medical optimization first.
Autoimmune disorders – conditions like rheumatoid arthritis or lupus can affect healing. Many patients with well-controlled autoimmune conditions successfully receive implants. Consideration focuses on whether immunosuppressive medications impair healing significantly.
Osteoporosis and bone medications – osteoporosis itself doesn’t prevent implants. However, bisphosphonate medications create osteonecrosis risk. Oral bisphosphonates might require drug holidays; IV bisphosphonates need careful evaluation.
Heart conditions and blood thinners – most patients on blood thinners can undergo surgery without stopping medications. Certain heart conditions require antibiotic prophylaxis. Coordination with your cardiologist ensures safe management.
Cancer treatment history – radiation to head and neck significantly increases failure risk in radiated areas. Adequate healing time post-radiation – often six months to a year – is needed. Most patients can proceed after chemotherapy completion and recovery.
Smoking – dramatically increases failure rates. Nicotine impairs healing and reduces osseointegration success. Smokers face roughly double the failure rate. Cessation for at least two weeks before and after surgery is typically required.
Controlled Conditions vs Disqualifying Factors
“Controlled” means the condition is managed to levels that don’t significantly compromise healing. For most patients, controlled conditions mean the answer to “can anyone get dental implants” is often yes—with preparation. For diabetes, that typically means A1C below 7.0 with stable glucose levels. For autoimmune conditions, it means disease activity is minimal and medication side effects don’t severely impair healing capacity.
Medical clearance from your treating physician documents that your condition is adequately managed for surgical procedures. This clearance isn’t just paperwork – it’s confirmation that proceeding with surgery presents acceptable risk given your current health status.
Some medications require adjustment timing. Blood thinners might continue through surgery with modified protocols, or your cardiologist might approve brief interruption. Bisphosphonates might need temporary discontinuation – a drug holiday – to reduce osteonecrosis risk. These decisions happen through coordination between your medical team and surgical team.
Timeline considerations matter with health optimization. Bringing uncontrolled diabetes into good control might take several months. Completing necessary medication adjustments adds time to your treatment timeline. This delay protects your investment and your health – proceeding before adequate optimization increases failure risk substantially.
Truly disqualifying factors are rare. Active cancer treatment, severe uncontrolled systemic disease, recent heart attack or stroke, or complete inability to heal represent situations where implant surgery isn’t appropriate. Even some of these become manageable after adequate recovery time and medical stabilization.
Bone Loss Solutions That Restore Candidacy
Insufficient bone volume represents the most common candidacy obstacle – and the most correctable one. Multiple techniques restore bone to levels that support successful implant placement. Bone loss alone rarely means the answer to can anyone get dental implants is no.
Bone grafting augments areas with inadequate height or width. Material integrates with existing bone over several months, then provides volume for implant placement. Minor grafting can happen with implant placement; substantial grafting requires healing time first.
Sinus lifts address bone loss in upper back jaw where sinus cavity limits bone height. The procedure lifts the sinus membrane and places graft material underneath. Success rates exceed 95 percent with proper technique.
Ridge augmentation rebuilds jaw width lost over years of tooth absence. Various techniques widen the ridge to accommodate implants properly based on deficiency severity.
Zygomatic implants provide solutions for severe upper jaw bone loss. These longer implants anchor in the cheekbone, bypassing areas of severe resorption. They allow immediate restoration without extensive grafting.
Timeline from grafting to implant placement varies – minor grafting heals in three to four months, major grafting might require six months or more. Adequate healing time protects your investment and maximizes success probability.
Age Considerations: When You’re “Too Young” or “Too Old”

Age creates candidacy questions at both ends of the spectrum. The answers are more straightforward than most patients expect. Age by itself almost never determines whether can anyone get dental implants applies to you.
Minimum age requirements exist because jaw growth must be complete before implant placement. Placing implants in growing jaws creates problems as the bone continues developing around fixed implant positions. For most patients, jaw growth completes around age 18 for females and age 21 for males. Younger patients who’ve lost teeth due to trauma or congenital absence need temporary solutions – bridges, partial dentures, or other options – until they reach appropriate age for implant placement.
There is no maximum age limit for dental implants. I’ve successfully placed implants in patients in their eighties and nineties. Chronological age matters far less than physiological health and healing capacity. An active, healthy 85-year-old with well-controlled health conditions often makes a better implant candidate than a 60-year-old with uncontrolled diabetes and poor healing capacity.
The relevant considerations for older patients focus on healing ability, systemic health status, and life expectancy relative to treatment investment. A patient in their seventies or eighties with good health and reasonable life expectancy benefits tremendously from implants – improved nutrition, better quality of life, and enhanced dignity during their remaining years. The treatment timeline matters less when you’re not working against age-related limitations but rather optimizing remaining life quality.
Older patients sometimes face more extensive bone loss simply due to longer time periods with missing teeth. This bone loss responds to grafting just as it does in younger patients. The healing might take slightly longer in older individuals, but outcomes remain predictable when health status is good.
The decision about implant treatment in older patients balances realistic assessment of health status, healing capacity, and personal goals against the investment of time and money. Many older patients tell me they wish they’d done it years earlier. Very few regret the decision to proceed with implant treatment in their later years.
The CT Scan Assessment: What It Reveals About Your Candidacy
Three-dimensional CT imaging provides the definitive assessment of your implant candidacy. This scan reveals information that clinical examination and standard x-rays cannot capture.
The scan shows bone quality and quantity in precise detail. I can measure exact bone height, width, and density at each potential implant site. This measurement determines whether existing bone is adequate, whether minor grafting at the time of implant placement will suffice, or whether staged grafting procedures need to precede implant placement.
Nerve and sinus position mapping prevents complications. The CT reveals where the inferior alveolar nerve runs through the lower jaw and how close the maxillary sinuses sit to potential implant sites in the upper jaw. This anatomical information guides surgical planning to avoid nerve injury and determine sinus lift necessity.
Density measurements from the CT predict how well bone will support implants and how quickly osseointegration should occur. Dense bone provides excellent stability but might require modified surgical technique. Soft bone requires specific implant designs and sometimes extended healing periods for adequate integration.
The scan guides surgical approach decisions. It shows whether conventional implants will work, whether angled implants optimize available bone, or whether alternative approaches like zygomatic implants make sense. This planning happens before surgery, eliminating surprises and allowing informed decision-making.
CT imaging reveals how much grafting you need if bone is deficient. Small deficiencies might require minimal grafting that adds little time to your treatment. Substantial deficiencies necessitate more extensive grafting with longer healing periods. Knowing this upfront provides realistic timelines and cost projections.
The scan is the first step in evaluation for good reason – it provides objective data about your actual anatomy and bone status. Online questionnaires and generic assessments can’t replace this individualized anatomical evaluation. Your specific bone quantity, quality, and anatomical relationships determine your candidacy and treatment approach.
Lifestyle Factors You Can Control to Improve Candidacy

While you cannot change your bone anatomy or genetics, several modifiable factors significantly impact implant candidacy and success rates. These modifiable factors often change the answer to can anyone get dental implants more than patients realize.
Smoking cessation timeline matters tremendously. Quitting tobacco use at least two weeks before surgery and remaining tobacco-free throughout healing dramatically improves outcomes. The longer you abstain, the better – patients who quit permanently show success rates approaching non-smokers. Even reducing smoking helps, though complete cessation provides optimal results. If you smoke and want implants, quitting represents the single most impactful change you can make.
Oral hygiene optimization before implant placement establishes habits necessary for long-term success. Address existing dental problems – cavities, gum disease, failing restorations. Develop consistent brushing and flossing routines. These habits protect your implant investment after placement and demonstrate the commitment necessary for maintenance.
Nutrition for healing supports tissue repair and bone integration. Adequate protein intake provides building blocks for new tissue. Sufficient calcium and vitamin D support bone health. Avoiding excessive alcohol consumption improves healing capacity. These dietary modifications matter most during the healing phases but benefit long-term implant success when maintained.
Medication management with physicians optimizes your health status for surgery. Work with your primary care doctor to achieve best possible control of diabetes, blood pressure, and other conditions. Discuss medication adjustments that might improve healing. This coordination takes time but substantially improves outcomes.
Weight and diabetes control interconnect – weight loss often improves glucose management in diabetic patients. Even modest weight reduction can bring A1C levels into acceptable ranges for surgery. The effort invested in health optimization pays dividends beyond implant success.
These lifestyle modifications require effort and commitment. But they’re entirely within your control, unlike bone anatomy or genetic factors. Patients who address modifiable risk factors before treatment show substantially better outcomes than those who proceed without optimization.
Financial Qualification vs Medical Qualification
Candidacy assessment separates medical eligibility from financial capacity. These are distinct considerations that sometimes get confused during initial research and planning.
Medical qualification determines whether implant treatment can succeed given your anatomy, health status, and healing capacity. Financial qualification addresses whether you can afford the treatment investment. Meeting medical requirements doesn’t guarantee you can afford treatment, and having financing available doesn’t override medical limitations.
Financing options exist to make treatment accessible to qualified candidates. Payment plans, healthcare credit companies, and various financing structures help manage costs over time. These options address affordability but don’t change your medical candidacy status – you still need adequate bone, controlled health conditions, and healing capacity regardless of how you pay.
Transparent cost discussion happens early in the evaluation process. You need to know what treatment will cost, whether grafting or other preparatory procedures add expense, and what financing options exist. This transparency prevents proceeding through evaluation only to discover affordability obstacles at the end.
At Optima Dental Surgery Center, we discuss both aspects clearly – whether you medically qualify for implants, and what investment is required for your specific situation. Medical candidacy gets assessed through examination and imaging. Financial planning happens through detailed cost breakdown and financing discussion. Both conversations matter, but they address different aspects of your decision.
Some patients medically qualify but decide treatment doesn’t fit their financial priorities currently. Others discover they need preparatory procedures that increase investment beyond initial expectations. These are legitimate considerations separate from whether you can physically receive and maintain implants successfully.
The Consultation Process: Getting Your Personal Answer

Generic candidacy information helps you understand general requirements, but only individual evaluation determines your specific status and options.
During consultation, we review your medical history, current health status, and medications. Clinical examination assesses oral health, gum tissue quality, and preliminary bone evaluation. CT imaging when indicated provides precise anatomical data about your bone and surrounding structures.
We discuss your specific situation honestly – whether you qualify immediately, whether preparatory procedures would make you a candidate, or whether obstacles exist that can’t be adequately addressed.
Key questions to ask: Do I qualify with my current health status? What preparatory procedures do I need? What’s the complete timeline? What’s the total investment including grafting? How do my health conditions affect success probability?
The timeline from consultation to treatment varies substantially based on your situation. Straightforward cases might proceed within weeks. Cases requiring grafting, health optimization, or medical coordination might span months before implant placement. Understanding this timeline upfront prevents frustration with necessary preparatory phases.
Generic online assessments cannot replace individual evaluation. Your specific anatomy, bone quality, health status, and treatment goals create a unique situation that requires personalized assessment. Two patients with similar medical histories might have completely different candidacy status based on bone volume or other anatomical factors.
If you’re wondering whether you qualify for dental implants, schedule a consultation at Optima Dental Surgery Center. Ultimately, can anyone get dental implants can only be answered accurately after a personalized clinical evaluation. We’ll evaluate your specific situation through examination and imaging, discuss any obstacles and corrective options, and provide honest assessment of your candidacy. Contact our office to begin the evaluation process and get definitive answers about your implant options.
Can Anyone Get Dental Implants? Common Questions About Eligibility and Candidacy
Can anyone get dental implants, or are some people automatically disqualified?
Not everyone qualifies immediately, but very few people are permanently disqualified. Most candidacy issues—such as bone loss or medical conditions—can be addressed with preparatory treatment or medical optimization.
Can anyone get dental implants if they have diabetes?
Patients with well-controlled diabetes often qualify for implants with success rates similar to non-diabetic patients. Uncontrolled diabetes usually requires better medical management before surgery.
Can anyone get dental implants if they have bone loss?
Bone loss does not automatically prevent implant treatment. Bone grafting, sinus lifts, and alternative implant techniques can often restore eligibility.
Can anyone get dental implants if they smoke?
Smoking significantly increases implant failure risk, but it does not always disqualify patients. Quitting smoking before and after surgery greatly improves outcomes.
Can anyone get dental implants at an older age?
There is no upper age limit for dental implants. Overall health and healing capacity matter far more than chronological age.
Can anyone get dental implants without a CT scan?
A CT scan is essential for determining candidacy. It provides detailed information about bone quantity, density, and anatomical structures that cannot be evaluated with standard exams alone.